numbness23, no recriminations. It is difficult for both patient and doctor to do this work without support. Patients undergo treatment clandestinely, not sharing the information with their neurologists, if they have one, who shame them. Treating physicians without the necessary tools of assessment, must go it alone, misunderstood by their colleague. We try very hard; we need to hang together to give this a chance.numbness23 wrote:I am not in agreement in any way shape or form with the FDA but drs doing angios and not collecting data for follow up is irresponsible and is a big part of the turf war as best ad speaks. Patient reported results is a joke and is not furthering our fight. Without actual substantiated procedural follow up by trained professionals, nobody is going to help us. Even if there is definable proof there will still be doubters. But here we are years into this thing and our best trials for ccsvi are patient emails. I have watched this site for the last two years and see people posting like mad , get their crack at the liberation, and then disappear. No doubt procedures are refined thanks to Sal, but we need some meat if the medical world is gonna take us seriously. Especially britspores
DrSclafani answers some questions
- drsclafani
- Family Elder
- Posts: 3182
- Joined: Fri Mar 12, 2010 3:00 pm
- Location: Brooklyn, New York
- Contact:
Re: DrSclafani answers some questions
Salvatore JA Sclafani MD
Patient contact: ccsviliberation@gmail.com
Patient contact: ccsviliberation@gmail.com
- drsclafani
- Family Elder
- Posts: 3182
- Joined: Fri Mar 12, 2010 3:00 pm
- Location: Brooklyn, New York
- Contact:
Re: DrSclafani answers some questions
I once asked Dr Zamboni if i could review some of his patient studies. He said that it was not possible. It would require permission of his IRB and it would also be a violation of his trustwith his patients.mo_en wrote:Dear Dr S, one more question regarding
No Evidence of Chronic Cerebrospinal Venous Insufficiency at Multiple Sclerosis Onset by
Claudio Baracchini, Paola Perini, Massimiliano Calabrese, Francesco Causin, Francesca Rinaldi, Paolo Gallo
Venography was performed to 7 people with probable MS that were positive in at least 2 ultrasound criteria, and to 3 more that we not. No problem was found, except for one hypoplastic RIJV.
My question is:
Is it feasible to find these 10 people, perform venography your way and compare the results? It would make a very good study and a (low cost) hard evidence against ccsvi-doubters.
Ten patients would make a nice study, but, ironically, our colleagues would not accept it as sufficient evidence.
But the study that you mention was done a long time ago. More than disproving the existence of CCSVI, it proved that considerable experience is necessary to recognize many of the findings of an abnormal venogram. Indeed, when we first started looking at these stenoses, it was thought that the vein wall was stenotic. It took considerable time and the help of the IVUS to show that the stenosis is most commonly caused by an immobile valve rather than stenosis of the wall of the vein.
Based upon a recent case in a young man, it is my sense that composition and function of the valvular tissue evolves with time.I think that i will share that case with you.
Salvatore JA Sclafani MD
Patient contact: ccsviliberation@gmail.com
Patient contact: ccsviliberation@gmail.com
- drsclafani
- Family Elder
- Posts: 3182
- Joined: Fri Mar 12, 2010 3:00 pm
- Location: Brooklyn, New York
- Contact:
Re: DrSclafani answers some questions
drsclafani wrote: But the study that you mention was done a long time ago. More than disproving the existence of CCSVI, it proved that considerable experience is necessary to recognize many of the findings of an abnormal venogram. Indeed, when we first started looking at these stenoses, it was thought that the vein wall was stenotic. It took considerable time and the help of the IVUS to show that the stenosis is most commonly caused by an immobile valve rather than stenosis of the wall of the vein.
Based upon a recent case in a young man, it is my sense that composition and function of the valvular tissue evolves with time.I think that i will share that case with you.
Its nature is such that it is common for abnormalities to be subtle and often unrecognizable by venography in young people with MS. With the progression in time the character of the valvular tissue is altered, becoming thicker with age. With aging the vein above the obstruction distends and makes the stenosis more obvious. As the valve thickens, it may become more noticeable. With the vein obstructed, the collateral veins enlarge and the orifice dilates to accomodate the flow. I believe there are obstructions that cannot be identified by the venogram at a young age. Even with IVUS the valvular stenosis and immoblity may be subtle and at some oint be imperceptible.
The case in point illustrates this point. I plan to go back and review the IVUS exams of the youngest patients and compare them to those who have had the disease for a considerable time.
This is a 20 year old Greek man who has had symptoms of multiple sclerosis since age 15. His major problems are difficulty in walking, predominantly because of spasticity caused by upper motor neuron disease. He has weakness in the right foot, with a foot drop, light numbness in the right finger , imbalance, temperature intolerance and fatigue. He had several exacerbations while taking avonex, but becamse exacerbation free while taking natalizumab (tysabri). When tysabri was stopped and copaxone was given he had several exacerbations. While currently taking natalizumab, he has had no exacerbations. He had two doppler exams, i(n Athens by Dr Liasis and in my office in Brooklyn) which showed signs consistent with CCSVI. His neurological examination showed slight nystagmus, absent vibratory sense in both lower legs and feet, an intention tremor and severe spastic weakness in both lower extremities. Rhomberg's test was positive Babinski was positive bilaterally. Clonus of both ankles was present.
Venography of the right internal jugular vein seemed pretty normal. However there was a subtle finding of possible jet effect (orange arrow).
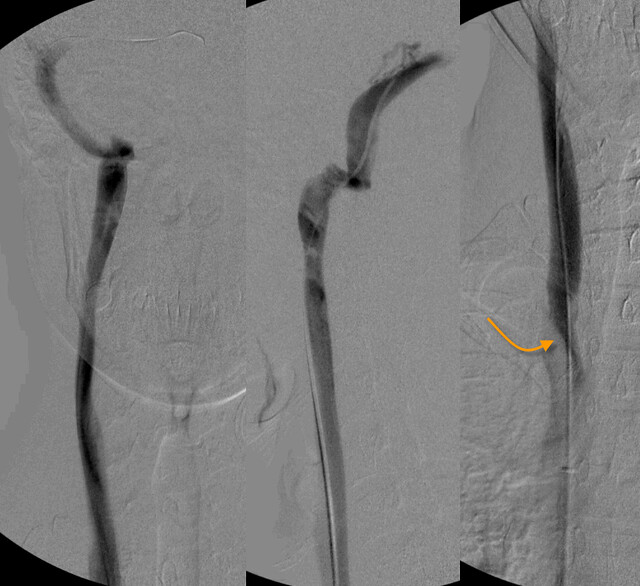
However the IVUS was quite obvious
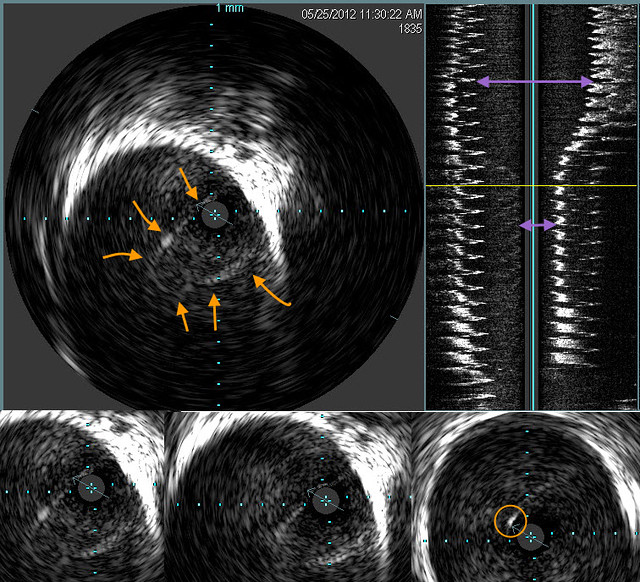
The orange arrows outline an immobile valve that funnels down to a high degree of obstruction.The purple double arrows show how great was the stenosis. However the echogenic area of the vein is not pronounces and the valve was barely visible on IVUS. I have circled in the righ right lower image a thickened focus of echogenic material in the valve .
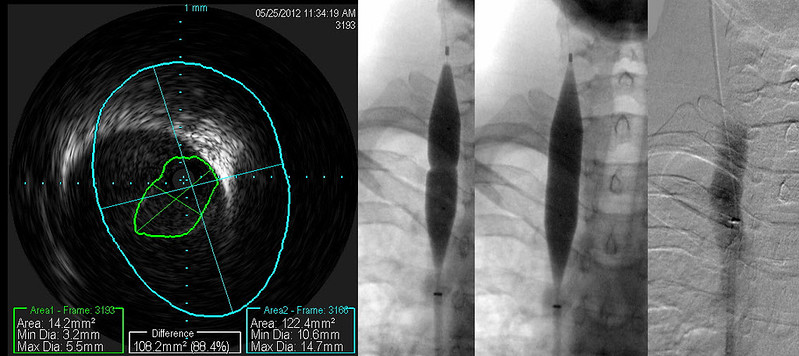
You can see the effective expansion of the vein on this patient's post angioplasty image. A small area of buckled valvular tissue is still within the lumen. Nowever an annular valvular stenosis is no longer present.
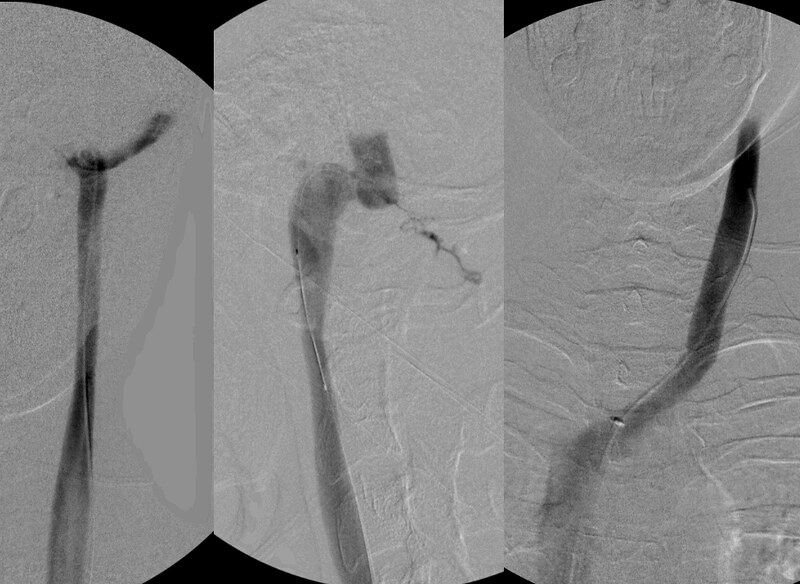
The findings were more subtle on the left side. I can discern no clues (except some possible puddling of contrast media within the cusp of a normal appearing venogram). The small amount of opacification of a condylar emissary vein is within normal appearance. It is interesting that the patient has not posterior skull base head and neck ache. I strongly suspect that this headache is due to distension of the posterior cervical veins.
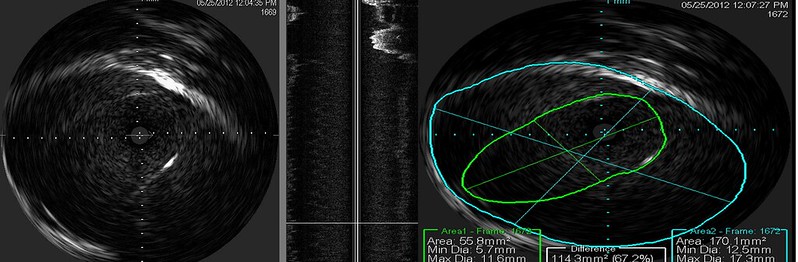
The degree of echogenicity of the valve is not great but sufficient to make it perceptible. I will find a case of long standing CCSVI in a patient with more than 20 years of MS. The difference is striking.
IVUS shows valve pretty clearly. Despite watching this valve orifice for more than one minute, it never opened. Suprisingly, the stenosis measured 67% and nothing was apparent on the venogram.
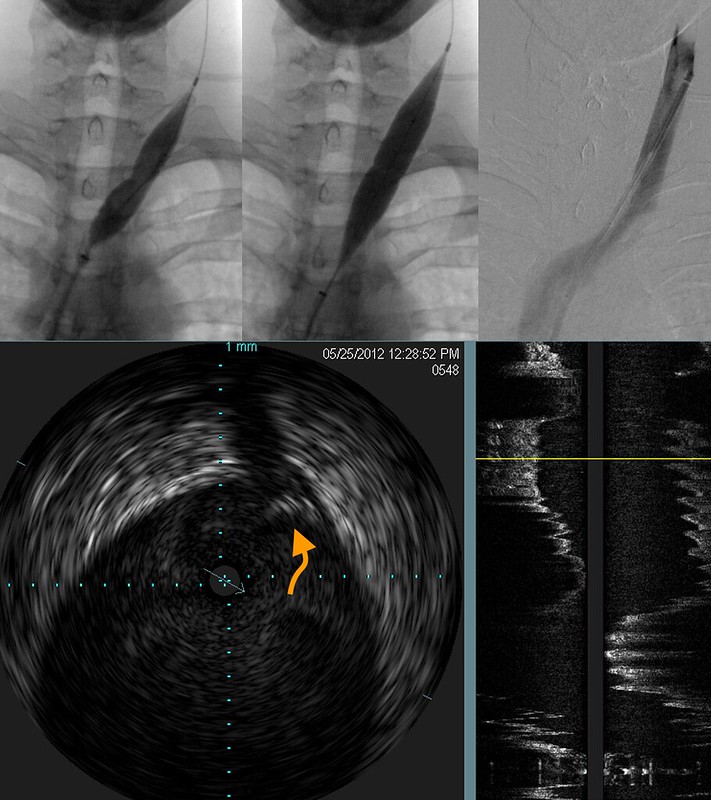
Venoplasty was performed. I think that the balloon sizing was very good. Although IVUS after venoplasty shows some residual valve tissue in the lumen (arrow), The narrowing ring of tissue has been disrupted and we have not risked injury to the vein. A larger balloon might have given a better picture, but I am not a photographer.
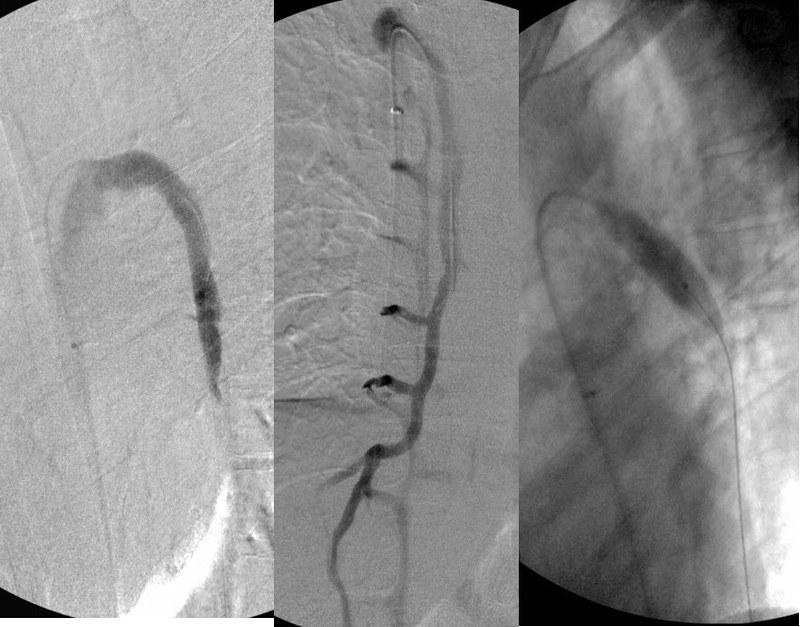
The azygous venogram looks pretty good too, although I would prefer to not see so much reflux. I am concerned by reflux but reflux alone does not tell me where to dilate. I would prefer not to do indiscriminate venooplasty.
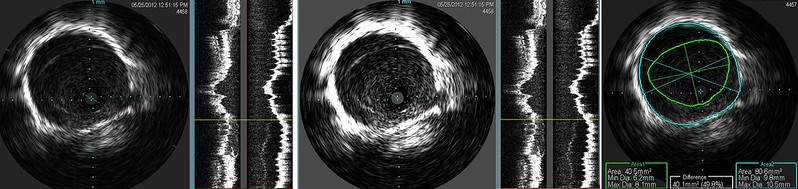
Again IVUS is not equivocal in this case. I showed the same image in two different brightness/contrast levels to illustrate how subtle it can be. Image too dark and it can very difficult to see the immobile valve. Looking at this abnormality, i was not impressed by the degree of stenosis on visual terms. But the IVUS calculation show this to be just about a 50% stenosis. More than the eye can tell.
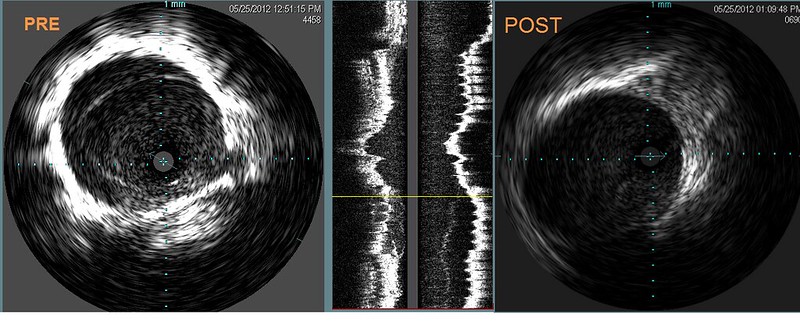
The post venoplasty image shows that no obstruction is present.
Such a case illustrates how even the accepted Gold Standard may miss stenoses in apparently normal looking venograms. Venography is less than perfect because the disease is not generally of the vein itself. But rather of the valve which is much better visualized by IVUS.
I am going to evaluate my speculation that the IVUS appearance changes with duration of disease or with age.
DrS
Salvatore JA Sclafani MD
Patient contact: ccsviliberation@gmail.com
Patient contact: ccsviliberation@gmail.com
-
Cece
- Family Elder
- Posts: 9335
- Joined: Mon Jan 04, 2010 3:00 pm
- Contact:
Re: DrSclafani answers some questions
As we age, the valve tissue becomes thicker.Its nature is such that it is common for abnormalities to be subtle and often unrecognizable by venography in young people with MS. With the progression in time the character of the valvular tissue is altered, becoming thicker with age. With aging the vein above the obstruction distends and makes the stenosis more obvious. As the valve thickens, it may become more noticeable. With the vein obstructed, the collateral veins enlarge and the orifice dilates to accomodate the flow. I believe there are obstructions that cannot be identified by the venogram at a young age. Even with IVUS the valvular stenosis and immoblity may be subtle and at some oint be imperceptible.
Also as we age, the vein above the stenosis distends.
Collateral veins enlarge and the orifice dilates to accomodate flow - this would be the top of the vein that dilates? J3.
This fits with what we saw in the Beirut study, that found CCSVI in 12 out of 13 patients with "advanced RR MS" of greater than ten years, but not in patients with CIS or less than 5 years of MS. With this theory, it's not the CCSVI wasn't there in the younger patients, but the body had not yet reacted with collaterals and dilatation and thickening of the valve and aging, and so it was not picked up.
The Beirut study was interpreted as indicating that CCSVI was not a likely cause of MS, since CCSVI was not found to be present in patients earlier in their disease course. That conclusion can be tossed if indeed the venous malformations are there but more challenging to image. (the beirut study = http://www.ncbi.nlm.nih.gov/pubmed/21041329 )
-
Cece
- Family Elder
- Posts: 9335
- Joined: Mon Jan 04, 2010 3:00 pm
- Contact:
Re: DrSclafani answers some questions
So residual valve tissue is a real thing that can be imaged...drsclafani wrote:
Venoplasty was performed. I think that the balloon sizing was very good. Although IVUS after venoplasty shows some residual valve tissue in the lumen (arrow), The narrowing ring of tissue has been disrupted and we have not risked injury to the vein. A larger balloon might have given a better picture, but I am not a photographer.
-
Cece
- Family Elder
- Posts: 9335
- Joined: Mon Jan 04, 2010 3:00 pm
- Contact:
Re: DrSclafani answers some questions
So in this image there is a lack of dilatation just above the stenosis, that would normally be present in patients with older veins and/or longer disease duration. There is also a lack of dilatation in the upper portion of the jugular, and that is because the patient has not developed collaterals that would allow flow to swell that section of the vein before diverging off into the collaterals. But why wouldn't a young patient have developed collaterals? If CCSVI is congenitally present since birth, then a twenty-year-old patient would have had twenty years to develop collaterals. The body can develop collaterals very quickly.drsclafani wrote:Venography of the right internal jugular vein seemed pretty normal. However there was a subtle finding of possible jet effect (orange arrow).
The image on the left looks to me like a normal healthy venogram of the vein. On the right, it does look like a funnel effect from a stenosis, but you must have had to capture that at just the right moment.
-
Cece
- Family Elder
- Posts: 9335
- Joined: Mon Jan 04, 2010 3:00 pm
- Contact:
Re: DrSclafani answers some questions
Good catch.However the IVUS was quite obvious
The orange arrows outline an immobile valve that funnels down to a high degree of obstruction.The purple double arrows show how great was the stenosis. However the echogenic area of the vein is not pronounces and the valve was barely visible on IVUS. I have circled in the righ right lower image a thickened focus of echogenic material in the valve .
The thickened focus of echogenic material in the valve reminds me of the dots of echogenic material from webs. Could webs also thicken as we age? Were any of those webs dots in the area of the valves, and could any of them have been a misidentified hard-to-visualize fixed-but-not-yet-thickened valve? Or were they commonly found elsewhere in the vein?
Someone should really get you a superIVUS. :sigh: You had theorized that superIVUS might pick up these more-difficult-to-see abnormalities in patients with CIS or early MS. This case makes a superIVUS even more attractive, to push that boundary of what can be seen.
Last edited by Cece on Tue May 29, 2012 8:02 pm, edited 1 time in total.
-
Cece
- Family Elder
- Posts: 9335
- Joined: Mon Jan 04, 2010 3:00 pm
- Contact:
Re: DrSclafani answers some questions
I am well acquainted with that skull base headache. But less well acquainted with the posterior cervical veins.The findings were more subtle on the left side. I can discern no clues (except some possible puddling of contrast media within the cusp of a normal appearing venogram). The small amount of opacification of a condylar emissary vein is within normal appearance. It is interesting that the patient has not posterior skull base head and neck ache. I strongly suspect that this headache is due to distension of the posterior cervical veins.
Wikipedia http://en.wikipedia.org/wiki/Deep_cervical_vein wrote:The deep cervical vein (posterior vertebral or posterior deep cervical vein) accompanies its artery between the Semispinales capitis and colli.
It begins in the suboccipital region by communicating branches from the occipital vein and by small veins from the deep muscles at the back of the neck.
It receives tributaries from the plexuses around the spinous processes of the cervical vertebræ, and terminates in the lower part of the vertebral vein.
-
jillMEnz
- Getting to Know You...
- Posts: 12
- Joined: Mon Apr 30, 2012 11:56 pm
Re: DrSclafani answers some questions
Hi Dr Sal,
Are you also noting down whether patients with such extraordinary valves have other weird anatomy? eg Marfans or Ehlers Danlos. My partner i'v just realised has Marfans limbs and a shocking 'heart attack /triple A' history on his fathers side of the family.
Have you treated ED or M patients? Do their veins 'hold' the ballooning or are they prone to restenose?
Just thoughts
Are you also noting down whether patients with such extraordinary valves have other weird anatomy? eg Marfans or Ehlers Danlos. My partner i'v just realised has Marfans limbs and a shocking 'heart attack /triple A' history on his fathers side of the family.
Have you treated ED or M patients? Do their veins 'hold' the ballooning or are they prone to restenose?
Just thoughts
- NZer1
- Family Elder
- Posts: 1624
- Joined: Thu Feb 18, 2010 3:00 pm
- Location: Rotorua New Zealand
Re: DrSclafani answers some questions
Hearing the age theory etc reminds me of why there is such a push for lifestyle and diet therapy by people like George Jelinek who is asking for people to help in his online study:
Calling people with multiple sclerosis (MS) to take part in a large international research study on.
http://www.overcomingmultiplesclerosis.org
http://www.surveymonkey.com/s/HOLISM
I understand the logic in this where the age, diet, exercise and mindfullness 'could delay the effects of CCSVI'. (If people like George and Terry Wahls had been checked with IVUS before the diet etc approach it would have been an interesting study!
I think that the 'super IVUS' if there is such a thing will sway the knowledge curve towards the real issue.
*Is there such a thing 'yet'?
*What comes first and also is that first issue the most important factor in the big picture with defining CCSVI?
If the valves are defective, if there are other malformations eg webs, membranes, septums then the answer to what is cause of brain damage in many diseases is becoming clearer.
The time factor with physical aging added is giving a more substantial ill effect.
So the split in thinking where the CCSVI symptom group is now being separated from MS symptoms will find an interesting reconnection to MS as research follows this theory?
Calling people with multiple sclerosis (MS) to take part in a large international research study on.
http://www.overcomingmultiplesclerosis.org
http://www.surveymonkey.com/s/HOLISM
I understand the logic in this where the age, diet, exercise and mindfullness 'could delay the effects of CCSVI'. (If people like George and Terry Wahls had been checked with IVUS before the diet etc approach it would have been an interesting study!
I think that the 'super IVUS' if there is such a thing will sway the knowledge curve towards the real issue.
*Is there such a thing 'yet'?
*What comes first and also is that first issue the most important factor in the big picture with defining CCSVI?
If the valves are defective, if there are other malformations eg webs, membranes, septums then the answer to what is cause of brain damage in many diseases is becoming clearer.
The time factor with physical aging added is giving a more substantial ill effect.
So the split in thinking where the CCSVI symptom group is now being separated from MS symptoms will find an interesting reconnection to MS as research follows this theory?
- drsclafani
- Family Elder
- Posts: 3182
- Joined: Fri Mar 12, 2010 3:00 pm
- Location: Brooklyn, New York
- Contact:
Re: DrSclafani answers some questions
sorry about your partner. I havent treated patients with Marfan's, indeed havent seen that characteristic appearance in any of my patients. I have diagnosed several patients with EDS during my initial clinical assessment and referred them on for further genetic testing, couseling etc. I have treated two patients, one with diagnosed and one with probable EDS. I didnt notice anything unusual about either's response to treatments.jillMEnz wrote:Hi Dr Sal,
Are you also noting down whether patients with such extraordinary valves have other weird anatomy? eg Marfans or Ehlers Danlos. My partner i'v just realised has Marfans limbs and a shocking 'heart attack /triple A' history on his fathers side of the family.
Have you treated ED or M patients? Do their veins 'hold' the ballooning or are they prone to restenose?
Just thoughts
DrS
Salvatore JA Sclafani MD
Patient contact: ccsviliberation@gmail.com
Patient contact: ccsviliberation@gmail.com
- drsclafani
- Family Elder
- Posts: 3182
- Joined: Fri Mar 12, 2010 3:00 pm
- Location: Brooklyn, New York
- Contact:
Re: DrSclafani answers some questions
The device is built and awaiting approvals and production. It is said to have five times the resolution that the current device has.NZer1 wrote:Hearing the age theory etc reminds me of why there is such a push for lifestyle and diet therapy by people like George Jelinek who is asking for people to help in his online study:
I think that the 'super IVUS' if there is such a thing will sway the knowledge curve towards the real issue.
*Is there such a thing 'yet'?
Nigel, you wont get me involved with that debate. it is pure conjecture and hypothesis. I continue to maintain that i treat ccsvi and that some symptoms get better after treatment. Whether treating CCSVI alters long term outcome of MS will require a lot more time to parse out.*What comes first and also is that first issue the most important factor in the big picture with defining CCSVI?
This too is speculation. I want to clarify that this is an impression of mine. I am trying to design a retrospective comparison of IVUS imaging in a large cohort to evaluate that spseculation.If the valves are defective, if there are other malformations eg webs, membranes, septums then the answer to what is cause of brain damage in many diseases is becoming clearer.
The time factor with physical aging added is giving a more substantial ill effect.
The challenging part is that there is going to be an overlap of symptoms caused by ccsvi and the symptoms caused by MS. I thinkm that is why it is so difficult to predict response.So the split in thinking where the CCSVI symptom group is now being separated from MS symptoms will find an interesting reconnection to MS as research follows this theory?
Salvatore JA Sclafani MD
Patient contact: ccsviliberation@gmail.com
Patient contact: ccsviliberation@gmail.com
- drsclafani
- Family Elder
- Posts: 3182
- Joined: Fri Mar 12, 2010 3:00 pm
- Location: Brooklyn, New York
- Contact:
Re: DrSclafani answers some questions
Collaterals do develop quickly but whether they are visible depends upon the methodology of the contrast injection. I am focusing more on low volume injections with low pressure which will show reflux with less frequency.Cece wrote:So in this image there is a lack of dilatation just above the stenosis, that would normally be present in patients with older veins and/or longer disease duration. There is also a lack of dilatation in the upper portion of the jugular, and that is because the patient has not developed collaterals that would allow flow to swell that section of the vein before diverging off into the collaterals. But why wouldn't a young patient have developed collaterals? If CCSVI is congenitally present since birth, then a twenty-year-old patient would have had twenty years to develop collaterals. The body can develop collaterals very quickly.drsclafani wrote:Venography of the right internal jugular vein seemed pretty normal. However there was a subtle finding of possible jet effect (orange arrow).
Looking with IVUS i do notice large tributaries, i am just not forcing the contrast into them
cool, eh? people see whar they are prepared to seeThe image on the left looks to me like a normal healthy venogram of the vein. On the right, it does look like a funnel effect from a stenosis, but you must have had to capture that at just the right moment.
Salvatore JA Sclafani MD
Patient contact: ccsviliberation@gmail.com
Patient contact: ccsviliberation@gmail.com
- mo_en
- Family Member
- Posts: 48
- Joined: Thu Dec 09, 2010 3:00 pm
- Location: Patras, Greece
Re: DrSclafani answers some questions
Great presentation Dr S!
Dr. Brenda Banwell is doing an ultrasound study on children with MS. If early CCSVI is difficult to trace by venography, i suspect it will be even harder to do with ultrasound. Do you agree?
To the questions:
1.
2. Does blood flow speed influence the way a vein is opacified by contrast media? Is it possible that venograms of problematic veins look normal because blood speed is low and contrast particles have time to surround the valves? Have you noticed (measured?) differences in blood speed between patients and healthy controls?
Dr. Brenda Banwell is doing an ultrasound study on children with MS. If early CCSVI is difficult to trace by venography, i suspect it will be even harder to do with ultrasound. Do you agree?
To the questions:
1.
Do you think that Tysabri may act by reducing CCSVI severity? It's supposed to prevent T cells from adhering to the vein walls. Could this action be anticoagulant and allow a swift blood flow through the immobile valves?drsclafani wrote:but becamse exacerbation free while taking natalizumab (tysabri).
2. Does blood flow speed influence the way a vein is opacified by contrast media? Is it possible that venograms of problematic veins look normal because blood speed is low and contrast particles have time to surround the valves? Have you noticed (measured?) differences in blood speed between patients and healthy controls?
-
AnCap
- Getting to Know You...
- Posts: 13
- Joined: Thu Mar 22, 2012 1:36 pm
Re: DrSclafani answers some questions
Dr. Sclafani,
I'm 25 with suspected, undiagnosed primary progressive MS for 3 years but there were signs and symptoms before then. My disease is aggressive, already causing atrophy of my forearms (being a computer programmer, I will have to go on long-term disability soon because of the difficulty typing), and bilateral weaksness and spasticity of all four limbs. I won't be walking for much longer and the use of my arms is rapidly fading. How much success have you had treating PPMS patients?
I believe Dr. Schelling is correct in postulating that venous reflux into the lumbo-sacral region that displaces CSF cranially from the lumbar cistern is one of the forces that causes fibrosis of the flanks of the spinal cord (he has reviewed my MRIs and while there are no lesions, typical of PPMS, he noted faint indications of involvement of the flanks of the cord). Virtually all of my symptoms are motor related, typical of PPMS. The reason I believe he is correct is that I have observed a very recurring pattern of flashing lights and exacerbation of my symptoms whenever my GI tract issues (which have exited since age 13 after head trauama, my disease is multi-factoral for sure, explaining why it surfaced so early) flare up, frequently after eating a meal and usually in the mornings. Morning diarrhea has been a part of life since about age 16 and my symptoms worsen after defecation. In fact, I am almost certain that the physical action of leaning forward (after being seated for a relatively extended period of time) can cause the flashing lights and worsening of my symptoms. In addition, my abdomen pulses very strongly, which can fluctuate but the pulsing is most severe during times when I know I'm progressing.
PPMS is a slightly different animal and I have been studying MS for three years and I am sure that there are more forces involved in producing these CSF shifts. I am actively pursuing those but I am interested in being treated for CCSVI again. I was treated by Dr. Sullivan in October 2010, very early on and one of his first patients. There was narrowing at both IJV valves and superior to the valves, and a stenosis in the arch of the azygos and another 4cm stenosis 10cm below the arch. There was extensive reflux into the branch vessels of the azygos, per the report. A lot has changed since then. My ascending lumbar vein, renal veins, and sacral veins have not been inspected which is what I'm most concerned about.
Thanks for all the time you spend on these boards, doctor.
-Peter
I'm 25 with suspected, undiagnosed primary progressive MS for 3 years but there were signs and symptoms before then. My disease is aggressive, already causing atrophy of my forearms (being a computer programmer, I will have to go on long-term disability soon because of the difficulty typing), and bilateral weaksness and spasticity of all four limbs. I won't be walking for much longer and the use of my arms is rapidly fading. How much success have you had treating PPMS patients?
I believe Dr. Schelling is correct in postulating that venous reflux into the lumbo-sacral region that displaces CSF cranially from the lumbar cistern is one of the forces that causes fibrosis of the flanks of the spinal cord (he has reviewed my MRIs and while there are no lesions, typical of PPMS, he noted faint indications of involvement of the flanks of the cord). Virtually all of my symptoms are motor related, typical of PPMS. The reason I believe he is correct is that I have observed a very recurring pattern of flashing lights and exacerbation of my symptoms whenever my GI tract issues (which have exited since age 13 after head trauama, my disease is multi-factoral for sure, explaining why it surfaced so early) flare up, frequently after eating a meal and usually in the mornings. Morning diarrhea has been a part of life since about age 16 and my symptoms worsen after defecation. In fact, I am almost certain that the physical action of leaning forward (after being seated for a relatively extended period of time) can cause the flashing lights and worsening of my symptoms. In addition, my abdomen pulses very strongly, which can fluctuate but the pulsing is most severe during times when I know I'm progressing.
PPMS is a slightly different animal and I have been studying MS for three years and I am sure that there are more forces involved in producing these CSF shifts. I am actively pursuing those but I am interested in being treated for CCSVI again. I was treated by Dr. Sullivan in October 2010, very early on and one of his first patients. There was narrowing at both IJV valves and superior to the valves, and a stenosis in the arch of the azygos and another 4cm stenosis 10cm below the arch. There was extensive reflux into the branch vessels of the azygos, per the report. A lot has changed since then. My ascending lumbar vein, renal veins, and sacral veins have not been inspected which is what I'm most concerned about.
Thanks for all the time you spend on these boards, doctor.
-Peter
