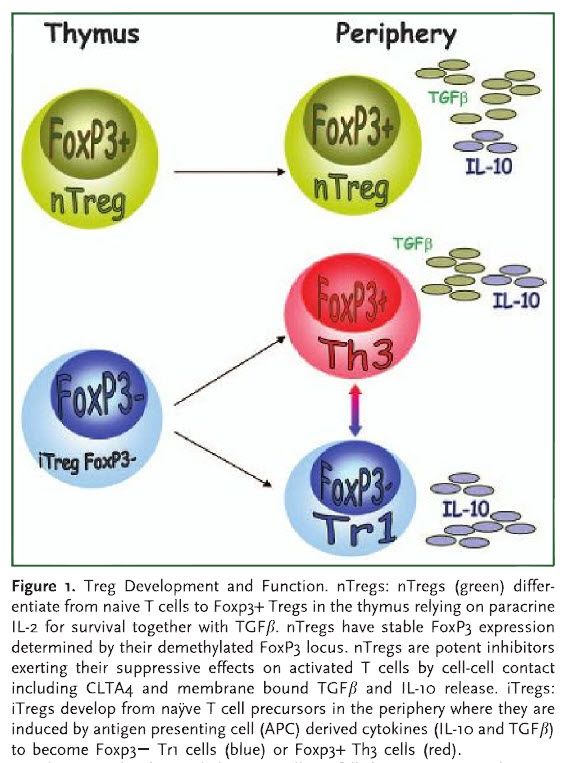
To review what is now known about regulatory T-cells, there are two basic types: Natural Tregs (nTregs) which are developed in the thymus and induced Tregs (iTregs) which are developed outside of the thymus.
nTregs seem to have the feature of preventing autoimmunity from occuring in the first place.
iTregs seem to migrate to sites of inflamation and shut-down an immune response at the appropriate time (see previous post on how this occurs) to prevent the response from getting out of control which could lead to autoimmunity.
Here is a good overview of the differences from the following paper:
 http://www.ncbi.nlm.nih.gov/pubmed/20402669
http://www.ncbi.nlm.nih.gov/pubmed/20402669
The important thing to note is that autoimmunity seems to be caused by a defect in nTregs.
How does Vitamin D play a role in this?
It appears that Vitamin D promotes the development of iTregs which can in effect shut-down an autoimmune response at the site of imflamation. In particular, it seems to promote the Tr1 class of regulatory t-cells which produce the anti-inflamitory cytokine (chemical signal) IL-10. Here is a recent high dosage study that demonstrates this:
http://www.ncbi.nlm.nih.gov/pubmed/21179201
Conclusion/Significance: Twelve week supplementation of high dose vitamin D3 in RRMS patients was well tolerated and
did not induce decompensation of calcium metabolism. The skewing towards an anti-inflammatory cytokine profile
supports the evidence on vitamin D as an immune-modulator, and may be used as outcome measure for upcoming
randomized placebo-controlled trials.
Therefore, we speculate that the rise in IL-10+CD4+ T cells might
reflect expansion of inducible regulatory Tr1 cells. The finding of
an altered profile of pro- and anti-inflammatory CD4+ T cells
conforms to observations in experimental studies [5] and further
supports the assessment of vitamin D3 as a natural immune
modulator in MS [3].
To paraphrase, the amount of Tr1 anitinflamitory regulatory t-cells found in the high vitamin D group is nearyly double that of that found in the control group.
Also, recently there was published another high dose Vitamin D paper which I have provided a link here:
http://www.neurology.org/content/77/17/1611
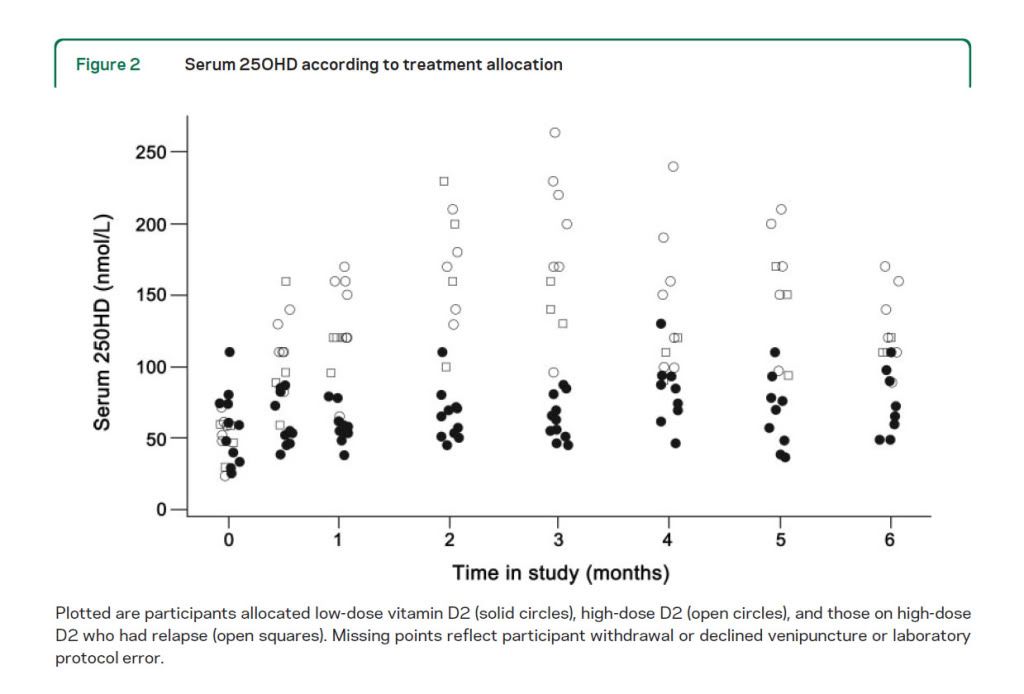
Results: Twenty-three people were randomized, of whom 19 were on established interferon or glatiramer acetate (Copaxone) treatment. Median 25OHD rose from 54 to 69 nM (low-dose D2) vs 59 to 120 nM (high-dose D2) (p = 0.002). No significant treatment differences were detected in the primary MRI endpoints. Exit EDSS, after adjustment for entry EDSS, was higher following high-dose D2 than following low-dose D2 (p = 0.05). There were 4 relapses with high-dose D2 vs none with low-dose D2 (p = 0.04).
Conclusion: We did not find a therapeutic advantage in RRMS for high-dose D2 over low-dose D2 supplementation.
However, this study did not evaluate objective parameters such as increases in Tr1 cells but only looked at more subjective measures such as relapse rate.
But it seems to me from everything I have read, Vitamin D will not stop MS. However, one thing it may do is reduce the relapse severity/frequency. This is what I have experienced, but my case is of course anecdotal. I believe the only way to stop MS is by the HSCT protocal which will re-set your immune system back to self tolerance.
One thing that is still not clear though when comparing the different vitamin D trials is the dosage.
The report from the above paper which found no significant benefit of high dose vitamin D maintained a vitamin D level in the range of 130–175 nM 25OHD.
However, the other high dosage study cited above (20,000 IU/day) had a significantly higher serum level without having any ill effects such as hypercalcemia:
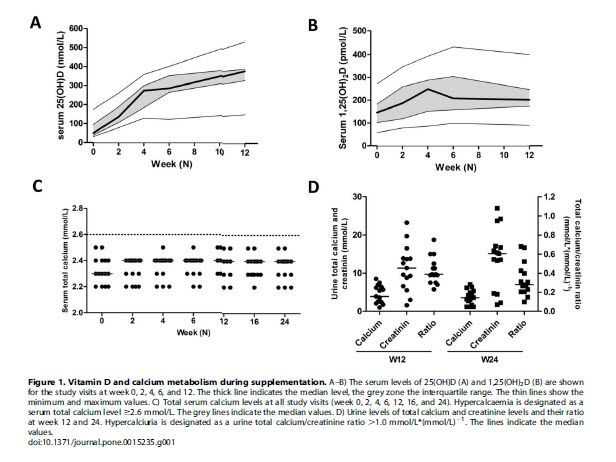
This is also the case for the Burton study shown in a previous post with a maximum dose of 40,000 IU/day and average dose of 15,000 IU/day.
Both of these later studies evaluated the T-cell profile and found an anit-inflamitory results.
So, I really don't believe that science yet knows what the optimun levels for vitamin D is in humans. Most of the guidelines are for bone health and the actual amount to maintain a healthy immune system may be much higher. Here is a good desciption of this:
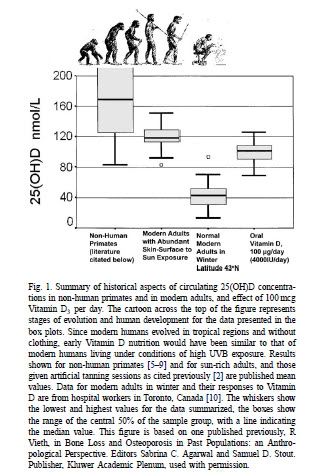 http://www.ncbi.nlm.nih.gov/pubmed/15225842
http://www.ncbi.nlm.nih.gov/pubmed/15225842