Notes from CureIous' at Stanford
- Sharon
- Family Elder
- Posts: 1286
- Joined: Sun Nov 07, 2004 3:00 pm
- Location: Colorado
- Contact:
Hey, Mark!
What an interesting follow-up report. You are so thorough at telling the little bits and pieces -- all of it is fascinating.
The BCV issues is fascinating to me because one of my stents is in that area. It was not until Dake placed the 2nd stent at the BCV did blood flow through the upper stent.
When do you think you will get the MRI results? I am so glad to hear that Dake is going back to count and size those little spots. My daughter is hoping to be the first ever non-diagnosed MS patient with a stent who no longer has lesions. My one year follow-up should be the first week in June, but I am holding off to go with my daughter in July or August.
Loved the T-shirt! Picture perfect of a proud father.
Sharon
What an interesting follow-up report. You are so thorough at telling the little bits and pieces -- all of it is fascinating.
The BCV issues is fascinating to me because one of my stents is in that area. It was not until Dake placed the 2nd stent at the BCV did blood flow through the upper stent.
When do you think you will get the MRI results? I am so glad to hear that Dake is going back to count and size those little spots. My daughter is hoping to be the first ever non-diagnosed MS patient with a stent who no longer has lesions. My one year follow-up should be the first week in June, but I am holding off to go with my daughter in July or August.
Loved the T-shirt! Picture perfect of a proud father.
Sharon
- Johnson
- Family Elder
- Posts: 979
- Joined: Tue Dec 01, 2009 3:00 pm
- Location: Ucluluet, BC
- Contact:
I have to concur with the rave reviews on your report.
Just one question - you wrote: "So there's a thin area, with a slight pressure gradient, and when he fixed the down-below part, the upper part improved, and he thought that the upper portion expanded just a wee bit. " Do you mean the vein wall is thin, or the diameter of the vein is narrowed?
Just a pondering: I wonder if the collaterals have always been there - in everyone, CCSVI or not, and are simply not usually observed. Think of the huge increase in blood flow when the heart rate gets up in exercise, and the brain needs to cool.
Just one question - you wrote: "So there's a thin area, with a slight pressure gradient, and when he fixed the down-below part, the upper part improved, and he thought that the upper portion expanded just a wee bit. " Do you mean the vein wall is thin, or the diameter of the vein is narrowed?
Just a pondering: I wonder if the collaterals have always been there - in everyone, CCSVI or not, and are simply not usually observed. Think of the huge increase in blood flow when the heart rate gets up in exercise, and the brain needs to cool.
My name is not really Johnson. MSed up since 1993
- CureIous
- Family Elder
- Posts: 1266
- Joined: Tue Jul 14, 2009 2:00 pm
- Location: Riverside, CA
- Contact:
Will come back later with a couple explanatory shots of what was attended to in the follow up procedure.
This is an assemblage of scans from 2008, 2009 (pre-op), 2009 (2 month follow up), and the latest scan April 2010.
Want to point out a few things though for posterity:
1. Different machines, different operators, different levels of contrast=different scans. Even the 3 at Stanford are all different, though the protocols are similiar, there were 3 different operators. (Aug-Oct-Apr).
2. The slightest variation in patient position in the tube, head slightly forward/back/tilted etc. will yield differing views of the same area, so no two scans are going to be alike. The scan goes the same way every time, the patient does not. So on some of the comparisons there's just no comparable slice. That means no comparable results.
3. MRI's are hereby stipulated as to not proving ANYTHING pro, or con in the CCSVI paradigm, they are just another piece of the puzzle. Obviously we all know that lesion load vs. disability is a non-starter, so lack of lesion load conversely doesn't "prove" anything, but it's nice to see nothing new.
The April scan lesions appear to me to be slightly less contrasted/lit up, but once again that could be an operator variation... The pics seem to be a bit darker overall.
4. Speaking specifically of my own, there were a few areas that exacerbated between the first scan in 2008 and 2009, and definitely a lot more than my initial scan in 2004, where few if any showed. Betcha those collaterals were there back then though....
Did want to point out the consistency of most of the lesions from 2008 thru 2010, with a few exceptions. Symptoms come and go but the lesions stayed fairly consistent. This is good and bad from my POV, insofar as CCSVI is concerned. Some of the lesions are still there, but doggone it all if my heat intolerance, cog-fog, short term memory, FATIGUE, balance and inability to focus for more than short periods has mitigated to the point that sometimes I forget just how screwed up things were a very short time ago.... Is it possible that slowed perfusion contributed to the above mentioned items??? (insert snicker).....
Anyways, no slam dunk as far as the scans go, but in a way I'm kind of glad, it just shows that the symptoms can take a hike and not come back (knock on wood), while the lesions keep chugging along, HOWEVER there was not one new one noted, just for the record, and I looked hard....
Sure would be nice to get SWI scans for everyone starting tomorrow....
Maybe it was mostly my veins after all eh???? ;)
Mark.
I tried to keep it limited to the ones that showed consistently so as to avoid the iffy ones or possible artifacts... (Also keep in mind that this is an 8 month follow up rolled into my 1 year follow up, so maybe another 4 months would show differently??)



This is an assemblage of scans from 2008, 2009 (pre-op), 2009 (2 month follow up), and the latest scan April 2010.
Want to point out a few things though for posterity:
1. Different machines, different operators, different levels of contrast=different scans. Even the 3 at Stanford are all different, though the protocols are similiar, there were 3 different operators. (Aug-Oct-Apr).
2. The slightest variation in patient position in the tube, head slightly forward/back/tilted etc. will yield differing views of the same area, so no two scans are going to be alike. The scan goes the same way every time, the patient does not. So on some of the comparisons there's just no comparable slice. That means no comparable results.
3. MRI's are hereby stipulated as to not proving ANYTHING pro, or con in the CCSVI paradigm, they are just another piece of the puzzle. Obviously we all know that lesion load vs. disability is a non-starter, so lack of lesion load conversely doesn't "prove" anything, but it's nice to see nothing new.
The April scan lesions appear to me to be slightly less contrasted/lit up, but once again that could be an operator variation... The pics seem to be a bit darker overall.
4. Speaking specifically of my own, there were a few areas that exacerbated between the first scan in 2008 and 2009, and definitely a lot more than my initial scan in 2004, where few if any showed. Betcha those collaterals were there back then though....
Did want to point out the consistency of most of the lesions from 2008 thru 2010, with a few exceptions. Symptoms come and go but the lesions stayed fairly consistent. This is good and bad from my POV, insofar as CCSVI is concerned. Some of the lesions are still there, but doggone it all if my heat intolerance, cog-fog, short term memory, FATIGUE, balance and inability to focus for more than short periods has mitigated to the point that sometimes I forget just how screwed up things were a very short time ago.... Is it possible that slowed perfusion contributed to the above mentioned items??? (insert snicker).....
Anyways, no slam dunk as far as the scans go, but in a way I'm kind of glad, it just shows that the symptoms can take a hike and not come back (knock on wood), while the lesions keep chugging along, HOWEVER there was not one new one noted, just for the record, and I looked hard....
Sure would be nice to get SWI scans for everyone starting tomorrow....
Maybe it was mostly my veins after all eh???? ;)
Mark.
I tried to keep it limited to the ones that showed consistently so as to avoid the iffy ones or possible artifacts... (Also keep in mind that this is an 8 month follow up rolled into my 1 year follow up, so maybe another 4 months would show differently??)



RRMS Dx'd 2007, first episode 2004. Bilateral stent placement, 3 on left, 1 stent on right, at Stanford August 2009. Watch my operation video: http://www.youtube.com/watch?v=cwc6QlLVtko, Virtually symptom free since, no relap
- thisisalex
- Family Elder
- Posts: 218
- Joined: Wed Dec 02, 2009 3:00 pm
- Location: Hungary
- Contact:
- CureIous
- Family Elder
- Posts: 1266
- Joined: Tue Jul 14, 2009 2:00 pm
- Location: Riverside, CA
- Contact:
Hi all, this is my official 9 month update, though it is getting a bit redundant, so I tossed in a picture to make it more interestinger.
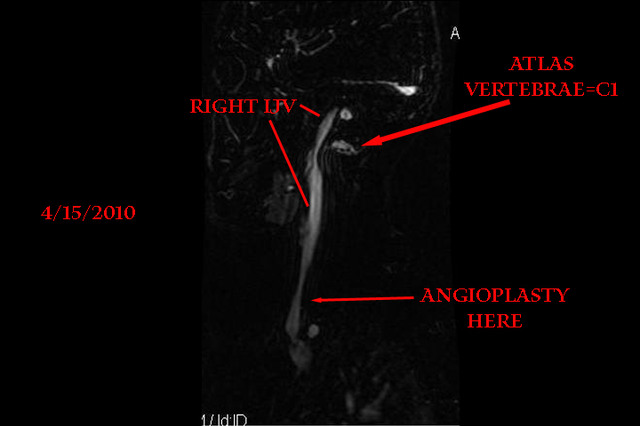
Okay on the upper part, you will see the obvious thin area where the Atlas bone is stressing out the right IJV, this was always there, before the surgery and afterwards. What was stented was further on down below that. This is a very tight area as a few of our pioneers are well aware, and not a spot to be trifled with out of hand.
So basically you had a thin spot, and keep in mind this picture is just one slice, it's not quite as dramatic as it looks on there, but the stenosed area is there, nonetheless. Some of the left IJV is obscuring the view here so there is more drainage area than is readily apparent.
Mind you, none of this showed up on the ultrasound. This is where I take exception to any assertion that this way or that way is the best way to scan, the fact of the matter is, you don't know, and I don't know either, so to tell someone "oh MRV's are junk" because YOU had a negative finding, don't make it so for everyone. Same thing with Ultrasound, it can go either way. If ya can't get it this way>>> go that way<<<< but never give up and take all internet medical advice with a grain of salt, regardless of source, do your own homework, please.
Back to the pic, this got me to thinking about what we've seen so many times already with two very well known areas, the collarbone and atlas vertebrae, where so many stenoses are seen. Came across this:
Titre du document / Document title
Compression of the internal jugular vein by the transverse process of the atlas as the cause of cerebellar hemorrhage after supratentorial craniotomy. Commentary
Auteur(s) / Author(s)
SEOANE E. (1) ; RHOTON A. L. (2) ; YONAS H. (Commentateur) (3) ;
Affiliation(s) du ou des auteurs / Author(s) Affiliation(s)
(1) Department of Microsurgical Anatomy, University of Florida, Gainesville, Florida, ETATS-UNIS
(2) Department of Neurological Surgery, University of Florida, Gainesville, Florida, ETATS-UNIS
(3) Cerebrovascular Surgery, University of Pittsburgh, Pittsburgh, Pennsylvania, ETATS-UNIS
Résumé / Abstract
Abstract
Background
The cerebellar hemorrhage reported in numerous cases after supratentorial craniotomy has uniformly exhibited the characteristics of hemorrhage associated with venous infarction rather than arterial bleeding. The cause has remained obscure, although previous reports suggested that the cause may be obstruction of flow in the internal jugular vein immediately below the base of the skull.
Methods
The microsurgical anatomy of 36 internal jugular veins in the upper cervical region were defined in adult cadaveric specimens using 3–40× magnification with special attention to the relationship of the vein to the atlas.
Results
In every specimen, the posterior wall of the internal jugular vein rested against the transverse process of the atlas as the vein descended immediately below the jugular foramen. In 14 of 36 specimens, the transverse process indented the posterior wall of the vein, causing the vein to be slightly or moderately angulated as it descended across the anterior surface of the transverse process. Three veins were severely kinked as they descended across the transverse process of the atlas.
Conclusions
Obstruction of flow in the internal jugular vein at the site where the vein descends across the transverse process of the atlas is a likely cause of the venous hypertension that has resulted in the cerebellar hemorrhage reported in numerous cases after supratentorial craniotomy. An examination of the biomechanics of the region confirms that turning the head to the side opposite a supratentorial craniotomy and extending the neck, common practices with unilateral supratentorial craniotomy, further aggravates the angulation and obstruction of the internal jugular vein at the transverse process of C1 on the side ipsilateral to the craniotomy.
Now obviously, this relates to people who had died of hemorrhage following brain surgery, but on the venous side and not the arterial side. Venous hypertension, we've sure heard that one before.
Mention this only as it relates to the mechanics involved in some cases of CCSVI that we've seen ample evidence of, where that C1 was pinching off the jugular veins.
You can see where the red Atlas bone abuts the blue IJV in this simple picture:
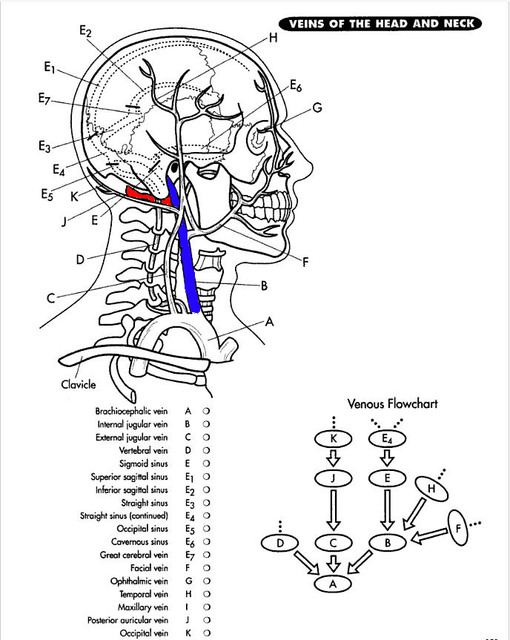
That is precisely the area you are seeing in the scan above.
Understood that this is just a tiny part of a complex, multi-faceted puzzle that is CCSVI/MS, but considering we sleep on that thing and twist it and hyperextend it and pull muscles in and around it, and that it is in a constant state of flux/growth throughout our lives, along with our other bone structures, more specifically our ever-evolving jaw lines, it doesn't take too much of an imagination to see this growth evolving after so many years, and after a tipping point is reached in a goodly number of us, the median years of MS diagnosis in the 30's, the bone growth and change may be implicated here in slowly over many years choking off the return supply from our IJV's to a certain extent, some more than others obviously.
I know this doesn't even touch the azy or explain much more than a simple mechanical issue which may or may not be implicated.
But anytime I see "venous hypertension" my mind says "reflux". I know at least one of our well known detractors (not skeptic, detractor) has insisted our heads would blow up like a balloon if venous hypertension were present, the body has other veins like the vetebrals to take care of the overflow.
Oh really, then why did all these people die of brain bleeds following stenosis of the internal jugular vein after brain surgery? Guess there's more hypertension there than meets the eye eh?
The brain bleeds were on the venous side, not the arterial side. Take a big red crayon and circle that. I see our process, if in fact it goes down that path in the future, as a much slower process than the extreme noted above. The damage accumulates, your veins don't build up enough pressure to rupture or you wouldn't be reading this, but reflux? Slowed perfusion/transition across the brain, lack of freshly oxygenated blood reaching our precious craniums? Fatigue, brain fog, lethargy, lack of short term memory, iron accumulation, cell death, immune system response? Sounds reasonable to me on the face of it...
As far as my anectdotal, placebo initiated effects, they are better than ever and stuck in high gear. I feel like I am only limited by the clock, which gets cursed multiple times per day. I haven't missed a DAY of my newborn son's existence here on earth for the last two months (it's his two month bday today), not one solitary hour, have been there, and I mean REALLY been there, in the game, aware and cognizant of everything that is happening and enjoying every last drop.
Like last week, I phoned my Dr's office on Monday to make an obligatory follow up appt after my angioplasty at Stanford last month. I was told the first available was Thursday at 2:15. No problem. Except I didn't write it down, I didn't need to do that. In the past, if that appt. time wasn't written down before they hung up the phone, I was guaranteed to require an embarrassing phone call to "confirm the time", when in fact it was forgotten the second the phone was hung up.
Now, it's absolutely effortless, it just comes without trying. That carries much farther into one's life than mere minutae like Dr.'s appointments. It impacts to the good, every waking moment, just like the opposite impacted to the negative, every waking moment.
And that is why us stentees are still here to keep the hope alive.
Don't EVER give up.
Mark.
p.s. my Dr. is VERY excited and always has been about all of this and is networking big time. He's had every scan taken in his hands and is passing it around. He's also friends with my neuro. Just lucked out on that is all. I try very hard to funnel them as much info as they will take. They have many MS patients between them. Dr's are human too, some can't help to get excited when they see something that has really and truly had a tremendous impact.
Wanted also to mention that thin area up high is where the pressure gradient was measured, before and after my follow up angioplasty. The gradient went from 4 to 0. The collaterals diminished substantially as well. To recap: the valve down below (where the arrow points to) was basically a flap obstructing the flow, all issues of stenosis and narrowing notwithstanding. That's the area that was ballooned. My right ear venous hum has dimished as well, my estimate 50-65% reduction and very tolerable now!!!!!! Instead of a chorus of alternating sounds, it's more steady, lower in volume and therefore much less noticeable. Makes sense, if the flap is holding up the flow, and it's been "unstuck" then the flow is more laminar and less stop-and-go, which creates the variations in pitch!

Okay on the upper part, you will see the obvious thin area where the Atlas bone is stressing out the right IJV, this was always there, before the surgery and afterwards. What was stented was further on down below that. This is a very tight area as a few of our pioneers are well aware, and not a spot to be trifled with out of hand.
So basically you had a thin spot, and keep in mind this picture is just one slice, it's not quite as dramatic as it looks on there, but the stenosed area is there, nonetheless. Some of the left IJV is obscuring the view here so there is more drainage area than is readily apparent.
Mind you, none of this showed up on the ultrasound. This is where I take exception to any assertion that this way or that way is the best way to scan, the fact of the matter is, you don't know, and I don't know either, so to tell someone "oh MRV's are junk" because YOU had a negative finding, don't make it so for everyone. Same thing with Ultrasound, it can go either way. If ya can't get it this way>>> go that way<<<< but never give up and take all internet medical advice with a grain of salt, regardless of source, do your own homework, please.
Back to the pic, this got me to thinking about what we've seen so many times already with two very well known areas, the collarbone and atlas vertebrae, where so many stenoses are seen. Came across this:
Titre du document / Document title
Compression of the internal jugular vein by the transverse process of the atlas as the cause of cerebellar hemorrhage after supratentorial craniotomy. Commentary
Auteur(s) / Author(s)
SEOANE E. (1) ; RHOTON A. L. (2) ; YONAS H. (Commentateur) (3) ;
Affiliation(s) du ou des auteurs / Author(s) Affiliation(s)
(1) Department of Microsurgical Anatomy, University of Florida, Gainesville, Florida, ETATS-UNIS
(2) Department of Neurological Surgery, University of Florida, Gainesville, Florida, ETATS-UNIS
(3) Cerebrovascular Surgery, University of Pittsburgh, Pittsburgh, Pennsylvania, ETATS-UNIS
Résumé / Abstract
Abstract
Background
The cerebellar hemorrhage reported in numerous cases after supratentorial craniotomy has uniformly exhibited the characteristics of hemorrhage associated with venous infarction rather than arterial bleeding. The cause has remained obscure, although previous reports suggested that the cause may be obstruction of flow in the internal jugular vein immediately below the base of the skull.
Methods
The microsurgical anatomy of 36 internal jugular veins in the upper cervical region were defined in adult cadaveric specimens using 3–40× magnification with special attention to the relationship of the vein to the atlas.
Results
In every specimen, the posterior wall of the internal jugular vein rested against the transverse process of the atlas as the vein descended immediately below the jugular foramen. In 14 of 36 specimens, the transverse process indented the posterior wall of the vein, causing the vein to be slightly or moderately angulated as it descended across the anterior surface of the transverse process. Three veins were severely kinked as they descended across the transverse process of the atlas.
Conclusions
Obstruction of flow in the internal jugular vein at the site where the vein descends across the transverse process of the atlas is a likely cause of the venous hypertension that has resulted in the cerebellar hemorrhage reported in numerous cases after supratentorial craniotomy. An examination of the biomechanics of the region confirms that turning the head to the side opposite a supratentorial craniotomy and extending the neck, common practices with unilateral supratentorial craniotomy, further aggravates the angulation and obstruction of the internal jugular vein at the transverse process of C1 on the side ipsilateral to the craniotomy.
Now obviously, this relates to people who had died of hemorrhage following brain surgery, but on the venous side and not the arterial side. Venous hypertension, we've sure heard that one before.
Mention this only as it relates to the mechanics involved in some cases of CCSVI that we've seen ample evidence of, where that C1 was pinching off the jugular veins.
You can see where the red Atlas bone abuts the blue IJV in this simple picture:

That is precisely the area you are seeing in the scan above.
Understood that this is just a tiny part of a complex, multi-faceted puzzle that is CCSVI/MS, but considering we sleep on that thing and twist it and hyperextend it and pull muscles in and around it, and that it is in a constant state of flux/growth throughout our lives, along with our other bone structures, more specifically our ever-evolving jaw lines, it doesn't take too much of an imagination to see this growth evolving after so many years, and after a tipping point is reached in a goodly number of us, the median years of MS diagnosis in the 30's, the bone growth and change may be implicated here in slowly over many years choking off the return supply from our IJV's to a certain extent, some more than others obviously.
I know this doesn't even touch the azy or explain much more than a simple mechanical issue which may or may not be implicated.
But anytime I see "venous hypertension" my mind says "reflux". I know at least one of our well known detractors (not skeptic, detractor) has insisted our heads would blow up like a balloon if venous hypertension were present, the body has other veins like the vetebrals to take care of the overflow.
Oh really, then why did all these people die of brain bleeds following stenosis of the internal jugular vein after brain surgery? Guess there's more hypertension there than meets the eye eh?
The brain bleeds were on the venous side, not the arterial side. Take a big red crayon and circle that. I see our process, if in fact it goes down that path in the future, as a much slower process than the extreme noted above. The damage accumulates, your veins don't build up enough pressure to rupture or you wouldn't be reading this, but reflux? Slowed perfusion/transition across the brain, lack of freshly oxygenated blood reaching our precious craniums? Fatigue, brain fog, lethargy, lack of short term memory, iron accumulation, cell death, immune system response? Sounds reasonable to me on the face of it...
As far as my anectdotal, placebo initiated effects, they are better than ever and stuck in high gear. I feel like I am only limited by the clock, which gets cursed multiple times per day. I haven't missed a DAY of my newborn son's existence here on earth for the last two months (it's his two month bday today), not one solitary hour, have been there, and I mean REALLY been there, in the game, aware and cognizant of everything that is happening and enjoying every last drop.
Like last week, I phoned my Dr's office on Monday to make an obligatory follow up appt after my angioplasty at Stanford last month. I was told the first available was Thursday at 2:15. No problem. Except I didn't write it down, I didn't need to do that. In the past, if that appt. time wasn't written down before they hung up the phone, I was guaranteed to require an embarrassing phone call to "confirm the time", when in fact it was forgotten the second the phone was hung up.
Now, it's absolutely effortless, it just comes without trying. That carries much farther into one's life than mere minutae like Dr.'s appointments. It impacts to the good, every waking moment, just like the opposite impacted to the negative, every waking moment.
And that is why us stentees are still here to keep the hope alive.
Don't EVER give up.
Mark.
p.s. my Dr. is VERY excited and always has been about all of this and is networking big time. He's had every scan taken in his hands and is passing it around. He's also friends with my neuro. Just lucked out on that is all. I try very hard to funnel them as much info as they will take. They have many MS patients between them. Dr's are human too, some can't help to get excited when they see something that has really and truly had a tremendous impact.
Wanted also to mention that thin area up high is where the pressure gradient was measured, before and after my follow up angioplasty. The gradient went from 4 to 0. The collaterals diminished substantially as well. To recap: the valve down below (where the arrow points to) was basically a flap obstructing the flow, all issues of stenosis and narrowing notwithstanding. That's the area that was ballooned. My right ear venous hum has dimished as well, my estimate 50-65% reduction and very tolerable now!!!!!! Instead of a chorus of alternating sounds, it's more steady, lower in volume and therefore much less noticeable. Makes sense, if the flap is holding up the flow, and it's been "unstuck" then the flow is more laminar and less stop-and-go, which creates the variations in pitch!
RRMS Dx'd 2007, first episode 2004. Bilateral stent placement, 3 on left, 1 stent on right, at Stanford August 2009. Watch my operation video: http://www.youtube.com/watch?v=cwc6QlLVtko, Virtually symptom free since, no relap
- cheerleader
- Family Elder
- Posts: 5361
- Joined: Mon Sep 10, 2007 2:00 pm
- Location: southern California
MARK!! Thank you so much for this very detailed and wonderfully geeky and thorough explanation. I'm SO glad you are one of the frontiersman with Jeff on this journey. He has had similar stuff to you (ear whooshing/positional headaches) and your diagram really clarified so much. It appears positional changes can catch and crimp that jugular vein with the bottom of the skull or the atlas. Glad Dr. D. found your flap and got that out of the way. Jeff goes up on May 12, and the good doctor knows even more about what to look for, thanks to your cutting the line. Thanks, buddy.
I don't think people understand how indebted they are to you and the pioneers. So much will be learned and this procedure will be routine in no time. Glad to hear the kids have their energetic and tech savvy Daddy back. Keep us posted, and thanks so much for sticking around here. We need to hear from the original group.
cheer
I don't think people understand how indebted they are to you and the pioneers. So much will be learned and this procedure will be routine in no time. Glad to hear the kids have their energetic and tech savvy Daddy back. Keep us posted, and thanks so much for sticking around here. We need to hear from the original group.
cheer
Husband dx RRMS 3/07
dx dual jugular vein stenosis (CCSVI) 4/09
http://ccsviinms.blogspot.com
dx dual jugular vein stenosis (CCSVI) 4/09
http://ccsviinms.blogspot.com
- magoo
- Family Elder
- Posts: 574
- Joined: Thu Sep 10, 2009 2:00 pm
- Location: Charlotte, NC
- Contact:
Mark,
Very cool find! I am so happy for you and your family! I have to say when I read about you not writing down your appt. time, I realized today I did the same. I made an appt. to take my car in and just hung up knowing I wouldn't forget. Before, I was exactly like you and would have forgotten before I hung up. Wow, the little things we take for granted now!!! So awesome!
Very cool find! I am so happy for you and your family! I have to say when I read about you not writing down your appt. time, I realized today I did the same. I made an appt. to take my car in and just hung up knowing I wouldn't forget. Before, I was exactly like you and would have forgotten before I hung up. Wow, the little things we take for granted now!!! So awesome!
Rhonda~
Treated by Dake 10/19/09, McGuckin 4/25/11 and 3/9/12- blockages in both IJVs, azy, L-iliac, L-renal veins. CCSVI changed my life and disease.
Treated by Dake 10/19/09, McGuckin 4/25/11 and 3/9/12- blockages in both IJVs, azy, L-iliac, L-renal veins. CCSVI changed my life and disease.
- QueenMum
- Family Member
- Posts: 41
- Joined: Sat Oct 10, 2009 2:00 pm
- Contact:
- jimmylegs
- Volunteer Moderator
- Posts: 12592
- Joined: Sat Mar 11, 2006 3:00 pm
- thisisalex
- Family Elder
- Posts: 218
- Joined: Wed Dec 02, 2009 3:00 pm
- Location: Hungary
- Contact:
Mark, could you please clarify, why the stenosis next to the Atlas wasnt stented? isnt it the origin of your problems?CureIous wrote:
Okay on the upper part, you will see the obvious thin area where the Atlas bone is stressing out the right IJV, this was always there, before the surgery and afterwards. What was stented was further on down below that.
thanks
Alex
- CureIous
- Family Elder
- Posts: 1266
- Joined: Tue Jul 14, 2009 2:00 pm
- Location: Riverside, CA
- Contact:
Excellent question Alex. The time that I went up was in the transitional phase, when he was going from the larger stents to the smaller stents (or so is my understanding, open to correction), meaning in diameter of course. As evidenced by Lew and Marie and others before me, the ACC nerve runs through that particular area and it is a tight area to add anything that exerts pressure, like a stent. In my particular case, there was enough down below to tend to, especially the left side which was narrow and stenosed, along with the lower stuff on the right, it just wasn't feasible to put more than 4 stents all at once. Better to wait for later and see how things shake out, plus the gradients weren't showing as particularly offensive. Over time, the area lower than the lone stenting on the right was seen as an avenue to angioplasty, rather than risk doing something up higher which could end up more trouble than it was worth, which in the end was a good game plan. Angio is way easier than stenting. No thinners, no 2 month follow up, no INR's etc etc. Plus my main complaint was mitigated as mentioned, 50-65%, and the gradient was reduced to nothing at that upper location. Although it *appears* to be pinched off substantially, in reality getting all the shots together shows that not to be the case. It's a bit thin, but not choking anything off and no pressure gradients. It's like blowing air through a whistle. Still getting through, just not as efficiently, but not bouncing back either, witnessed by the gradient reduction to zero...thisisalex wrote:Mark, could you please clarify, why the stenosis next to the Atlas wasnt stented? isnt it the origin of your problems?CureIous wrote:
Okay on the upper part, you will see the obvious thin area where the Atlas bone is stressing out the right IJV, this was always there, before the surgery and afterwards. What was stented was further on down below that.
thanks
Alex
Hope that helps to explain it a bit better!
Mark.
RRMS Dx'd 2007, first episode 2004. Bilateral stent placement, 3 on left, 1 stent on right, at Stanford August 2009. Watch my operation video: http://www.youtube.com/watch?v=cwc6QlLVtko, Virtually symptom free since, no relap
- CureIous
- Family Elder
- Posts: 1266
- Joined: Tue Jul 14, 2009 2:00 pm
- Location: Riverside, CA
- Contact:
Hi guys and gals, little late for my 10 month post-op post, but who's counting?
Just had my longer term follow up with the neuro today, which we agreed back 6 months ago would be a good thing, despite being off any DMD's since well before the operation. (and not because of the operation alone). He of course after listening to my techno surgical follow up blather, asked, "yes, but how do you FEEL", lol. Hey good question doc! As a matter of fact, feel just as fit as a fiddle. At my suggestion, we are doing an EVP next week, having had a good baseline back in 2008 which showed a noticeable imbalance between right/left auditory and ocular responses, forget which side was affected, will get back on that one.
This will be interesting to find out, something a bit more concrete and not as placebo affected as saying, "hey, I lost all heat fatigue doc aint that great!?". (not only lost it, it's still gone after 10 months, yippee!)
I also brought him my latest CD from the follow up procedure in April along with the pathology/post-op report which is a real humdinger in and of itself, wish could post the pics, but promised I wouldn't until all the study stuff is done. The pathology report though is another thing, since that can be anonymized to protect the innocent (snicker).
...blah blah put in catheter, do internal ultrasound, "demonstrated a high grade 90% stenosis upper right IJV near C1-2 vetebral bodies. (think where your skull rests on the top vetebrae or reference above posts).
This...associated with robust collateral network of veins througout the neck, located posteriorly with the neck corresponding to epidural and vetebral veins, pressure gradient was 4 mmHg across the narrowing.
Prior to ballooning, intravascular ultrasounding was introduced to get a better look, which failed to demonstrate a normal valve, NO INDIVIDUAL VALVE CUSPS WERE NOTED, however, a longitudinal membrane or septum was apparent coursing from approx. 5 cm above the confluence with the subclavian vein to just above the branchiocephalic. This membrane appeared quite thin, but was conspicuous, it was not apparent on contrast venography. (People, please underline that and make a bumper sticker for all those who may think their MRV and/or UT and/or venogram was negative, therefore they have no CCSVI, they have NOT explored all possibilities yet!) Maybe on the uber-pros doing the trans cranial thing with proper training, but for most regular Joes, forget it, these little buggers can be hiding in plain sight, they must be LOOKED for specifically. End rant, back to report.
Inflate 12mm angio balloon, no improvement in stenosis up high (remember, the angio was conducted way down below where the faux-valve is obstructing the flow, NOT up high at the skull level, bumper sticker that one too please). No improvement at this point in either collateral network, or stenosis, but the pressure gradient had reduced to 2 mmHg!
Inflate 14mm balloon, visual appearance of "up higher" stenosis reduced by 20%, however, collateral network at this time all but vanished. (the pics are dramatic). Pressure gradient reduced to 0.00.
Re-insert IVUS for a looksee at our septum flap/doohickey, "obvious disruption of the septum" was noted, was fairly pulsating, i.e. "flapping in the breeze".
Sorry for the super simple paraphrasing, but there's not much more beyond what is stated other than the usual jargon.
I know last year post-op I took the kids up that big hill, just to see if I could in the heat, and did great!
This year, I carried my 3 year old on left arm, held another kid's hand who was scared and led an entire group up the hill at the school picnic a few weeks ago, (solo!) I was um, "volunteered" when taking my kid up, and kept all the kids safe going up and back down, it was fun and no stress at all! This I guess was the true victory lap, being requistioned for stuff and not getting that panicked feeling of, "oh boy you just asked the WRONG person to keep his wits about him lol". Good times.

Aint that what's it's all about in the end???
Final thought, everyone is different in their MS and guaranteed you will be different in all ways when it comes to Funky Vein Syndrome, after 4 stents we thought this was licked except for the upper stenosis, but lo and behold, a bugger of a malformed valve can cause a pressure gradient to appear up high, collats and the like, despite the fact that another nearby stenosis had been stented already.
So what if this valve had been like this from birth , totally malformed, always causing problems upstream but not enough to create a pathology quite yet, but given time and enough consistent "non-inflation" of the vein up high, the bone gets free reign to grow out and protude into the void, later one we see the end result, a severe stenosis, bone causing vein to be stenosed, but bone grows where it may and absent any pressure can grow and protude at will, albeit very slowly and in minute amounts (remember we are talking mm's here!). Hope that makes sense. The properly functioning valve iow, would have allowed full inflation upstream, and that pressure would have kept the bone "at bay", never to present a problem. I speak specifically of the right side, we don't know what the internals of the left look like, I suspect the valve on that side may be a bit wonky too.
I do hope everyone's ears ring soundly with the thought that our "gold plated standard" is gold, but it aint perfect, and it CAN MISS things, even gold has impurities in it.
Myself, I think of all these different onion layers that must be peeled back, some get it on the first layer, one ultrasound and BAM they are dx'd, some get it on the first MRV, BAM there it is, some can't get definitive until a CT, or a venogram, some may need any combination of the above, AND an internal ultrasound to verify valve competence. There's only so many transcranial dopplers in the world with properly trained techs, and even then I wonder how "see-able" this is, mine was directly under the collarbone.
So don't give up, please don't give up, please please PLEASE don't give up until you have exhausted every possible angle, even then there may be more that we don't know!
Dios Bendiga.
Mark.
Just had my longer term follow up with the neuro today, which we agreed back 6 months ago would be a good thing, despite being off any DMD's since well before the operation. (and not because of the operation alone). He of course after listening to my techno surgical follow up blather, asked, "yes, but how do you FEEL", lol. Hey good question doc! As a matter of fact, feel just as fit as a fiddle. At my suggestion, we are doing an EVP next week, having had a good baseline back in 2008 which showed a noticeable imbalance between right/left auditory and ocular responses, forget which side was affected, will get back on that one.
This will be interesting to find out, something a bit more concrete and not as placebo affected as saying, "hey, I lost all heat fatigue doc aint that great!?". (not only lost it, it's still gone after 10 months, yippee!)
I also brought him my latest CD from the follow up procedure in April along with the pathology/post-op report which is a real humdinger in and of itself, wish could post the pics, but promised I wouldn't until all the study stuff is done. The pathology report though is another thing, since that can be anonymized to protect the innocent (snicker).
...blah blah put in catheter, do internal ultrasound, "demonstrated a high grade 90% stenosis upper right IJV near C1-2 vetebral bodies. (think where your skull rests on the top vetebrae or reference above posts).
This...associated with robust collateral network of veins througout the neck, located posteriorly with the neck corresponding to epidural and vetebral veins, pressure gradient was 4 mmHg across the narrowing.
Prior to ballooning, intravascular ultrasounding was introduced to get a better look, which failed to demonstrate a normal valve, NO INDIVIDUAL VALVE CUSPS WERE NOTED, however, a longitudinal membrane or septum was apparent coursing from approx. 5 cm above the confluence with the subclavian vein to just above the branchiocephalic. This membrane appeared quite thin, but was conspicuous, it was not apparent on contrast venography. (People, please underline that and make a bumper sticker for all those who may think their MRV and/or UT and/or venogram was negative, therefore they have no CCSVI, they have NOT explored all possibilities yet!) Maybe on the uber-pros doing the trans cranial thing with proper training, but for most regular Joes, forget it, these little buggers can be hiding in plain sight, they must be LOOKED for specifically. End rant, back to report.
Inflate 12mm angio balloon, no improvement in stenosis up high (remember, the angio was conducted way down below where the faux-valve is obstructing the flow, NOT up high at the skull level, bumper sticker that one too please). No improvement at this point in either collateral network, or stenosis, but the pressure gradient had reduced to 2 mmHg!
Inflate 14mm balloon, visual appearance of "up higher" stenosis reduced by 20%, however, collateral network at this time all but vanished. (the pics are dramatic). Pressure gradient reduced to 0.00.
Re-insert IVUS for a looksee at our septum flap/doohickey, "obvious disruption of the septum" was noted, was fairly pulsating, i.e. "flapping in the breeze".
Sorry for the super simple paraphrasing, but there's not much more beyond what is stated other than the usual jargon.
I know last year post-op I took the kids up that big hill, just to see if I could in the heat, and did great!
This year, I carried my 3 year old on left arm, held another kid's hand who was scared and led an entire group up the hill at the school picnic a few weeks ago, (solo!) I was um, "volunteered" when taking my kid up, and kept all the kids safe going up and back down, it was fun and no stress at all! This I guess was the true victory lap, being requistioned for stuff and not getting that panicked feeling of, "oh boy you just asked the WRONG person to keep his wits about him lol". Good times.

Aint that what's it's all about in the end???
Final thought, everyone is different in their MS and guaranteed you will be different in all ways when it comes to Funky Vein Syndrome, after 4 stents we thought this was licked except for the upper stenosis, but lo and behold, a bugger of a malformed valve can cause a pressure gradient to appear up high, collats and the like, despite the fact that another nearby stenosis had been stented already.
So what if this valve had been like this from birth , totally malformed, always causing problems upstream but not enough to create a pathology quite yet, but given time and enough consistent "non-inflation" of the vein up high, the bone gets free reign to grow out and protude into the void, later one we see the end result, a severe stenosis, bone causing vein to be stenosed, but bone grows where it may and absent any pressure can grow and protude at will, albeit very slowly and in minute amounts (remember we are talking mm's here!). Hope that makes sense. The properly functioning valve iow, would have allowed full inflation upstream, and that pressure would have kept the bone "at bay", never to present a problem. I speak specifically of the right side, we don't know what the internals of the left look like, I suspect the valve on that side may be a bit wonky too.
I do hope everyone's ears ring soundly with the thought that our "gold plated standard" is gold, but it aint perfect, and it CAN MISS things, even gold has impurities in it.
Myself, I think of all these different onion layers that must be peeled back, some get it on the first layer, one ultrasound and BAM they are dx'd, some get it on the first MRV, BAM there it is, some can't get definitive until a CT, or a venogram, some may need any combination of the above, AND an internal ultrasound to verify valve competence. There's only so many transcranial dopplers in the world with properly trained techs, and even then I wonder how "see-able" this is, mine was directly under the collarbone.
So don't give up, please don't give up, please please PLEASE don't give up until you have exhausted every possible angle, even then there may be more that we don't know!
Dios Bendiga.
Mark.
RRMS Dx'd 2007, first episode 2004. Bilateral stent placement, 3 on left, 1 stent on right, at Stanford August 2009. Watch my operation video: http://www.youtube.com/watch?v=cwc6QlLVtko, Virtually symptom free since, no relap
- cheerleader
- Family Elder
- Posts: 5361
- Joined: Mon Sep 10, 2007 2:00 pm
- Location: southern California
-
ErikaSlovakia
- Family Elder
- Posts: 1125
- Joined: Wed Jul 29, 2009 2:00 pm
- Location: Slovakia, Europe
- Contact:
- magoo
- Family Elder
- Posts: 574
- Joined: Thu Sep 10, 2009 2:00 pm
- Location: Charlotte, NC
- Contact:
Yes Mark, there is still so much more to learn! Thank you for your detailed report and for keeping Dr. Dake on his toes! 
I think we should use your new name for CCSVI...Funky Vein Syndrome!! I am so glad you continue to enjoy good health.
I am so glad you continue to enjoy good health.
I think we should use your new name for CCSVI...Funky Vein Syndrome!!
Rhonda~
Treated by Dake 10/19/09, McGuckin 4/25/11 and 3/9/12- blockages in both IJVs, azy, L-iliac, L-renal veins. CCSVI changed my life and disease.
Treated by Dake 10/19/09, McGuckin 4/25/11 and 3/9/12- blockages in both IJVs, azy, L-iliac, L-renal veins. CCSVI changed my life and disease.



