some thoughtsPrague Med Rep. 2012;113(4):289-93.
Serious Complication of Percutaneous Angioplasty with Stent Implantation in so Called "Chronic Cerebrospinal Venous Insufficiency" in Multiple Sclerosis Patient.
Doležal O, Horáková D, Gdovinová Z, Szilasiová J.
Department of Neurology and Center of Clinical Neuroscience, First Faculty of Medicine, Charles University in Prague and General University Hospital in Prague, Prague, Czech Republic.
Abstract
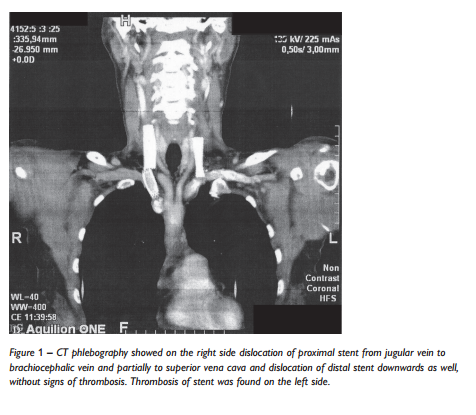
We report female patient, age 51, with clinically definitive multiple sclerosis (CDMS) since 1998, who underwent two PTA procedures with stent implantation for CCSVI in 2010. Expanded disability status scale (EDSS) worsened since the procedure from 4.5 to 6. Total number of three stents was implanted (two of them in the right internal jugular vein). In six month time, in 2011, patient was referred for independent examination by computer tomography (CT) phlebography for right-sided neck pain. Dislocation of stents on the right side and thrombosis of left sided stent was found. Conservative approach was used so far. Our short report is showing possible complications of PTA and stenting in jugular veins in so called CCSVI and bringing information about neurological state (EDSS) worsening in a subject. Continuation of stent migration in the future is probable, possibly resulting in pulmonary embolism with fatal risk for the patient. We strongly ask for restriction of PTA procedure in so called CCSVI, which concept was not proven to be relevant to MS.
There are some specific situations that warrant the use of stents in CCSVI, but these situations are rare. For this patient, the stents worsened the outflow.
When the doctors discovered the thrombosed stent and the migrated stent, they did nothing ("conservative care"). It may have been possible to recanalize the vein.
The authors say that continued migration of the stent is probable, which may possibly result in fatal pulmonary embolism. But my understanding is that a stent will endothelize into the vein wall within weeks of implantation. Although this stent migrated, it will not migrate further, if it is correct that it has endothelized. There are patients who live in fear of their stents migrating even a year or two after the procedure. My understanding is that this is a risk only in the first few weeks. After that the stent is a part of the vein wall itself.
The conclusion is that the authors strongly ask for restriction of PTA angioplasty in CCSVI. But what was done in this patient was not PTA. It was stenting. The outcome for this patient with stents, which is terrible, does not inform about the outcome of patients with ballooning only.
In this patient, new outflow obstructions were introduced into the veins in the form of these failed stents. When new outflow obstructions happened, the patient's EDSS deteriorated. This is only a single case study but it supports the hypothesis that extracranial outflow obstructions have negative consequences for patients with MS.
The abstract says that the full text is available but I cannot find the full text. If the right jugular stent migrated so that is blocking some of the confluence with the subclavian vein, there might be retrograde flow in the subclavian, which might then reroute up and into the jugular or the other neck veins, which would further worsen the outflow.
I do not know how such a flow situation could be helped. Vein grafting, where the entire jugular vein is subsected, has not shown a good outcome but jugular patch angioplasty may provide a better outcome. But there are no veins to patch if both are blocked with stents, nor is there a way to help the subclavian if it is partially blocked by a migrated stent, which is an assumption. Vertebral vein patch angioplasty would be the only contender and that is too risky a thought because those veins are typically smaller.