I'll look forward to it then.drsclafani wrote:it is difficult to present cases if there are none scheduled.
Today i treated two patients, both are incredible illustrations.
it takes quite a bit of time to prepare these cases but look forward to some tonite or tmorrow
DrSclafani answers some questions
-
Cece
- Family Elder
- Posts: 9335
- Joined: Mon Jan 04, 2010 3:00 pm
- Contact:
-
Cece
- Family Elder
- Posts: 9335
- Joined: Mon Jan 04, 2010 3:00 pm
- Contact:
- Thekla
- Family Elder
- Posts: 149
- Joined: Sun Jul 04, 2010 2:00 pm
- Location: Germany
I never took any of the dmd's either. I do take LDN though. I've been on it for 6-7 years.
I was treated by Dr S just 2 weeks ago. My first treatment was in Germany a year ago. I have had improvements after both procedures---not nearly as much as I would like but absolutely worth it both times. This time there were no instant changes but by about the third day, my bladder was functioning better. It is not normal but distinctly better. Spasticity changed and seems to be improving. I can bend my left leg without help in bed. It used to just lock straight. It has only been 2 weeks, and there may be other gradual improvements happening too. After my first procedure, I had instant energy and an amazingly clear head. Instant changes are easy to notice. But I am very happy with any bladder improvement---that affects life so much. It is so odd to not need to think about bathrooms all of the time.
I was treated by Dr S just 2 weeks ago. My first treatment was in Germany a year ago. I have had improvements after both procedures---not nearly as much as I would like but absolutely worth it both times. This time there were no instant changes but by about the third day, my bladder was functioning better. It is not normal but distinctly better. Spasticity changed and seems to be improving. I can bend my left leg without help in bed. It used to just lock straight. It has only been 2 weeks, and there may be other gradual improvements happening too. After my first procedure, I had instant energy and an amazingly clear head. Instant changes are easy to notice. But I am very happy with any bladder improvement---that affects life so much. It is so odd to not need to think about bathrooms all of the time.
- Thekla
- Family Elder
- Posts: 149
- Joined: Sun Jul 04, 2010 2:00 pm
- Location: Germany
I just read of a patient who was treated for MT as part of a 2nd treatment. Afterward, there were still leg issues including swelling, pain and discoloration. A dopplar leg scan showed venous insufficiency in the saphenous vein and no DVT.
This seems is supposed to be an independent issue but could it be indicative of our susceptibility to malformed, irregular veins throughout the body? Perhaps diverse secondary areas of venous irregularities could explain some of the variation in symptoms in different patients.
This seems is supposed to be an independent issue but could it be indicative of our susceptibility to malformed, irregular veins throughout the body? Perhaps diverse secondary areas of venous irregularities could explain some of the variation in symptoms in different patients.
- pklittle
- Family Elder
- Posts: 341
- Joined: Sun Mar 07, 2010 3:00 pm
Cases are not being scheduled???drsclafani wrote:it is difficult to present cases if there are none scheduled.Cece wrote:
Maybe it is time for another case to be posted? It has been at least a few days. Or should we talk more about the balloon-CSA post?
I recall you telling us it takes hours to prepare these cases. Please please please do not feel pressured... we know you do need to sleep now and then...drsclafani wrote: it takes quite a bit of time to prepare these cases but look forward to some tonite or tmorrow

-
Cece
- Family Elder
- Posts: 9335
- Joined: Mon Jan 04, 2010 3:00 pm
- Contact:
- pklittle
- Family Elder
- Posts: 341
- Joined: Sun Mar 07, 2010 3:00 pm
Start rumors??? About what? I am just pointing out that he should not feel he needs to sacrifice his down time ( if he does) because there are expectations here.Cece wrote:careful or you will start rumors!
Dr. Sclafani is working. He treats every patient who is scheduled. Sometimes his dance card has open dockets. There is some wasted opportunity, that's all.
- Hooch
- Family Member
- Posts: 57
- Joined: Thu Feb 18, 2010 3:00 pm
I have thought for some time now, like Thekla, that we have other vein valve abnormalities throughout our bodies.
It was after I was treated for CCSVI that I asked for a venous doppler of my legs and sure enough there was reflux in the femoral (or is it the saphenous vein) in my painful leg.
This is of particular relevance here in Canada because as MSers the focus is on no treatment for CCSVI but we can have other parts of our body treated.
It was after I was treated for CCSVI that I asked for a venous doppler of my legs and sure enough there was reflux in the femoral (or is it the saphenous vein) in my painful leg.
This is of particular relevance here in Canada because as MSers the focus is on no treatment for CCSVI but we can have other parts of our body treated.
-
Cece
- Family Elder
- Posts: 9335
- Joined: Mon Jan 04, 2010 3:00 pm
- Contact:
I meant about whether or not cases were being scheduled. The first part of what you wrote, not the second. And I meant it pretty lightly. Previously he'd had people misinterpretating his 2010 shutdown woes for present-day woes, that sort of thing, so it's always good to be clear for anyone reading this that yes Dr. Sclafani is open for business. And that he tries to keep the business side separate from this educational thread. Whew.pklittle wrote:Start rumors??? About what? I am just pointing out that he should not feel he needs to sacrifice his down time ( if he does) because there are expectations here.Cece wrote:careful or you will start rumors!
Dr. Sclafani is working. He treats every patient who is scheduled. Sometimes his dance card has open dockets. There is some wasted opportunity, that's all.
For the second part, hmmmm, in some ways, it's like asking, so what did you do today, drsclafani? And his replies come in fantastic detail, with images and arrows pointing to relevant parts of the images. It would be ok if his replies came more simply, it's just fun to hear how things are going.
- NZer1
- Family Elder
- Posts: 1624
- Joined: Thu Feb 18, 2010 3:00 pm
- Location: Rotorua New Zealand
There has been allot of discussion on FB lately about the number of CCSVI patients who have had legs checked and found that there are problems. Please don't accept that MS has caused leg weakness and colour or temp issues. Ginger Mc Queen has just gone through the drama herself and found that there are problems in both legs. This has had allot of people saying that they too have found problems by ultrasound testing.
- NZer1
- Family Elder
- Posts: 1624
- Joined: Thu Feb 18, 2010 3:00 pm
- Location: Rotorua New Zealand
About a year ago I put some links here about the vertebral veins and also wanted to open up a discussion about the importance of vertebral veins. It appears that discussion has returned via Joan on FB. As a person with PPMS and with the knowledge that Dr. Zamboni was finding the high number of PPMS patients showed vertebral insufficiency I hope that the discussion can happen now that there is more acceptance of the opinion of Dr. Flanagan. From one of his old articles;
http://uprightdoctor.wordpress.com/2010 ... n-cooling/
"Both the cavernous and suboccipital cavernous sinuses also play a role in maintaining blood flow and pressure in the brain. Their inner walls contain pressure sensors called baroreceptors that detect pressure in the tunnels. When pressure goes up they send signals that cause the muscles in the incoming arteries to constrict and decrease blood flow. When pressure drops they signal the blood vessels to open up and increase blood flow. Technically it is called the “neurovascular myogenic autoregulatory reflex mechanism.” As an aside, similar important pressure receptors and blood flow regulators are located in the carotid sinuses near the Adams apple of the throat.
The cranial veins drain into two extracranial venous drainage routes. One route is the jugular veins. The other is the vertebral veins. Interestingly, in contrast to the jugular veins, the vertebral veins have no valves making them similar to the cranial veins. Thus, back pressure against the vertebral veins can affect both the drainage and cooling capacity of the brain. This is interesting in light of the fact that in addition to evidence of CCSVI, MS patients often experience symptoms of heat intolerance.
An increase in pressure in the suboccipital cavernous sinus can also decrease blood flow through the vertebral arteries that pass through it before supplying the inner rear and lower most parts of the brain. It can do so by either direct compression of the vertebral arteries, or by stimulating the pressure sensors in the sinus walls thereby causing the arteries to constrict.
Decreased blood flow through the vertebral arteries can cause a wide variety of symptoms such as fatigue, dizziness, loss of balance and coordination to name a few. The complete list of symptoms is too long to discuss here so I will save it for future posts."
My thoughts are along the lines of comparing flow volumes of normal's and PwMS and gain and understanding of what might be changing symptom expressions noted above. Ironic that these symptoms change with jugular angio treatment as well.
Could this be due the the way that the brain drainage is shared by many veins?
Regards all,
Nigel
http://uprightdoctor.wordpress.com/2010 ... n-cooling/
"Both the cavernous and suboccipital cavernous sinuses also play a role in maintaining blood flow and pressure in the brain. Their inner walls contain pressure sensors called baroreceptors that detect pressure in the tunnels. When pressure goes up they send signals that cause the muscles in the incoming arteries to constrict and decrease blood flow. When pressure drops they signal the blood vessels to open up and increase blood flow. Technically it is called the “neurovascular myogenic autoregulatory reflex mechanism.” As an aside, similar important pressure receptors and blood flow regulators are located in the carotid sinuses near the Adams apple of the throat.
The cranial veins drain into two extracranial venous drainage routes. One route is the jugular veins. The other is the vertebral veins. Interestingly, in contrast to the jugular veins, the vertebral veins have no valves making them similar to the cranial veins. Thus, back pressure against the vertebral veins can affect both the drainage and cooling capacity of the brain. This is interesting in light of the fact that in addition to evidence of CCSVI, MS patients often experience symptoms of heat intolerance.
An increase in pressure in the suboccipital cavernous sinus can also decrease blood flow through the vertebral arteries that pass through it before supplying the inner rear and lower most parts of the brain. It can do so by either direct compression of the vertebral arteries, or by stimulating the pressure sensors in the sinus walls thereby causing the arteries to constrict.
Decreased blood flow through the vertebral arteries can cause a wide variety of symptoms such as fatigue, dizziness, loss of balance and coordination to name a few. The complete list of symptoms is too long to discuss here so I will save it for future posts."
My thoughts are along the lines of comparing flow volumes of normal's and PwMS and gain and understanding of what might be changing symptom expressions noted above. Ironic that these symptoms change with jugular angio treatment as well.
Could this be due the the way that the brain drainage is shared by many veins?
Regards all,
Nigel
- CureOrBust
- Family Elder
- Posts: 3374
- Joined: Wed Jul 27, 2005 2:00 pm
- Location: Sydney, Australia
10 years ago I was diagnosed with superficial thrombosis of my left leg. The pain was unbearable, and you could see a vein popping out over my shin. Every now and then (<>6m) it would return and pass in the same day. A few years ago it started to come more often, so I had it checked using ultrasound (before dec 2008, and Zamboni's paper). They could find nothing wrong with my leg. Again it came up, and I had them scan it while it was hurting, and again nothing. Since I had my procedures, it hasn't been back. Only my Jugulars were ballooned.
- drsclafani
- Family Elder
- Posts: 3182
- Joined: Fri Mar 12, 2010 3:00 pm
- Location: Brooklyn, New York
- Contact:
Cece, I think that the more patients understand of the details, the more their physicians will look at the details.Cece wrote: hmmmm, in some ways, it's like asking, so what did you do today, drsclafani? And his replies come in fantastic detail, with images and arrows pointing to relevant parts of the images. It would be ok if his replies came more simply, it's just fun to hear how things are going.
There was a paper presented once that showed that when pictures of the face of the patient were included with the images of the CT scan, the reports were more detailed. My goal is to have patients put an educated face forward, with the hope that they will get a more committed response.
This weekend i treated four patients. One patient in particular was seen on both friday and saturday because of the complexity of the case. I think that this case will show so many interesting issues, some of which rarely are discussed.
The patient is a 52 year old female diagnosed with MS in 1998. She was originally diagnosed with RRMS but states that she never has classical relapses but rather mostly steadily progressive disease. She says that she has difficulty finding words sometimes but states that her memory is good. She has debilitating fatigue which exaccerabates symptoms such as difficulty swallowing, balance, tightness in her arm, coordination and spasticity.
She has had therapy with rebif, amantadine, LDN and in 2007 underwent an 18 month course of low dose cytoxan for MS administered through an implanted port.
As usual I accessed the venous circulation via the left saphenous vein. I attempted right jugular catheterization first. However after 30-40 minutes, I could not enter the right jugular vein. So i moved on to the left internal jugular vein..
Catheterization was also very difficult and I was about to give up whenI finally was able to enter the LIJV. Almost one hour had passed.
The catheter was placed in the left transverse sinus.
Dural sinus venography looked like this:
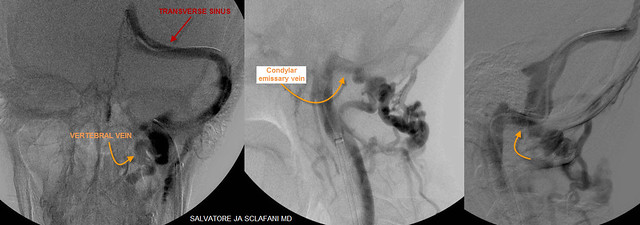
These images show that the transverse sinus and the sigmoid sinus had normal diameters. However there was a prominent connection between the transverse sinus inside the skull and the vertebral vein and posterior cervical branches on the outside. These vessels are connected by a very large emissary vein traversing across the skull via the hypoglossal canal. This canal is usually a very small opening in the skull but in this patient it is exceedingly large. I think this suggests that a long standing (perhaps congenital) outflow obstruction of the internal jugular vein has existed.
The catheter was then withdrawn into the internal jugular vein.
Venography looked like this:
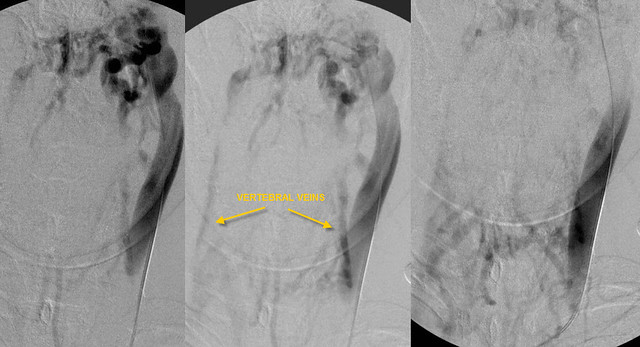
These images show very slow flow down the internal jugular vein. The majority of the flow is through collaterals involving the vertebral veins (yellow arrows). Other collaterals extend across the midline as well involving the face, spine and neck.
Note the failure of the contrast to exit the jugular vein.
The catheter was positioned lower in the internal jugular vein and the venogram was repeated. Then intravascular ultrasound was performed. Note the location of the probe in the upper right image.
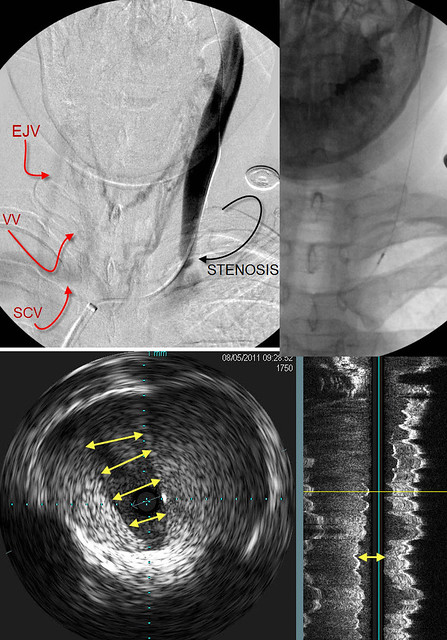
The upper left image shows the area of stenosis (black curved arrow). Minimal contrast exits the IJV; Collaterals are seen crossing the midline to opacify the External jugular vein (EJV), the vertebral vein (VV) and the subclavian vein (SCV). Other collaterals are seen in the midline.
The Left bottom image is an IVUS image at the level of the probe. The valve was persistently closed. The dense white tissue represents the valve tissue, thickened and immobile.
The image on the bottom right is another view. It shows a narrowed valve (double arrow). Dense tissue is evident on both sides of the arrow.
I rely upon IVUS to plan treatment of these stenoses.
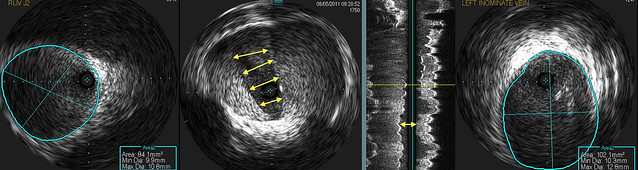
I rely upon IVUS to plan my treatment. I use it to decide what size balloon to use and where to position the balloon. These three images show the valvular stenosis and an image above (LEFT) and below (RIGHT) the valve.
I think that the valve is quite thick manifested by the brightness of the echoes on the valve. I think that a somewhat larger balloon may be necessary. So on the LEFT the vein measures 84 mm2 in cross sectional area. This is equivalent to a 10 mm balloon. Below the valve (RIGHT), the vein measured 102 mm2. That is close to a 12 mm balloon (113 square mm). That means the the minimum balloon I would use would be a 14 mm balloon which has a cross sectional area of 154 mm2.
That is a really big balloon to inflate on that upper jugular vein especially on the left side where there is a angle between the orientation of the vein and the orientation of the balloon.
So IVUS tells me that i need to position as much of the balloon BELOW the valvular stenosis.
In this case, the valvular tissue is thick and will require a strong angioplasty. I have included images above and below the area of valvular stenosis because they are important in deciding what size balloon to use and how to position it.
The image on the LEFT is above the injury. The cross sectional area is 84mm2. This is slightly larger than a 10 mm balloon. The image on the RIGHT shows the vein BELOW the valve.The cross sectional area measured 102 mm2, slightly less than a 12 mm balloon. So we surely will have to start with a 14mm balloon which has a cross sectional radea of 154 mm2. That is more than twice the cross sectional area of the vein above the stenosis. On the left jugular, because of the angle of the vein compared to the balloon, this is a bit riskier for dissection.
It because critical that I position this balloon so that the majority of the balloon is below the stenosis where the vein is of a dimension that can more easily accomodate the 14 mm (and possibly a 16mm) balloon.
This next sequence shows that decision in action.
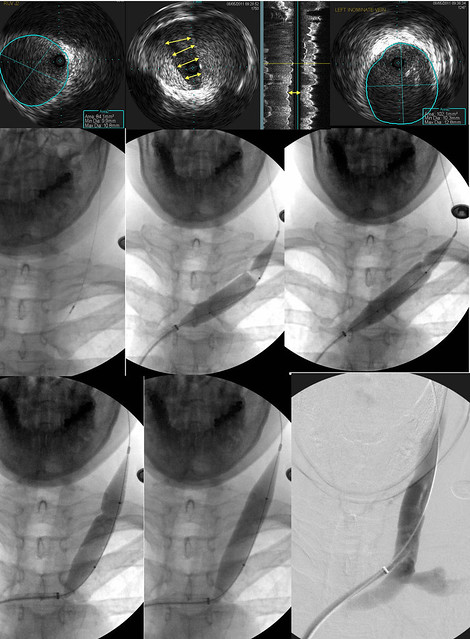
The uper row again shows the IVUS exam. The middle row (Left) shows the IVUS probe at the level of the valve stenosis. It is just below the second rib. I attempted to place the upper shoulder of the 14 mm balloon (note the black dot at the waist on the balloon) exactly at the valvular stenosis (MIDDLE). Unfortunately I cut it too close and the balloon slipped below the stenosis. (RIGHT) The balloon was deflated and repositioned.
The lower row shows the new position of the balloon. Thus there is a small amount of upper vein that will be subjected to a fairly large distension (double in cross sectional area). The waist on the balloon (indicative of resistance to dilation) was overcome with 18 atmospheres of pressure. The post dilatation venogram shows a really nice diameter.
Unfortunately, there was still slow flow....
But that is a story for another day
Any questions so far?
Last edited by drsclafani on Sun Aug 14, 2011 7:45 pm, edited 3 times in total.
-
Cece
- Family Elder
- Posts: 9335
- Joined: Mon Jan 04, 2010 3:00 pm
- Contact:
Yes, that's a worthwhile goal.Cece, I think that the more patients understand of the details, the more their physicians will look at the details.
There was a paper presented once that showed that when pictures of the face of the patient were included with the images of the CT scan, the reports were more detailed. My goal is to have patients put an educated face forward, with the hope that they will get a more committed response.
Here's a nyt write-up on the paper mentioned:
www.nytimes.com/2009/04/07/health/07pati.html
But what does the picture of the radiologist (included in the article) say about him?

