New theory of MS
Posted: Sat Nov 27, 2010 10:14 am
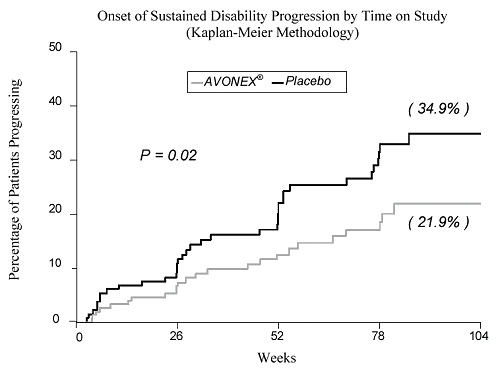
The abstract below describes another new way of classifying MS. I like it because it blasts EAE right off the top. On the other hand their condemnation of immunosuppression seems too broad to me since there are some successes on that front (campath etc.) Also, their comments about the placebo effect and the existing therapies (CRABs) seems strange. It's repeating an oft-mentioned misunderstanding that they are no better than placebo when they are actually 30% better than placebo in double-blind placebo controlled trials. Anyhow, still interesting...
The sad plight of multiple sclerosis research (low on fact, high on fiction): critical data to support it being a neurocristopathy.
Inflammopharmacology. 2010 Sep 24. [Epub ahead of print]
Behan PO, Chaudhuri A.
Department of Neurology, Institute of Neurological Sciences, Glasgow University, Glasgow, Scotland, UK, pob1w@clinmed.gla.ac.uk.
The literature for evidence of autoimmunity in multiple sclerosis (MS) is analysed critically.
In contrast to the accepted theory, the human counterpart of the animal model experimental autoimmune demyelinating disease, experimental allergic encephalomyelitis (EAE), is not MS but a different demyelinating disorder, i.e. acute disseminated encephalomyelitis and acute haemorrhagic leucoencephalitis. Extrapolation of EAE research to MS has been guided largely by faith and a blind acceptance rather than sound, scientific rationale.
No specific or sensitive immunological test exists that is diagnostic of MS despite the extensive application of modern technology. Immunosuppression has failed to have any consistent effect on prognosis or disease progression. The available data on MS immunotherapy are conflicting, at times contradictory and are based on findings in animals with EAE. They show predominantly a 30% effect in relapsing/remitting MS which suggests powerful placebo effect.
Critical analysis of the epidemiological data shows no association with any specific autoimmune diseases, but does suggest that geographic factors and age at development posit an early onset possibly dependent on environmental influences. Certain neurological diseases are, however, found in association with MS, namely hypertrophic peripheral neuropathy, neurofibromatosis-1, cerebral glioma, glioblastoma multiforme and certain familial forms of narcolepsy. These share a common genetic influence possibly from genes on chromosome 17 affecting cell proliferation. A significant number of these disorders are of neural crest origin, the classical example being abnormalities of the Schwann cell.
These and other data allow us to propose that MS is a developmental neural crest disorder, i.e. a cristopathy, implicating glial cell dysfunction with diffuse blood-brain barrier breakdown. The data on transcription factor SOX10 mutations in animals may explain these bizarre clinical associations with MS and the phenotypic variability of such alterations (Cossais et al. 2010). Research directed to the area of neural crest associations is likely to be rewarding.
http://www.ncbi.nlm.nih.gov/pubmed/20862553
The sad plight of multiple sclerosis research (low on fact, high on fiction): critical data to support it being a neurocristopathy.
Inflammopharmacology. 2010 Sep 24. [Epub ahead of print]
Behan PO, Chaudhuri A.
Department of Neurology, Institute of Neurological Sciences, Glasgow University, Glasgow, Scotland, UK, pob1w@clinmed.gla.ac.uk.
The literature for evidence of autoimmunity in multiple sclerosis (MS) is analysed critically.
In contrast to the accepted theory, the human counterpart of the animal model experimental autoimmune demyelinating disease, experimental allergic encephalomyelitis (EAE), is not MS but a different demyelinating disorder, i.e. acute disseminated encephalomyelitis and acute haemorrhagic leucoencephalitis. Extrapolation of EAE research to MS has been guided largely by faith and a blind acceptance rather than sound, scientific rationale.
No specific or sensitive immunological test exists that is diagnostic of MS despite the extensive application of modern technology. Immunosuppression has failed to have any consistent effect on prognosis or disease progression. The available data on MS immunotherapy are conflicting, at times contradictory and are based on findings in animals with EAE. They show predominantly a 30% effect in relapsing/remitting MS which suggests powerful placebo effect.
Critical analysis of the epidemiological data shows no association with any specific autoimmune diseases, but does suggest that geographic factors and age at development posit an early onset possibly dependent on environmental influences. Certain neurological diseases are, however, found in association with MS, namely hypertrophic peripheral neuropathy, neurofibromatosis-1, cerebral glioma, glioblastoma multiforme and certain familial forms of narcolepsy. These share a common genetic influence possibly from genes on chromosome 17 affecting cell proliferation. A significant number of these disorders are of neural crest origin, the classical example being abnormalities of the Schwann cell.
These and other data allow us to propose that MS is a developmental neural crest disorder, i.e. a cristopathy, implicating glial cell dysfunction with diffuse blood-brain barrier breakdown. The data on transcription factor SOX10 mutations in animals may explain these bizarre clinical associations with MS and the phenotypic variability of such alterations (Cossais et al. 2010). Research directed to the area of neural crest associations is likely to be rewarding.
http://www.ncbi.nlm.nih.gov/pubmed/20862553