Today I treated a 38 year old North American woman who consulted with me about pelvic congestion syndrome recently diagnosed by CT angiogram, done in an emergency department because of pelvic pain, that showed a dilated ovarian vein opacifying a venous plethora in the pelvis.
I share this case because this patient's medical history resembles that of a prior patient, whose pelvic congestion was treated endovascularly while neglecting to stent a renal vein compression. The result was a variety of symptoms that I often see in patients with Multiple Sclerosis, such as fatigue, heat intolerance, cognitive impairment, imbalance. These symptoms completely resolved with stenting of the renal vein. It was ultimately determined that the patient did not have MS. I thought it important to have discovered someone without MS who clearly developed classic ccsvi symptoms after occluding the ovarian vein by forcing all that renal venous blood into the vertebral plexus.
Now I have another patient with similar presentation, again without a diagnosis of MS. Today's patient complains of chronic fatigue, short term memory loss, tinnitus, left flank and back pain, tightness and spasm, heat intolerance, tinnitus, headaches, hematuria, nocturia, hesitancy and frequency and recently nausea. Sound familiar?
In the upright position, gravity tends to force blood up from the ovary using a series of valves that have one way flow toward the heart. The pelvic congestion syndrome results when blood is unimpeded in flowing downward into the pelvis. This occurs when the valve that normally allow one way flow toward the heart become incompetent. The resulting venous engorgement is associated with symptoms such as urinary blood or protein, pelvic pain, hemorrhoids, and fatigue. The recommended treatment is to block blood from descending into the pelvis by occluding the ovarian vein at its connecctions to other major pelvic veins.
The first step in treatment is to assess venous incompetency, determine anatomy and look for cause.
I performed left renal and ovarian venography and IVUS. This is best approached from the right jugular vein going down through the right atrium into the left renal vein. However, because of my suspicion of CCSVI, I chose to access the venous circulation through the right saphenofemoral junction. A bit of a challenge.
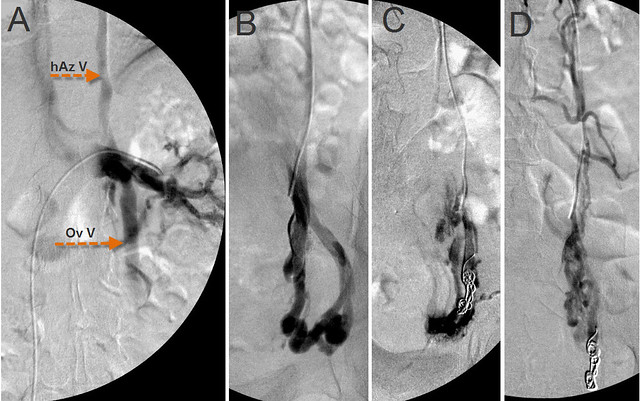
Figure 1 Treatment of Nutcracker Syndrome and pelvic congestion syndrome.
The catheter tip is in the distal renal vein. Venography (A) revealed obstruction of the left renal vein, reflux of the ovarian vein (Ov V) into the pelvis and reflux of the renal vein through the hemiazygo-renal anastomosis (hAz V) into intervertebral veins and the vertebral plexus.The renal vein contrast is markedly diminished where it is compressed by the aorta.
When a good catheter position was achieved, I used coiling and sclerotherapy to occlude proximally and distally, the incompetent ovarian vein at its pelvic anastomoses . (Figure 1 C&D) Sclerosis by sotradecol injures the endothelium and results in thrombosis.
After each step in this procedure, check venograms were performed. Control venograms were performed after each stage
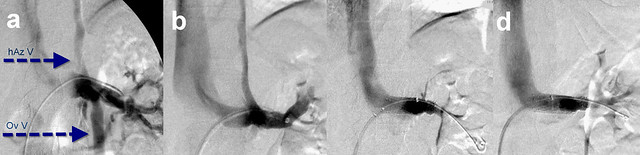
Figure 2. Nutcracker treatment
A. Pre-treatment venogram. For comparison, the pretreatment venogram (A) ishows significant reflux into hemiazygous (hAzV) and ovarian vein (Ov V). After completion of the embolization and sclerotherapy of the ovarian vein (B), one now fails to see any contrast media refluxing into the ovarian vein. However reflux into the spinal Figure 2B shows that ovarian vein treatment has been successful.. No ovarian reflux is seen. However there is reflux up the hemiazygous vein. The left renal vein flow is great, With loss of the ovarian vein as a decompressing outflow, that flow must now find new routes The likely one is the hemiazygous vein,which impacts the thoracic and spinal venous drainage.
To avoid this collateral pathway, the most reasonable approach is to improve direct renal venous outflow into the inferior vena cava. After deployment of two nickel/titanium self expanding stents, one sees no contrast flowing toward the spine; it is only see flowing directly into the IVC and the right atrium.
Because her symptom complex presented a picture similar to many patients with CCSVI, I performed supine and upright Duplex ultrasound by standard CCSVI protocol. This fufilled two criteria of CCSVI, namely supine and erect reflux and long, thickened immobile valves in the left Internal jugular vein
The patient agreed to undergo venography of the left internal jugular vein at the completion of the renal vein stenting.
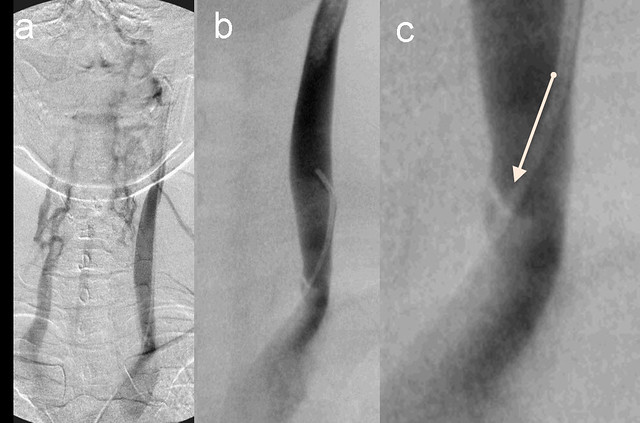
Figure 3. Internal Jugular vein valvular stenosis and reflux.
A. Left IJ Venogram showed reflux into condylar emissary , posterior cervical veins and contralaterl vertebral vein.
B. Lower jugular segment venogram shows stenosis of greater than 80 %stenosis. T
C. The zoom view shows an immobile medial valve (arrow)
This patient's medical history resembles that of a prior patient, whose pelvic congestion was treated endovascularly without stenting a renal vein compression. The result was a variety of symptoms that I often see in patients with Multiple Sclerosis, such as fatigue, heat intolerance, cognitive impairment, imbalance. These symptoms completely resolved with stenting of the renal vein. That patient did not have MS.
Today's patient complains of chronic fatigue, short term memory loss, tinnitus, left flank and back pain, tightness and spasm, Lower extremity swelling, stiff muscles and purple feet, heat intolerance, tinnitus, headaches, hematuria, nocturia, hesitancy and frequency and recently nausea. These are many of the symptoms that are commonly seen in MS and among those symptoms that are relieved by improvement in venous outflow obstructions. It is encouraging to note that the constant purple color of her feet and the tense heaviness of her legs are no longer present.. Of course, it is too soon to draw conclusions .
She is not a simple case. Rare disease is her middle name right now. She was diagnosed several years ago at Cleveland Clinic with postural orthostatic tachycardia syndrome, In addition she has mitral prolapse with mitral insufficiency as did her grandfather. In CCSVI . i am always focused on mitral prolapse in MS, thinking of Ehlers Danlos Syndrome. She does have early shoulder arthritis and many orthopedic injuries, prominent secondary palpebral fissures, easy bruisability, I think she needs to be tested. Further many of these symptoms are present in patients with MS. She needs to visit a neurologist as well.
This may very well be another case of CCSVI in a patient without MS. As such cases accumulate, evidence will mount that CCSVI is its own entity. Improvement of her symptoms may allow us to define symptoms that are specific to CCSVI.



