CCSVI tracking project-POST PER P.1 FORMAT ONLY
-
radeck
- Family Elder
- Posts: 398
- Joined: Mon Feb 16, 2009 3:00 pm
- Contact:
CCSVI tracking project-POST PER P.1 FORMAT ONLY
[The following introduction and example format is open for edits based on comments from TIMS users. Comments can be discussed in the thread that initiated this one here: http://www.thisisms.com/ftopic-8295-15- ... rasc-.html or via pm. Thank you.]
The purpose of this thread is to get an overview of the experiences of patients getting tested for CCSVI and those receiving treatment (ballooning, stents, open neck surgery, or other), be it in Italy, Poland, USA, or elsewhere (we hope to include translations of this introductory post in the near future). Now there has been a "patient log" thread here already, but it ended up loosing structure as newbie's and other's who got exited commented on patients logs. Here we hope to collect as many accounts as possible, neatly organized without interruptions so that newbie's and others can get an overview of diagnoses and of side effects and subjective as well as objective efficacy of the treatment. For quantitative tracking purposes, the FSS, MSIS, and/or EDSS scores, as well as number of relapses (if applicable) will be important. Once tabulated, this will allow us to show a snapshot of group progress.
So, the idea of this thread is to have one post per patient, each of which will hopefully be updated regularly using the "Edit" feature, basically however often patients like (though probably not too often as this might make the long term development hard to follow). Edits should be to the point and could include past MRI and other test results, original CCSVI testing results, side of major IJV stenosis (if applicable), side of most lesions as well as symptoms, experiences with the treatment and post-treatment medications, and perhaps most importantly, CCSVI/MS symptoms pre and post treatment.
Finally, if you could post MRV and other images, that would be fantastic to give people a feel for what kinds of malformations we're looking at. I found http://photobucket.com/ a hassle-free site for uploading and hosting images anonymously.
For the sake of keeping the thread neatly organized, we ask others to refrain from posting comments on patients logs. Comments outside of personal CCSVI accounts will be erased by the moderator.
=======================================================
[JL edit: please use the post subject field to specify 'positive' 'neutral' 'negative' 'pending' or similar, re response to treatment, so that readers have a quick way to assess individual response. the subject field can also be edited over time as appropriate.]
CCSVI TRACKING [Please use date format MM/DD/YYYY]
MS HISTORY
Name (if want to give other than TIMS login name):
Male/Female: (M/F)
Age:
Date(s) & type of neurological diagnosis (RRMS, SPMS, PPMS, CIS, or other):
Lesion locations (most affected side, if known), number:
MS treatments:
MS symptoms before stenosis intervention:
Number of relapses before intervention (if applicable):
EDSS before CCSVI intervention (self-assessed or physician-assessed?):
[To review EDSS rating, click the following link: http://www.mult-sclerosis.org/expandedd ... scale.html ]
FSS before CCSVI intervention:
[To calculate FSS rating, click the following link: http://www.mult-sclerosis.org/fatigueseverityscale.html ]
MSIS before CCSVI intervention:
[To calculate MSIS rating , click the following link: http://healingpowernow.com/msis.htm ]
Are you using Inclined Bed Therapy I.B.T? (Y/N)
Have you had testing (and possibly procedure) for blockage yet: (Y/N)
[Some patients may wish to start with a baseline report, if Y, continue with next section]
STENOSIS PROCEDURE HISTORY
Date/location of testing/procedure:
Type of venographic study: (MRV, Doppler)
Diagnosis:
Type of procedure:
Procedure/drug related symptoms:
[Repeat this section if there have been more than one procedure]
Number of relapses since first CCSVI intervention:
Impact on your MS symptoms in words (include date in brackets if there have been multiple updates):
EDSS as of this update (self-assessed or physician-assessed?)
FSS as of this update:
MSIS as of this update:
The purpose of this thread is to get an overview of the experiences of patients getting tested for CCSVI and those receiving treatment (ballooning, stents, open neck surgery, or other), be it in Italy, Poland, USA, or elsewhere (we hope to include translations of this introductory post in the near future). Now there has been a "patient log" thread here already, but it ended up loosing structure as newbie's and other's who got exited commented on patients logs. Here we hope to collect as many accounts as possible, neatly organized without interruptions so that newbie's and others can get an overview of diagnoses and of side effects and subjective as well as objective efficacy of the treatment. For quantitative tracking purposes, the FSS, MSIS, and/or EDSS scores, as well as number of relapses (if applicable) will be important. Once tabulated, this will allow us to show a snapshot of group progress.
So, the idea of this thread is to have one post per patient, each of which will hopefully be updated regularly using the "Edit" feature, basically however often patients like (though probably not too often as this might make the long term development hard to follow). Edits should be to the point and could include past MRI and other test results, original CCSVI testing results, side of major IJV stenosis (if applicable), side of most lesions as well as symptoms, experiences with the treatment and post-treatment medications, and perhaps most importantly, CCSVI/MS symptoms pre and post treatment.
Finally, if you could post MRV and other images, that would be fantastic to give people a feel for what kinds of malformations we're looking at. I found http://photobucket.com/ a hassle-free site for uploading and hosting images anonymously.
For the sake of keeping the thread neatly organized, we ask others to refrain from posting comments on patients logs. Comments outside of personal CCSVI accounts will be erased by the moderator.
=======================================================
[JL edit: please use the post subject field to specify 'positive' 'neutral' 'negative' 'pending' or similar, re response to treatment, so that readers have a quick way to assess individual response. the subject field can also be edited over time as appropriate.]
CCSVI TRACKING [Please use date format MM/DD/YYYY]
MS HISTORY
Name (if want to give other than TIMS login name):
Male/Female: (M/F)
Age:
Date(s) & type of neurological diagnosis (RRMS, SPMS, PPMS, CIS, or other):
Lesion locations (most affected side, if known), number:
MS treatments:
MS symptoms before stenosis intervention:
Number of relapses before intervention (if applicable):
EDSS before CCSVI intervention (self-assessed or physician-assessed?):
[To review EDSS rating, click the following link: http://www.mult-sclerosis.org/expandedd ... scale.html ]
FSS before CCSVI intervention:
[To calculate FSS rating, click the following link: http://www.mult-sclerosis.org/fatigueseverityscale.html ]
MSIS before CCSVI intervention:
[To calculate MSIS rating , click the following link: http://healingpowernow.com/msis.htm ]
Are you using Inclined Bed Therapy I.B.T? (Y/N)
Have you had testing (and possibly procedure) for blockage yet: (Y/N)
[Some patients may wish to start with a baseline report, if Y, continue with next section]
STENOSIS PROCEDURE HISTORY
Date/location of testing/procedure:
Type of venographic study: (MRV, Doppler)
Diagnosis:
Type of procedure:
Procedure/drug related symptoms:
[Repeat this section if there have been more than one procedure]
Number of relapses since first CCSVI intervention:
Impact on your MS symptoms in words (include date in brackets if there have been multiple updates):
EDSS as of this update (self-assessed or physician-assessed?)
FSS as of this update:
MSIS as of this update:
Last edited by radeck on Sun Feb 14, 2010 2:07 pm, edited 19 times in total.
- Sharon
- Family Elder
- Posts: 1286
- Joined: Sun Nov 07, 2004 3:00 pm
- Location: Colorado
- Contact:
Patient Name: Sharon
MS History
Female
Age: 66
Diagnosed 2003 RRMS
Lesion locations : cervical spine C2-C4; low lesion burden in subcortical and periventricular white matter.
MS treatments: Diet, exercise, LDN since May of 2008
MS symptoms before stenosis intervention: left side weakness, foot drop, loss left palmar muscle wasting, little cognitive impairment, slight imbalance when ambulating, tinnitus. Use WalkAide
EDSS before stenosis intervention 4-4.5
Stenosis Procedure History
June 2, 2009 - Stanford Hospital
MRV/MRI - Ultrasound
Diagnosis: Narrowing of the left IJ vein extending approx. 6 cm below
the left jugular bulb. Left jugular venography showed long segment of stenosis with significant collateral venous channels.
Procedure: Stenting of the left IJ vein with a 10 mm self-expanding stent and 2nd stent placement at valve at the junciton with left brachioceohalci vein.
Procedure/drug related symptoms: Major problems with muscle spasming in neck (levator muscle) and shoulder; treated with massage, muscle relaxors, acupuncture. Four months out from surgery and shoulder is at 90%.
Number of relapses since CCSVI intervention: -0-
Impact on MS symptoms: Less spasticity in left leg; facial pain is gone; right side back pain is gone; normal sweating; high altitude headaches gone; walking gait is smoother. No progression since intervention.
EDSS 10/5/2009 - 4.0
FSS 10/5/2009 - 2.88 - Fatigue has not been a symptom for me
MSIS 10/5/09 - 61 -
Sharon
MS History
Female
Age: 66
Diagnosed 2003 RRMS
Lesion locations : cervical spine C2-C4; low lesion burden in subcortical and periventricular white matter.
MS treatments: Diet, exercise, LDN since May of 2008
MS symptoms before stenosis intervention: left side weakness, foot drop, loss left palmar muscle wasting, little cognitive impairment, slight imbalance when ambulating, tinnitus. Use WalkAide
EDSS before stenosis intervention 4-4.5
Stenosis Procedure History
June 2, 2009 - Stanford Hospital
MRV/MRI - Ultrasound
Diagnosis: Narrowing of the left IJ vein extending approx. 6 cm below
the left jugular bulb. Left jugular venography showed long segment of stenosis with significant collateral venous channels.
Procedure: Stenting of the left IJ vein with a 10 mm self-expanding stent and 2nd stent placement at valve at the junciton with left brachioceohalci vein.
Procedure/drug related symptoms: Major problems with muscle spasming in neck (levator muscle) and shoulder; treated with massage, muscle relaxors, acupuncture. Four months out from surgery and shoulder is at 90%.
Number of relapses since CCSVI intervention: -0-
Impact on MS symptoms: Less spasticity in left leg; facial pain is gone; right side back pain is gone; normal sweating; high altitude headaches gone; walking gait is smoother. No progression since intervention.
EDSS 10/5/2009 - 4.0
FSS 10/5/2009 - 2.88 - Fatigue has not been a symptom for me
MSIS 10/5/09 - 61 -
Sharon
Last edited by Sharon on Fri Oct 16, 2009 1:34 pm, edited 1 time in total.
- mrhodes40
- Family Elder
- Posts: 2068
- Joined: Thu Sep 23, 2004 2:00 pm
- Location: USA
- Contact:
MS HISTORY for Marie
Female
Age: 48
Diagnosis: 1991 Dx RRMS, May of '08 SPMS
Lesion locations: 4 Perventricular lesions left hemisphere seen on 1.5 MRI, right sided weakness. All spinal MRI's clear. No inflammation for years on MRI, no enhancement.
MS treatments: Copaxone, supplements, failed treatments: MTX x 1.5 yr, plaquenil x 4yr (I have RA too), LDNx2yr, ABX x 3+yr,
MS symptoms before stenosis intervention: Severe drop foot right (foot is totally incapable of function, can't even willingly move a toe; really limp) right sided hand weakness, writing is difficult. Cane dependent, Rollator for long distances (mall etc). No cognitive issues. Mild urinary retention and voiding 4-5 times at night. Flexor spasms at night requiring Baclofen and Requip for many years. A test of a Walkaide functional electrical stimulator failed due to spasms. Stiffness upon standing. Sleeping difficulties; wakefulness and chronic daytime fatigue with Epworth sleepiness scales ranging from 11-17 over the last 2 years on MD assessment sheets.
Number of relapses before intervention (if applicable): none.
EDSS before stenosis intervention: 6+ self assessed. I use the rollator for long distances which is "bilateral support" but I can walk with the cane for 100 yards so is that a 6 (unilateral support) or more?
MSIS (estimated 10/09) before procedure 106
FSS before procedure (from my own MD records) 6
STENOSIS PROCEDURE HISTORY
Date/location of testing&procedure: May 19 Stanford
Type of venographic study: MRV, MRI Doppler
Diagnosis: Bilateral jugular occlusion 80-90% with extensive collateral circulation.
Type of procedure: Stents 8x40mm left, 12x40 right
Procedure/drug related symptoms:
1. I have spinal accessory nerve damage from the right stent. It is expected to heal in 9 more months. This is painful and causes weakness in the right shoulder.
2. I also had a rectus sheath hematoma-a bleed into my stomach muscles from the surgery that kept bleeding because of the coumadin.
3. Blood clot in the left calf.
Number of relapses since first CCSVI intervention: None.
Impact on your MS symptoms: [10/09]My changes are mostly very subtle. I feel energetic and awake, can walk for much longer without the drop foot tripping me, and am awake all day. I can even do back to back days of activities where before I would have to have days off between. Rest rejuvenates me so that a few minutes of rest allows me to go again, for example at the mall. Heat bothers me less. I no longer feel unnaturally cold all the time; I can keep my body warm as others can.
I no longer take Baclofen or Requip at bedtime and have very few spasms at all at night, fewer than I used to have ON the drugs. Can now use a Bioness functional electrical stimulator to correct the drop foot as spasms are so greatly reduced. I sleep well and wake to void perhaps once a night. Epworth sleepiness scales are now 4-5 (normal)
EDSS as of 10/09: no change at this point 4 months out from surgery..This is expected due to 18 year history of MS with progressive course,
MSIS as of 10/09 85 (down from est. 106) Biggest changes are in spasms, anxiety confidence sleeping feeling unwell worrying. These were significant before 1's now.
FSS as of 10/09 4.5. My own doctor keeps this record so the difference is from actual medical records. Biggest difference is overall it is much less a factor in my life. I still get tired but I recover so I can still do things.
As a comment I do not feel "cured": I feel like a woman with MS, my hope is for no progression. I also have a longer regimens thread "Marie's Stents CCSVI"
Female
Age: 48
Diagnosis: 1991 Dx RRMS, May of '08 SPMS
Lesion locations: 4 Perventricular lesions left hemisphere seen on 1.5 MRI, right sided weakness. All spinal MRI's clear. No inflammation for years on MRI, no enhancement.
MS treatments: Copaxone, supplements, failed treatments: MTX x 1.5 yr, plaquenil x 4yr (I have RA too), LDNx2yr, ABX x 3+yr,
MS symptoms before stenosis intervention: Severe drop foot right (foot is totally incapable of function, can't even willingly move a toe; really limp) right sided hand weakness, writing is difficult. Cane dependent, Rollator for long distances (mall etc). No cognitive issues. Mild urinary retention and voiding 4-5 times at night. Flexor spasms at night requiring Baclofen and Requip for many years. A test of a Walkaide functional electrical stimulator failed due to spasms. Stiffness upon standing. Sleeping difficulties; wakefulness and chronic daytime fatigue with Epworth sleepiness scales ranging from 11-17 over the last 2 years on MD assessment sheets.
Number of relapses before intervention (if applicable): none.
EDSS before stenosis intervention: 6+ self assessed. I use the rollator for long distances which is "bilateral support" but I can walk with the cane for 100 yards so is that a 6 (unilateral support) or more?
MSIS (estimated 10/09) before procedure 106
FSS before procedure (from my own MD records) 6
STENOSIS PROCEDURE HISTORY
Date/location of testing&procedure: May 19 Stanford
Type of venographic study: MRV, MRI Doppler
Diagnosis: Bilateral jugular occlusion 80-90% with extensive collateral circulation.
Type of procedure: Stents 8x40mm left, 12x40 right
Procedure/drug related symptoms:
1. I have spinal accessory nerve damage from the right stent. It is expected to heal in 9 more months. This is painful and causes weakness in the right shoulder.
2. I also had a rectus sheath hematoma-a bleed into my stomach muscles from the surgery that kept bleeding because of the coumadin.
3. Blood clot in the left calf.
Number of relapses since first CCSVI intervention: None.
Impact on your MS symptoms: [10/09]My changes are mostly very subtle. I feel energetic and awake, can walk for much longer without the drop foot tripping me, and am awake all day. I can even do back to back days of activities where before I would have to have days off between. Rest rejuvenates me so that a few minutes of rest allows me to go again, for example at the mall. Heat bothers me less. I no longer feel unnaturally cold all the time; I can keep my body warm as others can.
I no longer take Baclofen or Requip at bedtime and have very few spasms at all at night, fewer than I used to have ON the drugs. Can now use a Bioness functional electrical stimulator to correct the drop foot as spasms are so greatly reduced. I sleep well and wake to void perhaps once a night. Epworth sleepiness scales are now 4-5 (normal)
EDSS as of 10/09: no change at this point 4 months out from surgery..This is expected due to 18 year history of MS with progressive course,
MSIS as of 10/09 85 (down from est. 106) Biggest changes are in spasms, anxiety confidence sleeping feeling unwell worrying. These were significant before 1's now.
FSS as of 10/09 4.5. My own doctor keeps this record so the difference is from actual medical records. Biggest difference is overall it is much less a factor in my life. I still get tired but I recover so I can still do things.
As a comment I do not feel "cured": I feel like a woman with MS, my hope is for no progression. I also have a longer regimens thread "Marie's Stents CCSVI"
Last edited by mrhodes40 on Fri Dec 18, 2009 7:18 pm, edited 3 times in total.
I'm not offering medical advice, I am just a patient too! Talk to your doctor about what is best for you...
http://www.thisisms.com/ftopic-7318-0.html This is my regimen thread
http://www.ccsvibook.com Read my book published by McFarland Health topics
http://www.thisisms.com/ftopic-7318-0.html This is my regimen thread
http://www.ccsvibook.com Read my book published by McFarland Health topics
- cheerleader
- Family Elder
- Posts: 5361
- Joined: Mon Sep 10, 2007 2:00 pm
- Location: southern California
MS HISTORY
Jeff
M
46
RRMS diagnosed 3/07 (age 43) after first serious exacerbation
20 small, round lesions (Steiner's splashes) most in corpus callosum. One spinal lesion at C-3.
Program: Copaxone, endothelial health program (exercise, Swank diet, many antioxidant and vasodilating supplements)
MS symptoms: Fatigue, depression, emotional lability, heat intolerance, urgent bladder, leg pain, spasms, disturbed sleep, sleep apnea
Jeff has no peripheral vision. Diagnosed with bilateral drusen as a child. Depression and fatigue had also been around for 15 years prior to diagnosis.
Only one relapse, at time of diagnosis
Fatigue Severity Scale 6.5 (fatigue was hugely disabling)
1.5 EDSS
Had procedure to relieve stenosis at Stanford May 12, 2009
STENOSIS PROCEDURE HISTORY
MRV and doppler completed at Stanford University
Diagnosis: dual jugular stenosis, left closed 95% with many small collateral veins, right closed 80%
Blockage was very high, between C2-C4
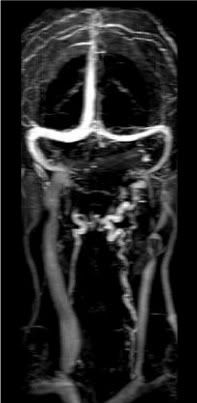
Type of procedure: two telescoping, self-expanding stents on left side, one on right side
Procedure/drug related symptoms: Severe nausea during procedure, head and neck pain after, relieved with extra strength tylenol. Shoulder pain and spasms from accessory nerve pinching, relieved with hot towel and pain relievers, gone after 9 weeks.
Second procedure done at Stanford, July 21, 2009
Ballooning of left stent to remove thickening of the endothelial lining at the bottom of the stent. Did much better, no nausea, no pain. Did not take any medications during this procedure. Slight headache after relieved with tylenol.
Third procedure at Stanford November 23, 2009
Ballooning of left stent and attempt to open up above in the very high left jug. No additional stent. No nausea or pain, but Jeff has a faint whoosh in his left ear when lying down at night, and has had daily headaches which seem to be postural, relieved if he lies down for a bit or takes tylenol. Energy is still great, fatigue is remitted. No relapses or progression.
Impact on MS symptoms. Immediate and profound affect on fatigue. No longer has that sense of "I can't keep my eyes open one more minute." Clearer perception, better mood. Much better heat tolerance, able to exercise in heat with no fatigue. Vastly improved sleep. No more sleep apnea or jarring spasms. Now sleeps deeply and is dreaming again. Smooth regular breathing, wakes up refreshed and ready for new day. Gets up once a night at most to void...much improved bladder.
Still has occasional leg pain and spasms.
End of March- coming up on year exam at Stanford in April- Jeff continues to have energy and enthusiasm. He is social, out-going and energetic. He still has slight whooshing in his left ear at night (where he now has jugular return-left side needed 2 stents), uses an air-filter fan to mask noise. Still has postural headaches, not as severe or every day anymore. No relapses or progression. Spasms gone at night, breathing is smooth, deep and even. Bladder is much better (many more nights without getting up at all) No more problems with heat or altitude. Looking forward to one year post stents MRI. Will post more after that.
1 EDSS
Fatigue Severity Scale 3
One year checkup - May 12, 2010-- no new lesions, no enhancing lesions, no MS progression. We will compare new MRI with old one at his neuro's office to see if there has been lesion healing/remyelination.
No more sleep apnea, much better bladder, no more myclonic jerks/spasms, no more heat intolerance, no more cog fog, much better fatigue. Still has occasional neuropathic leg pain. Still has postural headaches and the left ear whoosh, and still has a narrow sinus up above the left jugular, which Dr. Dake is not able to address at this time. Dr. Dake recommends getting rid of caffeine to see if there is any change in headaches/whoosh. We'll report back if that is effective/ineffective.
1 EDSS
Fatigue Severity Scale 3
Jeff
M
46
RRMS diagnosed 3/07 (age 43) after first serious exacerbation
20 small, round lesions (Steiner's splashes) most in corpus callosum. One spinal lesion at C-3.
Program: Copaxone, endothelial health program (exercise, Swank diet, many antioxidant and vasodilating supplements)
MS symptoms: Fatigue, depression, emotional lability, heat intolerance, urgent bladder, leg pain, spasms, disturbed sleep, sleep apnea
Jeff has no peripheral vision. Diagnosed with bilateral drusen as a child. Depression and fatigue had also been around for 15 years prior to diagnosis.
Only one relapse, at time of diagnosis
Fatigue Severity Scale 6.5 (fatigue was hugely disabling)
1.5 EDSS
Had procedure to relieve stenosis at Stanford May 12, 2009
STENOSIS PROCEDURE HISTORY
MRV and doppler completed at Stanford University
Diagnosis: dual jugular stenosis, left closed 95% with many small collateral veins, right closed 80%
Blockage was very high, between C2-C4

Type of procedure: two telescoping, self-expanding stents on left side, one on right side
Procedure/drug related symptoms: Severe nausea during procedure, head and neck pain after, relieved with extra strength tylenol. Shoulder pain and spasms from accessory nerve pinching, relieved with hot towel and pain relievers, gone after 9 weeks.
Second procedure done at Stanford, July 21, 2009
Ballooning of left stent to remove thickening of the endothelial lining at the bottom of the stent. Did much better, no nausea, no pain. Did not take any medications during this procedure. Slight headache after relieved with tylenol.
Third procedure at Stanford November 23, 2009
Ballooning of left stent and attempt to open up above in the very high left jug. No additional stent. No nausea or pain, but Jeff has a faint whoosh in his left ear when lying down at night, and has had daily headaches which seem to be postural, relieved if he lies down for a bit or takes tylenol. Energy is still great, fatigue is remitted. No relapses or progression.
Impact on MS symptoms. Immediate and profound affect on fatigue. No longer has that sense of "I can't keep my eyes open one more minute." Clearer perception, better mood. Much better heat tolerance, able to exercise in heat with no fatigue. Vastly improved sleep. No more sleep apnea or jarring spasms. Now sleeps deeply and is dreaming again. Smooth regular breathing, wakes up refreshed and ready for new day. Gets up once a night at most to void...much improved bladder.
Still has occasional leg pain and spasms.
End of March- coming up on year exam at Stanford in April- Jeff continues to have energy and enthusiasm. He is social, out-going and energetic. He still has slight whooshing in his left ear at night (where he now has jugular return-left side needed 2 stents), uses an air-filter fan to mask noise. Still has postural headaches, not as severe or every day anymore. No relapses or progression. Spasms gone at night, breathing is smooth, deep and even. Bladder is much better (many more nights without getting up at all) No more problems with heat or altitude. Looking forward to one year post stents MRI. Will post more after that.
1 EDSS
Fatigue Severity Scale 3
One year checkup - May 12, 2010-- no new lesions, no enhancing lesions, no MS progression. We will compare new MRI with old one at his neuro's office to see if there has been lesion healing/remyelination.
No more sleep apnea, much better bladder, no more myclonic jerks/spasms, no more heat intolerance, no more cog fog, much better fatigue. Still has occasional neuropathic leg pain. Still has postural headaches and the left ear whoosh, and still has a narrow sinus up above the left jugular, which Dr. Dake is not able to address at this time. Dr. Dake recommends getting rid of caffeine to see if there is any change in headaches/whoosh. We'll report back if that is effective/ineffective.
1 EDSS
Fatigue Severity Scale 3
Last edited by cheerleader on Wed May 12, 2010 3:16 pm, edited 5 times in total.
Husband dx RRMS 3/07
dx dual jugular vein stenosis (CCSVI) 4/09
http://ccsviinms.blogspot.com
dx dual jugular vein stenosis (CCSVI) 4/09
http://ccsviinms.blogspot.com
- Sport
- Family Member
- Posts: 40
- Joined: Sun Jul 05, 2009 2:00 pm
- Location: Midwest, USA
- Contact:
Patient Name: Sport
MS History
Male
Age: 43
Diagnosed 2005 PPMS
Lesion locations : T9 posterior to the spinal cord, midline and to the left. Probable lesion in the dorsal cord at C2-3. In the brain, a few periventricular lesions in the left side of the pons. One of these is hypointense on T1 weighted imaging (aka a black hole). All lesions show normal enhancement.
MS treatments: Mitoxantrone (3 courses, 2006), Rituxan (4 courses, 2006 - 2008), Copaxone (5/09 - current)
MS symptoms before stenosis intervention: bilateral leg/flexor weakness, foot drop, little cognitive impairment, significant imbalance when ambulating, moderate/severe leg spasticity.
EDSS before stenosis intervention 6-6.5
Stenosis Procedure History
Sept 24, 2009 - Stanford Hospital
MRV/MRI - Ultrasound
Diagnosis: Left IJV markedly narrowed over a 5cm segment from the jugular bulb centrally. In addition, a tight narrowing of IJV at the level of the valve above the clavicle. In the right IJV, a high-grade flattening was noted at the level of C1-C2.
Procedure: Stenting of the left IJ vein with a 8 x 60 mm self-expanding stent and 2nd stent, 14 x 30 mm at the level of the valve. The right IJV was treated with 9 x 40 mm self-expanding stent at the C1-C2 level. No stenosis noted in the azygos vein.
Procedure/drug related symptoms: Moderate problems with muscle pain in neck (levator muscle) and right shoulder; muscle weakness in right arm.
Number of relapses prior to CCSVI intervention: -0-
Number of relapses since CCSVI intervention: -0-
Impact on MS symptoms: less spasticity in both legs. Slight bilateral increase in leg strength and stamina noted when riding recumbent bike.
EDSS 10/5/2009 - 6 - 6.5.
Update 1/2/2010 - Are you using Inclined Bed Therapy I.B.T? (Y/N) - No
Update 11/11/2010 - One year follow up on 9/27/2010. All stents patent. Blood flowing through jugulars normally (or in medical speak, jugular blood flow is "unremarkable"). No change in brain lesion load. No significant MS symptomatic changes since the procedure for better or worse other than complete improvement in procedural related symptoms. Ambulation and walking stamina have probably continued to decline slowly. EDSS 6.5.
MS History
Male
Age: 43
Diagnosed 2005 PPMS
Lesion locations : T9 posterior to the spinal cord, midline and to the left. Probable lesion in the dorsal cord at C2-3. In the brain, a few periventricular lesions in the left side of the pons. One of these is hypointense on T1 weighted imaging (aka a black hole). All lesions show normal enhancement.
MS treatments: Mitoxantrone (3 courses, 2006), Rituxan (4 courses, 2006 - 2008), Copaxone (5/09 - current)
MS symptoms before stenosis intervention: bilateral leg/flexor weakness, foot drop, little cognitive impairment, significant imbalance when ambulating, moderate/severe leg spasticity.
EDSS before stenosis intervention 6-6.5
Stenosis Procedure History
Sept 24, 2009 - Stanford Hospital
MRV/MRI - Ultrasound
Diagnosis: Left IJV markedly narrowed over a 5cm segment from the jugular bulb centrally. In addition, a tight narrowing of IJV at the level of the valve above the clavicle. In the right IJV, a high-grade flattening was noted at the level of C1-C2.
Procedure: Stenting of the left IJ vein with a 8 x 60 mm self-expanding stent and 2nd stent, 14 x 30 mm at the level of the valve. The right IJV was treated with 9 x 40 mm self-expanding stent at the C1-C2 level. No stenosis noted in the azygos vein.
Procedure/drug related symptoms: Moderate problems with muscle pain in neck (levator muscle) and right shoulder; muscle weakness in right arm.
Number of relapses prior to CCSVI intervention: -0-
Number of relapses since CCSVI intervention: -0-
Impact on MS symptoms: less spasticity in both legs. Slight bilateral increase in leg strength and stamina noted when riding recumbent bike.
EDSS 10/5/2009 - 6 - 6.5.
Update 1/2/2010 - Are you using Inclined Bed Therapy I.B.T? (Y/N) - No
Update 11/11/2010 - One year follow up on 9/27/2010. All stents patent. Blood flowing through jugulars normally (or in medical speak, jugular blood flow is "unremarkable"). No change in brain lesion load. No significant MS symptomatic changes since the procedure for better or worse other than complete improvement in procedural related symptoms. Ambulation and walking stamina have probably continued to decline slowly. EDSS 6.5.
Last edited by Sport on Thu Nov 11, 2010 9:00 am, edited 2 times in total.
- Arcee
- Family Elder
- Posts: 338
- Joined: Wed Jan 05, 2005 3:00 pm
- Location: Massachusetts, USA
- Contact:
MS HISTORY
Name: Randi
Male/Female: F
Age: 41
Date(s) & type of neurological diagnosis (RRMS, SPMS, PPMS, CIS, or other): RRMS Spring 2004
Lesion locations (most affected side, if known), number:
Brain: Right Internal capsule. Bilateral periventricular white matter. Corona radiata and centrum semiovale. Right cerebellum. Ventral left medulla.
C-spine: most significant lesions are at C3/C4 levels
MS treatments: Betaseron for about a month until bad liver reaction. Copaxone, on and off, due to injection site reactions and current wait-and-see approach. Tysabri when first available, and then again when re-introduced, but allergic reaction stopped that treatment after 4 doses total.
MS symptoms before stenosis intervention: occasional tingling in my forearms and hands, a bit of fatigue or perhaps a lack of stamina, some heat sensitivity
Number of relapses before intervention (if applicable): 1 unbeknownst to me but showed on an MRI
EDSS before stenosis intervention :
0 - .5
Have you had a procedure for stenosis yet: Y
STENOSIS PROCEDURE HISTORY
Date/location of testing&procedure: 07/15/2009 Stanford University
Type of venographic study: MRV, Doppler
Diagnosis: tight narrowing at C2 that extends 3cm in left jugular vein; a 'functional occlusion'
Type of procedure: 7mm stent placed in left jugular vein
Procedure/drug related symptoms: Hardly any initial discomfort after procedure and none after a few days. Excessive bruising on aspirin/Coumadin/Plavix combo so discontinued Plavix
Number of relapses since first CCSVI intervention: 0
Impact on your MS symptoms in words :
While still at Stanford, feeling of going from digital cable to HD. Greater clarity visually and overall energized feeling. That sense of enhanced stamina remains. Heat intolerance has gone away.
EDSS as of this update: 0
Update: 4 mos. later and the stamina and HD-like perception remain. Have had occasional tingling in my forearms as I had pre-stenosis, but it is mild.
Update: 6 mos. and feeling great. Not even a twinge of tingling (the longest lapse since diagnosis). Stamina is great. Used to have dizziness when I would stand up at times, but that does not occur (although I recognize that it may be because I am well hydrated).
Update: 12 mos. and feel great. No fatigue or problems with heat. Do have very rare and short-lived tingling, but unclear whether the issue is MS damage or a disc issue. The standing up dizziness thing happens once in a rare while and makes me hydrate better. MRV and MRI checked out just fine at 1st anniversary Stanford visit. Will have those tests on an annual basis.
Name: Randi
Male/Female: F
Age: 41
Date(s) & type of neurological diagnosis (RRMS, SPMS, PPMS, CIS, or other): RRMS Spring 2004
Lesion locations (most affected side, if known), number:
Brain: Right Internal capsule. Bilateral periventricular white matter. Corona radiata and centrum semiovale. Right cerebellum. Ventral left medulla.
C-spine: most significant lesions are at C3/C4 levels
MS treatments: Betaseron for about a month until bad liver reaction. Copaxone, on and off, due to injection site reactions and current wait-and-see approach. Tysabri when first available, and then again when re-introduced, but allergic reaction stopped that treatment after 4 doses total.
MS symptoms before stenosis intervention: occasional tingling in my forearms and hands, a bit of fatigue or perhaps a lack of stamina, some heat sensitivity
Number of relapses before intervention (if applicable): 1 unbeknownst to me but showed on an MRI
EDSS before stenosis intervention :
0 - .5
Have you had a procedure for stenosis yet: Y
STENOSIS PROCEDURE HISTORY
Date/location of testing&procedure: 07/15/2009 Stanford University
Type of venographic study: MRV, Doppler
Diagnosis: tight narrowing at C2 that extends 3cm in left jugular vein; a 'functional occlusion'
Type of procedure: 7mm stent placed in left jugular vein
Procedure/drug related symptoms: Hardly any initial discomfort after procedure and none after a few days. Excessive bruising on aspirin/Coumadin/Plavix combo so discontinued Plavix
Number of relapses since first CCSVI intervention: 0
Impact on your MS symptoms in words :
While still at Stanford, feeling of going from digital cable to HD. Greater clarity visually and overall energized feeling. That sense of enhanced stamina remains. Heat intolerance has gone away.
EDSS as of this update: 0
Update: 4 mos. later and the stamina and HD-like perception remain. Have had occasional tingling in my forearms as I had pre-stenosis, but it is mild.
Update: 6 mos. and feeling great. Not even a twinge of tingling (the longest lapse since diagnosis). Stamina is great. Used to have dizziness when I would stand up at times, but that does not occur (although I recognize that it may be because I am well hydrated).
Update: 12 mos. and feel great. No fatigue or problems with heat. Do have very rare and short-lived tingling, but unclear whether the issue is MS damage or a disc issue. The standing up dizziness thing happens once in a rare while and makes me hydrate better. MRV and MRI checked out just fine at 1st anniversary Stanford visit. Will have those tests on an annual basis.
Last edited by Arcee on Sun Jul 18, 2010 8:47 am, edited 4 times in total.
diagnosed RR in spring '04
1 stent placed in left jugular vein 7/15/09
on and off Copaxone
allergric to interferons and Tysabri
1 stent placed in left jugular vein 7/15/09
on and off Copaxone
allergric to interferons and Tysabri
- gibbledygook
- Family Elder
- Posts: 1421
- Joined: Mon Feb 14, 2005 3:00 pm
- Location: London
- Contact:
Name: gibbledygook
Male/Female: Female
Age: 38
Date(s) & type of neurological diagnosis (RRMS, SPMS, PPMS, CIS, or other): 03/24/2004 RRMS
Lesion locations (most affected side, if known), number: brain and cervical spine
MS treatments: avonex, antibiotics, herbs, stents
MS symptoms before stenosis intervention: difficulty walking, bladder control, bowel control, swallowing difficulties, sensory deficits in leg and hands, torso and face, inability to sleep owing to spasms, movement induced phosphenes, depression
Number of relapses before intervention (if applicable): 6
EDSS before stenosis intervention (self-assessed or physician-assessed?): 6.5 by physician
Have you had a procedure for stenosis yet: Yes
STENOSIS PROCEDURE HISTORY
Date/location of testing&procedure: 06/23/20009 Stanford University Hospital
Type of venographic study: MRV
Diagnosis: bilateral jugular stenoses at C1 to C2
Type of procedure: 2 4cm stents placed in left and right jugular, extra 2cm stent placed in left jugular
Procedure/drug related symptoms: severe pain post-operation, initially all around head, left cheek and shoulders. Later, for 2.5 months severe pain in both shoulders
Number of relapses since first CCSVI intervention: 1 (see below for progress since pregnancy)
Impact on your MS symptoms:
Significant improvement in bladder control; less urgency, greater control, able to partially void using sphincter muscles
Significant improvement in night spasms; far weaker spasms, sometimes even absent spasms, spasms respond to stretching and am able to sleep before 1am most nights
Improvement in spasticity and walking. Recently walked the furthest I have walked since becoming ill in 2004. Less severe spasticity on standing and in the mornings.
Greater resilience to humid conditions
Sensory deficit affecting left leg much quieter
EDSS as of this update: 5 (self-assessment)
Since pregnancy my MS symptoms have deteriorated significantly and I thought it honest to update my symptoms as at 23 weeks of pregnancy and with alarmingly low blood pressure of 70 over 40. Below is as at 11/03/2010.
Number of relapses since first CCSVI intervention: 1 (see below for relapse info)
Impact on your MS symptoms:
Bladder improvements no longer evident but pregnancy a major issue
Night spasms have reverted to pre-operational strength and I am struggling to sleep with both legs going into strong spasms which do not respond to stretching.
Walking is much worse and I am back to about 300meters maximum with poor pick-up and spasticity is back to where it was before the operation.
The left leg sensory deficit has been more evident and in fact both feet are tingling much more heavily than in the non-pregnant months after the operation.
EDSS as of this update: 6.5 (self-assessment)
I am now at week 28 of pregnancy and I believe that I must have had in the last month or so a relapse as I developed a brand new symptom for a few days in my left hand and my left arm now seems weaker. I have been having a lot of pain in the area around the stents in the left jaw area and a cluster headache in the same place in the left side of the head for 6 weeks now. I have an ultrasound next week to check on blood flow.
Number of relapses since first CCSVI intervention: 1
Impact on your MS symptoms:
Night spasms are now the worst I have ever experienced.
Walking and spasticity are also very poor.
EDSS as of this update: 6.5 (self-assessment)
An ultrasound undertaken on 21 April 2010 revealed that the left stent has a new narrowing from 11mm to 3mm close to the transverse process at C1. However neither Professor Dake nor Dr Simka thought that this was relevant to my deterioration and do not recommend ballooning at this point. Dr Simka thinks I may have stenosis elsewhere in the venous outflow pathways since the vertebral veins were not examined at Stanford. Or he thinks the pregnancy has led to my deterioration. He mentioned that another of his patients who has become pregnant is also feeling worse.
Post-partum symptoms have improved significantly. update as at 18th August 2010.
Impact on your MS symptoms:
Bladder has reverted to post-stent level with ability to void using sphincter muscles and much much better control
Night spasms have significantly improved although are perhaps not as good as post stent. However they respond to stretching and I am able to sleep.
Walking is still worse than before the pregnancy and than after the stent operation but has improved a lot since the pregnancy.
The left leg sensory deficit is still rather evident.
I continue to have a left headache on the left side of the head which is worse on bending the neck in certain ways.
EDSS as of this update: 6.0 (self-assessment)
Number of relapses since first CCSVI intervention: 1
20/10/2010 update
I have returned from a Doppler scan in Poland by Dr Simka. Here is his report:
I take 500mg salvia miltiorrhiza every few days in addition to a daily 75mg aspirin just to ensure the blood is thin.
Male/Female: Female
Age: 38
Date(s) & type of neurological diagnosis (RRMS, SPMS, PPMS, CIS, or other): 03/24/2004 RRMS
Lesion locations (most affected side, if known), number: brain and cervical spine
MS treatments: avonex, antibiotics, herbs, stents
MS symptoms before stenosis intervention: difficulty walking, bladder control, bowel control, swallowing difficulties, sensory deficits in leg and hands, torso and face, inability to sleep owing to spasms, movement induced phosphenes, depression
Number of relapses before intervention (if applicable): 6
EDSS before stenosis intervention (self-assessed or physician-assessed?): 6.5 by physician
Have you had a procedure for stenosis yet: Yes
STENOSIS PROCEDURE HISTORY
Date/location of testing&procedure: 06/23/20009 Stanford University Hospital
Type of venographic study: MRV
Diagnosis: bilateral jugular stenoses at C1 to C2
Type of procedure: 2 4cm stents placed in left and right jugular, extra 2cm stent placed in left jugular
Procedure/drug related symptoms: severe pain post-operation, initially all around head, left cheek and shoulders. Later, for 2.5 months severe pain in both shoulders
Number of relapses since first CCSVI intervention: 1 (see below for progress since pregnancy)
Impact on your MS symptoms:
Significant improvement in bladder control; less urgency, greater control, able to partially void using sphincter muscles
Significant improvement in night spasms; far weaker spasms, sometimes even absent spasms, spasms respond to stretching and am able to sleep before 1am most nights
Improvement in spasticity and walking. Recently walked the furthest I have walked since becoming ill in 2004. Less severe spasticity on standing and in the mornings.
Greater resilience to humid conditions
Sensory deficit affecting left leg much quieter
EDSS as of this update: 5 (self-assessment)
Since pregnancy my MS symptoms have deteriorated significantly and I thought it honest to update my symptoms as at 23 weeks of pregnancy and with alarmingly low blood pressure of 70 over 40. Below is as at 11/03/2010.
Number of relapses since first CCSVI intervention: 1 (see below for relapse info)
Impact on your MS symptoms:
Bladder improvements no longer evident but pregnancy a major issue
Night spasms have reverted to pre-operational strength and I am struggling to sleep with both legs going into strong spasms which do not respond to stretching.
Walking is much worse and I am back to about 300meters maximum with poor pick-up and spasticity is back to where it was before the operation.
The left leg sensory deficit has been more evident and in fact both feet are tingling much more heavily than in the non-pregnant months after the operation.
EDSS as of this update: 6.5 (self-assessment)
I am now at week 28 of pregnancy and I believe that I must have had in the last month or so a relapse as I developed a brand new symptom for a few days in my left hand and my left arm now seems weaker. I have been having a lot of pain in the area around the stents in the left jaw area and a cluster headache in the same place in the left side of the head for 6 weeks now. I have an ultrasound next week to check on blood flow.
Number of relapses since first CCSVI intervention: 1
Impact on your MS symptoms:
Night spasms are now the worst I have ever experienced.
Walking and spasticity are also very poor.
EDSS as of this update: 6.5 (self-assessment)
An ultrasound undertaken on 21 April 2010 revealed that the left stent has a new narrowing from 11mm to 3mm close to the transverse process at C1. However neither Professor Dake nor Dr Simka thought that this was relevant to my deterioration and do not recommend ballooning at this point. Dr Simka thinks I may have stenosis elsewhere in the venous outflow pathways since the vertebral veins were not examined at Stanford. Or he thinks the pregnancy has led to my deterioration. He mentioned that another of his patients who has become pregnant is also feeling worse.
Post-partum symptoms have improved significantly. update as at 18th August 2010.
Impact on your MS symptoms:
Bladder has reverted to post-stent level with ability to void using sphincter muscles and much much better control
Night spasms have significantly improved although are perhaps not as good as post stent. However they respond to stretching and I am able to sleep.
Walking is still worse than before the pregnancy and than after the stent operation but has improved a lot since the pregnancy.
The left leg sensory deficit is still rather evident.
I continue to have a left headache on the left side of the head which is worse on bending the neck in certain ways.
EDSS as of this update: 6.0 (self-assessment)
Number of relapses since first CCSVI intervention: 1
20/10/2010 update
I have returned from a Doppler scan in Poland by Dr Simka. Here is his report:
My walking has improved considerably and the myoclonus whilst not as good as in the first few months after the stent operation is much better than during the pregnancy. I estimate my EDSS to be 5.5. The bladder is also considerably improved. Dr Simka said that the flow in the right jugular was mainly impaired when my head was tilted to the right so I shall try to ensure my head doesn't tilt to the right by pillow arrangment.Right internal jugular vein - stent is patent, no signs of thrombosis, intimal hyperplasia, pathological valve in the junction with brachiocephalic vein, with slight reflux in the area of the valve.
Left internal jugular vein - normal flow, stent is patent, no sign of thrombosis and intimal hyperplasia.
I take 500mg salvia miltiorrhiza every few days in addition to a daily 75mg aspirin just to ensure the blood is thin.
Last edited by gibbledygook on Thu Oct 21, 2010 4:00 am, edited 11 times in total.
3 years antibiotics, 06/09 bilateral jug stents at C1, 05/11 ballooning of both jug valves, 07/12 stenting of renal vein, azygos & jug valve ballooning,
- Jamie
- Family Elder
- Posts: 596
- Joined: Mon Jan 07, 2008 3:00 pm
- Contact:
MS HISTORY
Melissa
F
33
RRMS diagnosed 8/07 (age 31) after first serious exacerbation
8 lesions, 2x black holes, including lesion on brain stem.
Program: Rebif, High Dose Chemotherapy (HiCy/Revimmune), Copaxone.
MS symptoms: Fatigue, depression, emotional lability, heat intolerance, left side weakness, clonus, disturbed sleep, no dreams.
Depression had also been around for 15 years prior to diagnosis. Heavy bout of constipation, double vision and severe depression immediately prior to diagnosis.
5+ severe relapses (bedridden for several days) pre-HiCy. 2x clinical but not supported by MRI relapses post HiCy and pre-stents. Dr.Kerr at Hopkins agreed that Mel was indeed relapsing despite the absence of MRI activity. Mel was losing left side ability (particularly leg) at the time of intervention.
1.5 EDSS
Had procedure to relieve stenosis at Stanford July 7th 2009.
STENOSIS PROCEDURE HISTORY
MRV and doppler completed at Stanford University
Diagnosis: Dr. Dake discovered 3x jugular veins in Melissa, the left side veins were twisted around each other in such a way as it was impossible to tell which was 'real' and which was collateral.
Her left jug is congenitally 'weird', twisted with poor flow and a very small sinus.
He fixed one stenosis there and would have liked to open up the sinus with a stent but considered it too risky.
Her right jug is very dominant and normal flow has been restored with a large stent and all the collatoral veins have disappeared.
Type of procedure: Fitted one 12mm stent in right jug and one 7mm stent in left. No azygous occlusion. The stents were on the jawline.
Procedure/drug related symptoms: Neck pain for 5-7 days post surgery. for 3 days after surgery Mel ground her teeth in her sleep (loud enough to wake me up!), other than that - no issues.
Zero relapses since procedure.
Impact on MS symptoms: Immediate and profound affect on fatigue, weakness, heat tolerance etc etc. Mel has so far had a complete clinical response to intervention. Mel has stopped her prozac and no longer needs any psychotherapy and her bowel control is now normal. Restarted a running regime (treadmill), long term goal to get back to full fitness. Prescription for eyeglasses changed to a weaker lens as vision has improved dramatically. Milking the cliche here but she too went from Cable to HD almost immediately and has remained there since.
EDSS 0.5 (Doctor assessed, essentially very few remnants of her MS symptoms apart from muscle/nerve damage to left eye means it doesn't track properly when tested by doctor but no longer interferes with Mel's vision.)
Melissa
F
33
RRMS diagnosed 8/07 (age 31) after first serious exacerbation
8 lesions, 2x black holes, including lesion on brain stem.
Program: Rebif, High Dose Chemotherapy (HiCy/Revimmune), Copaxone.
MS symptoms: Fatigue, depression, emotional lability, heat intolerance, left side weakness, clonus, disturbed sleep, no dreams.
Depression had also been around for 15 years prior to diagnosis. Heavy bout of constipation, double vision and severe depression immediately prior to diagnosis.
5+ severe relapses (bedridden for several days) pre-HiCy. 2x clinical but not supported by MRI relapses post HiCy and pre-stents. Dr.Kerr at Hopkins agreed that Mel was indeed relapsing despite the absence of MRI activity. Mel was losing left side ability (particularly leg) at the time of intervention.
1.5 EDSS
Had procedure to relieve stenosis at Stanford July 7th 2009.
STENOSIS PROCEDURE HISTORY
MRV and doppler completed at Stanford University
Diagnosis: Dr. Dake discovered 3x jugular veins in Melissa, the left side veins were twisted around each other in such a way as it was impossible to tell which was 'real' and which was collateral.
Her left jug is congenitally 'weird', twisted with poor flow and a very small sinus.
He fixed one stenosis there and would have liked to open up the sinus with a stent but considered it too risky.
Her right jug is very dominant and normal flow has been restored with a large stent and all the collatoral veins have disappeared.
Type of procedure: Fitted one 12mm stent in right jug and one 7mm stent in left. No azygous occlusion. The stents were on the jawline.
Procedure/drug related symptoms: Neck pain for 5-7 days post surgery. for 3 days after surgery Mel ground her teeth in her sleep (loud enough to wake me up!), other than that - no issues.
Zero relapses since procedure.
Impact on MS symptoms: Immediate and profound affect on fatigue, weakness, heat tolerance etc etc. Mel has so far had a complete clinical response to intervention. Mel has stopped her prozac and no longer needs any psychotherapy and her bowel control is now normal. Restarted a running regime (treadmill), long term goal to get back to full fitness. Prescription for eyeglasses changed to a weaker lens as vision has improved dramatically. Milking the cliche here but she too went from Cable to HD almost immediately and has remained there since.
EDSS 0.5 (Doctor assessed, essentially very few remnants of her MS symptoms apart from muscle/nerve damage to left eye means it doesn't track properly when tested by doctor but no longer interferes with Mel's vision.)
- SammyJo
- Family Elder
- Posts: 225
- Joined: Wed Mar 10, 2004 3:00 pm
- Contact:
- Quest56
- Family Elder
- Posts: 323
- Joined: Mon May 22, 2006 2:00 pm
- Location: Northern Calif Monterey Bay Area
- Contact:
Tracy (Questor)
Male
Age: 53
MS History:
1981 CIS (first episode of optic neuritis)
1987 Diagnosed RRMS (private neurologist)
2000 Diagnosed SPMS (UCSF MS Center)
Lesion locations:
Extensive areas of T2 and FLAIR abnormality within the periventricular white matter including an approximate 8mm lesion adjacent to the left frontal horn. Rather prominent T2 hyperintense lesions within the middle cerebellar peduncles, more prominent on the left and within the pons and medulla. Some of the more prominent lesions demonstrate decreased signal intensity on T1 weighting.
MS treatments:
Betaseron 1993 through 1996.
Copaxone since 1998.
LDN (4.5mg) 9/2008 through 8/2009.
Exercise, Tai Chi, gluten- and dairy-free diet (BBD).
MS symptoms before stenosis intervention:
Gradually worsening problems over the years related to body fatigue, heat sensitivity, bladder and bowel problems, nausea, sexual impotence, migraines, lower body weakness, diminishing physical and mental stamina, nystagmus, poor left-eye vision and muscle control, gait instability, reduced sensation below the knees in both legs, lower leg spasticity (particularly at night), mental cloudiness, word slurring, and cognitive and short term memory weakness.
Number of relapses before intervention (if applicable):
Entire MS course has been relatively relapse free (except for the first few years in which relapses of optic neuritis, and episodes of double vision were not uncommon), disease course characterized instead by slow and steady progression,
EDSS before CCSVI intervention: 4 (UCSF MS Clinic 9/2008)
FSS before CCSVI intervention: 6.3
MSIS before CCSVI intervention: 70
Are you using Inclined Bed Therapy I.B.T? (Y/N) No
Have you had a procedure for stenosis yet: Yes
STENOSIS PROCEDURE HISTORY
Date/location of testing&procedure:
Stanford Hospital Medical Center
Test completed 9/15/2009
Stent procedure 9/16/2009
Type of venographic study: MRV, MRI, Doppler
Diagnosis:
Stenosis in left and right internal jugular veins, at a location approximately behind mid-ear, extending down to upper jaw
Type of procedure:
Absolute Pro 9.0 Stent (9mm diameter, 4cm long) inserted into left IJV, right side stent diameter slightly smaller (7mm or 8mm).
Procedure/drug related symptoms:
Neck and shoulder pain, a couple of very bad headaches (in the first week), nausea and weight loss (about 12 pounds). Pain meds discontinued after 2 weeks, still us Tylenol at night to sleep. After 4 weeks, I am still only able to sleep flat on my back, using a neck pillow, but pain is pretty much gone. Unusual neck and shoulder muscle tightness continues, with slow improvement. Right arm is still very weak in certain positions. I have started physical therapy and light exercise to speed recovery.
Link to Related Forum Topic: <<High Hopes in Santa Cruz>>
Number of relapses since first CCSVI intervention: 0
Impact on your MS symptoms in words:
[10/20/2009]
Significant reduction in nighttime spasticity in lower legs, and reduction in burning, tingling, numbness in legs/feet. Some reduction in heat sensitivity, but impossible to quantify. Increased dreaming activity. Moments of improved mental clarity and broadened mental scope (including memory access). Haven't needed to self-cath since procedure, but wake-up 5+ times at night to void. Continue with ear acupuncture treatment and kegel exercise to control bladder leakage.
[10/28/2009]
Am now able to bend my neck far enough to comfortably resume self-cathing at night before bed, which has reduced the number of nighttime trips to the bathroom to 2-3. Lower leg nighttime benefits continue (reduced spasticity and numbness), but degree of benefit still varies considerably from night to night. Because of the variability, it is impossible for me to say if the reduced spasticity benefit is due to the stent procedure, or if it is due to the changes in my routine since having the procedure (i.e., how I now sleep, reduced activity during the day, meds I am still on, etc). I have only needed to take ionic magnesium twice to quiet the spasticity since returning from Stanford. Before Stanford, I took magnesium nightly to help quiet the leg jerks so that I could sleep. My 2-month follow-up appointment is scheduled for 11/9/2009.
[12/10/2009]
Neck and shoulder difficulties continue, shoulder pain is felt when I am overly tired or forget to stretch/exercise (or exercise too much). Day-to-day variability of MS symptoms continues (lower body weakness, cog-fog, and night spasticity, in particular). I very rarely self-cath these days, once or twice a month instead of several times a week (I wake up at night approximately every two hours to void), my bladder seems to be emptying better, and my bowels seem much more regular than before the procedure (I used to go several days without a bowel movement, I now seem to be fairly regular in the morning without supplements or diet change, I continue BBD and acidophilus supplements with each meal).
[12/15/2009]
I have decided to discontinue taking LDN. I had stopped it temporarily on 8/31/2009 in preparation for surgery. I tried to restart LDN after I stopped taking blood thinners (first at 4.5mg, then 3.0mg) but stopped it again each time after only one night because of increased leg spasticity and bladder leakage, similar to what I had been experiencing over the last few years up to the point of surgery on 09/16/2009.
[01/13/2010]
Nighttime leg spasticity has been worsening over the last several days, last night was the most sleepless night I think I've ever had from this problem (pre- or post-procedure). Also, I have had to self-cath several times in the last week before bed, as I have had more trouble emptying my bladder lately.
[02/11/2010]
Minimal or no nighttime spasticity in lower-legs these last few weeks. This is still THE most remarkable symptomatic improvement I have felt since having the stent procedure. Also, I am often told by people who know me that my facial color is better than before the procedure, and that I show more walking stability and carry myself better. I seldom need to use a walking stick when I go out. Right shoulder is still bothersome, but improving slowly.
[09/08/2010]
One year summary posted in a separate thread, view it here:
One Year Stanford Treatment Exam
-- EDSS updates will be made 6-months to a year post-procedure
I won't be making these updates, as I think the self-assessed tests are too subjective to be useful.
EDSS as of this update (self-assessed or physician-assessed?)
FSS as of this update:
MSIS as of this update:
Male
Age: 53
MS History:
1981 CIS (first episode of optic neuritis)
1987 Diagnosed RRMS (private neurologist)
2000 Diagnosed SPMS (UCSF MS Center)
Lesion locations:
Extensive areas of T2 and FLAIR abnormality within the periventricular white matter including an approximate 8mm lesion adjacent to the left frontal horn. Rather prominent T2 hyperintense lesions within the middle cerebellar peduncles, more prominent on the left and within the pons and medulla. Some of the more prominent lesions demonstrate decreased signal intensity on T1 weighting.
MS treatments:
Betaseron 1993 through 1996.
Copaxone since 1998.
LDN (4.5mg) 9/2008 through 8/2009.
Exercise, Tai Chi, gluten- and dairy-free diet (BBD).
MS symptoms before stenosis intervention:
Gradually worsening problems over the years related to body fatigue, heat sensitivity, bladder and bowel problems, nausea, sexual impotence, migraines, lower body weakness, diminishing physical and mental stamina, nystagmus, poor left-eye vision and muscle control, gait instability, reduced sensation below the knees in both legs, lower leg spasticity (particularly at night), mental cloudiness, word slurring, and cognitive and short term memory weakness.
Number of relapses before intervention (if applicable):
Entire MS course has been relatively relapse free (except for the first few years in which relapses of optic neuritis, and episodes of double vision were not uncommon), disease course characterized instead by slow and steady progression,
EDSS before CCSVI intervention: 4 (UCSF MS Clinic 9/2008)
FSS before CCSVI intervention: 6.3
MSIS before CCSVI intervention: 70
Are you using Inclined Bed Therapy I.B.T? (Y/N) No
Have you had a procedure for stenosis yet: Yes
STENOSIS PROCEDURE HISTORY
Date/location of testing&procedure:
Stanford Hospital Medical Center
Test completed 9/15/2009
Stent procedure 9/16/2009
Type of venographic study: MRV, MRI, Doppler
Diagnosis:
Stenosis in left and right internal jugular veins, at a location approximately behind mid-ear, extending down to upper jaw
Type of procedure:
Absolute Pro 9.0 Stent (9mm diameter, 4cm long) inserted into left IJV, right side stent diameter slightly smaller (7mm or 8mm).
Procedure/drug related symptoms:
Neck and shoulder pain, a couple of very bad headaches (in the first week), nausea and weight loss (about 12 pounds). Pain meds discontinued after 2 weeks, still us Tylenol at night to sleep. After 4 weeks, I am still only able to sleep flat on my back, using a neck pillow, but pain is pretty much gone. Unusual neck and shoulder muscle tightness continues, with slow improvement. Right arm is still very weak in certain positions. I have started physical therapy and light exercise to speed recovery.
Link to Related Forum Topic: <<High Hopes in Santa Cruz>>
Number of relapses since first CCSVI intervention: 0
Impact on your MS symptoms in words:
[10/20/2009]
Significant reduction in nighttime spasticity in lower legs, and reduction in burning, tingling, numbness in legs/feet. Some reduction in heat sensitivity, but impossible to quantify. Increased dreaming activity. Moments of improved mental clarity and broadened mental scope (including memory access). Haven't needed to self-cath since procedure, but wake-up 5+ times at night to void. Continue with ear acupuncture treatment and kegel exercise to control bladder leakage.
[10/28/2009]
Am now able to bend my neck far enough to comfortably resume self-cathing at night before bed, which has reduced the number of nighttime trips to the bathroom to 2-3. Lower leg nighttime benefits continue (reduced spasticity and numbness), but degree of benefit still varies considerably from night to night. Because of the variability, it is impossible for me to say if the reduced spasticity benefit is due to the stent procedure, or if it is due to the changes in my routine since having the procedure (i.e., how I now sleep, reduced activity during the day, meds I am still on, etc). I have only needed to take ionic magnesium twice to quiet the spasticity since returning from Stanford. Before Stanford, I took magnesium nightly to help quiet the leg jerks so that I could sleep. My 2-month follow-up appointment is scheduled for 11/9/2009.
[12/10/2009]
Neck and shoulder difficulties continue, shoulder pain is felt when I am overly tired or forget to stretch/exercise (or exercise too much). Day-to-day variability of MS symptoms continues (lower body weakness, cog-fog, and night spasticity, in particular). I very rarely self-cath these days, once or twice a month instead of several times a week (I wake up at night approximately every two hours to void), my bladder seems to be emptying better, and my bowels seem much more regular than before the procedure (I used to go several days without a bowel movement, I now seem to be fairly regular in the morning without supplements or diet change, I continue BBD and acidophilus supplements with each meal).
[12/15/2009]
I have decided to discontinue taking LDN. I had stopped it temporarily on 8/31/2009 in preparation for surgery. I tried to restart LDN after I stopped taking blood thinners (first at 4.5mg, then 3.0mg) but stopped it again each time after only one night because of increased leg spasticity and bladder leakage, similar to what I had been experiencing over the last few years up to the point of surgery on 09/16/2009.
[01/13/2010]
Nighttime leg spasticity has been worsening over the last several days, last night was the most sleepless night I think I've ever had from this problem (pre- or post-procedure). Also, I have had to self-cath several times in the last week before bed, as I have had more trouble emptying my bladder lately.
[02/11/2010]
Minimal or no nighttime spasticity in lower-legs these last few weeks. This is still THE most remarkable symptomatic improvement I have felt since having the stent procedure. Also, I am often told by people who know me that my facial color is better than before the procedure, and that I show more walking stability and carry myself better. I seldom need to use a walking stick when I go out. Right shoulder is still bothersome, but improving slowly.
[09/08/2010]
One year summary posted in a separate thread, view it here:
One Year Stanford Treatment Exam
-- EDSS updates will be made 6-months to a year post-procedure
I won't be making these updates, as I think the self-assessed tests are too subjective to be useful.
EDSS as of this update (self-assessed or physician-assessed?)
FSS as of this update:
MSIS as of this update:
Last edited by Quest56 on Wed Feb 08, 2012 12:52 pm, edited 46 times in total.
- skydog
- Family Elder
- Posts: 306
- Joined: Tue Feb 24, 2009 3:00 pm
- Location: North Oregon Coast
Mark (skydog)
M
52 yrs
PPMS
02 to 04 some periodic double vision and constant dull headache that would not respond to most over the counter medications.
04 to 05 same double vision, dull headache, occasional tremors in right hand and pins and needle feeling in left foot. Up to this point all Dr. visits were answered with go easy your just getting older and need to slow down a little.
05 to 07 I was thinking possible MS and was sent in for my first MRI by a Dr. I see too this day and trust will always listen to me!
Patient: Mark diagnosis: PPMS 5/07 ( at age 50 ) lesions: scattered foci of the T2 hyperintense signal within the pariventicular and subcorttical white matter with involvement of the corpus callosum and colossal skeptical margin. Mild T2 shine through involving largest lesion within left perivvenrticular white matter measuring 7 mm Symptoms: left drop foot, pins and needle feeling in left foot, left leg weak, severe headaches, double vision, loud noises and ringing in ears, urgent bladder and bowel issues, stiff neck, left hand numbness and weakness, not able to perspire, heat intolerance, eyes would twitch for days at a time, left side of face would tighten, left foot looked purple, head felt hot and feet and hands cold. EDSS: Physician assessed 5.5 Treatments: Candida cleanse, antibiotic ( lime disease protocol ), anti viral, Swank diet, chelating therapy 3 months, low dose naltraxone 3 months, reduced stress load from work, 85% raw food diet, eat home grown organic foods, Exercise daily. Despite all my lifestyle changes, treatments and diet changes I was still progressively getting worse.
Diagnosis at Stanford 6/29/09 MRV, MRI, Doppler, Ultrasound showed anomalies of both jugular veins very high up near the base of skull in upper sinus area, right side jugular had a major twist and short area of stenosis ( resembled a pigs tail ) left side sharper than normal bend high up. On 6/30/09 two 7mm diameter stents were placed high up in the right jugular.
Enjoyed a two week period directly following surgery of reduced symptoms. Certain issues that I had not even thought about had disappeared, and some still remained the same. Most noticeably my hearing had improved. No longer heard the sounds in my head of a busy welding shop, just a steady ring that would be expected of the years of exposure to loud diesel engines fishing and operating heavy equipment. Fatigued less, and heat tolerance was better. The 7 years of dull to severe headaches had vanished, and aside from an occasional twinge of pain near the stented area was pain free. I was able to lift my left leg a little higher, but the drop foot remained the same. The left hand still got numb and week but would recover quickly with a little rest. Still faced bladder control issues, but the urgency seemed less. I broke into a good sweat the second night of our trip home, just the arms and chest area but sweating for the first times in 3 yrs. My forehead would dampen, but only when nearly overheated and starting to fatigue. The scaly dry legs were starting to get oily and was hopefully the precursor to sweating there also.
Now after a noticeable downturn 4 weeks post surgery all former issues have returned plus a rather stiff sore neck. EDSS at present is 6.5 self assessed.
Procedure # 2 at Stanford. MRI/MRV Showed no significant change since the Sept. 1 follow up. The big picture is the view from the beginning until the last scans showed much of the same collateral's. This is what Dr. Dake made his decision on stenting both the jugulars in the area of stenosis. His thoughts were that somehow during the first testing I was unusually tanked up and had the blood flowing. My take is that my prior regime to be in the best possible shape for the procedure might have downplayed the significance of the stenosis observed in this area. Now in addition to the original two 7mm stents in the upper right jugular, I now have two new ones. Right side 12mm/30mm and left 10/30mm both in the mid neck region. So far my biggest improvements are that my head feels much clearer, resumed sweating on my arms, arm pits, and torso. Just currently night sweats as I can not get very physical yet. The downside has been my neck was quite painful for the first couple of days. Now the pain has subsided some there and moved into the shoulders and right arm. Will post any significant changes in the future. Its been four weeks since my last procedure and I am feeling great! First off I must say that I am thrilled to see so many new people here. The energy they bring is outstanding. Not only has the CCSVI received more attention but all other topics as well are gaining fresh insight from all that have joined us here. Thank you! For those that think they missed the CCSVI boat. Be patient the best is yet to come. I feel honored to have been in on the groundbreaking of CCSVI. To be quite honest it has not been as easy as it seems as you know from following my journey. Without the pioneers there is no way that future clinical trials could begin without huge pitfalls. Lets hope lessons learned will bring smooth sailing for those treated in the future. For now please stay as positive and healthy as you can be. So here is my update. Most all of the former symptoms have lessened to some degree. The thing I wish most for is the ability to beat the heavy left leg and drop foot issue. It would seem that there is no improvement there yet. Actually it seems a little worse. I guess that I was hoping for a repeat too my original point post first surgery. My feeling is that during the 16 plus weeks in which I was defiantly suffering from decreased drainage that more added brain iron is to blame. I finally got the INR up and beyond the therapeutic level. My last INR was 4.21 and PT 39 so I will be backing off a bit on the blood thinners. My diet definitely was effecting my ability to get within range the first time around. Too much green! and high vita K foods. I can hardly wait to get back to gardening next spring and my healthy green smoothies once off the blood thinners of coarse. All is well and couldn't feel better. My energy level is up so Brenda has had to keep me on the short leash. No appreciable pain just the occasional twinge in both the upper and lower stent areas. The right side has been virtually pain free now for two weeks. One thing I have noticed is that the twinges of pain seem to be accompanied with what feels like a muscle contraction around the stent area on the left side. I am sure this will pass in time. Now for the best news. My heat intolerance is definitely better, fatigue way less, bladder control somewhat better, headaches a thing of the past, head feels clear, ringing in the ears back to my norm. Just plain feels right this time around! The biggest limiting factor is muscle spasticity and drop foot. With PT I am recovering some mobility. Just going to take some time and honest effort. I have been sleeping well and feel quite refreshed in the mornings. Peace and Health to All, Mark
M
52 yrs
PPMS
02 to 04 some periodic double vision and constant dull headache that would not respond to most over the counter medications.
04 to 05 same double vision, dull headache, occasional tremors in right hand and pins and needle feeling in left foot. Up to this point all Dr. visits were answered with go easy your just getting older and need to slow down a little.
05 to 07 I was thinking possible MS and was sent in for my first MRI by a Dr. I see too this day and trust will always listen to me!
Patient: Mark diagnosis: PPMS 5/07 ( at age 50 ) lesions: scattered foci of the T2 hyperintense signal within the pariventicular and subcorttical white matter with involvement of the corpus callosum and colossal skeptical margin. Mild T2 shine through involving largest lesion within left perivvenrticular white matter measuring 7 mm Symptoms: left drop foot, pins and needle feeling in left foot, left leg weak, severe headaches, double vision, loud noises and ringing in ears, urgent bladder and bowel issues, stiff neck, left hand numbness and weakness, not able to perspire, heat intolerance, eyes would twitch for days at a time, left side of face would tighten, left foot looked purple, head felt hot and feet and hands cold. EDSS: Physician assessed 5.5 Treatments: Candida cleanse, antibiotic ( lime disease protocol ), anti viral, Swank diet, chelating therapy 3 months, low dose naltraxone 3 months, reduced stress load from work, 85% raw food diet, eat home grown organic foods, Exercise daily. Despite all my lifestyle changes, treatments and diet changes I was still progressively getting worse.
Diagnosis at Stanford 6/29/09 MRV, MRI, Doppler, Ultrasound showed anomalies of both jugular veins very high up near the base of skull in upper sinus area, right side jugular had a major twist and short area of stenosis ( resembled a pigs tail ) left side sharper than normal bend high up. On 6/30/09 two 7mm diameter stents were placed high up in the right jugular.
Enjoyed a two week period directly following surgery of reduced symptoms. Certain issues that I had not even thought about had disappeared, and some still remained the same. Most noticeably my hearing had improved. No longer heard the sounds in my head of a busy welding shop, just a steady ring that would be expected of the years of exposure to loud diesel engines fishing and operating heavy equipment. Fatigued less, and heat tolerance was better. The 7 years of dull to severe headaches had vanished, and aside from an occasional twinge of pain near the stented area was pain free. I was able to lift my left leg a little higher, but the drop foot remained the same. The left hand still got numb and week but would recover quickly with a little rest. Still faced bladder control issues, but the urgency seemed less. I broke into a good sweat the second night of our trip home, just the arms and chest area but sweating for the first times in 3 yrs. My forehead would dampen, but only when nearly overheated and starting to fatigue. The scaly dry legs were starting to get oily and was hopefully the precursor to sweating there also.
Now after a noticeable downturn 4 weeks post surgery all former issues have returned plus a rather stiff sore neck. EDSS at present is 6.5 self assessed.
Procedure # 2 at Stanford. MRI/MRV Showed no significant change since the Sept. 1 follow up. The big picture is the view from the beginning until the last scans showed much of the same collateral's. This is what Dr. Dake made his decision on stenting both the jugulars in the area of stenosis. His thoughts were that somehow during the first testing I was unusually tanked up and had the blood flowing. My take is that my prior regime to be in the best possible shape for the procedure might have downplayed the significance of the stenosis observed in this area. Now in addition to the original two 7mm stents in the upper right jugular, I now have two new ones. Right side 12mm/30mm and left 10/30mm both in the mid neck region. So far my biggest improvements are that my head feels much clearer, resumed sweating on my arms, arm pits, and torso. Just currently night sweats as I can not get very physical yet. The downside has been my neck was quite painful for the first couple of days. Now the pain has subsided some there and moved into the shoulders and right arm. Will post any significant changes in the future. Its been four weeks since my last procedure and I am feeling great! First off I must say that I am thrilled to see so many new people here. The energy they bring is outstanding. Not only has the CCSVI received more attention but all other topics as well are gaining fresh insight from all that have joined us here. Thank you! For those that think they missed the CCSVI boat. Be patient the best is yet to come. I feel honored to have been in on the groundbreaking of CCSVI. To be quite honest it has not been as easy as it seems as you know from following my journey. Without the pioneers there is no way that future clinical trials could begin without huge pitfalls. Lets hope lessons learned will bring smooth sailing for those treated in the future. For now please stay as positive and healthy as you can be. So here is my update. Most all of the former symptoms have lessened to some degree. The thing I wish most for is the ability to beat the heavy left leg and drop foot issue. It would seem that there is no improvement there yet. Actually it seems a little worse. I guess that I was hoping for a repeat too my original point post first surgery. My feeling is that during the 16 plus weeks in which I was defiantly suffering from decreased drainage that more added brain iron is to blame. I finally got the INR up and beyond the therapeutic level. My last INR was 4.21 and PT 39 so I will be backing off a bit on the blood thinners. My diet definitely was effecting my ability to get within range the first time around. Too much green! and high vita K foods. I can hardly wait to get back to gardening next spring and my healthy green smoothies once off the blood thinners of coarse. All is well and couldn't feel better. My energy level is up so Brenda has had to keep me on the short leash. No appreciable pain just the occasional twinge in both the upper and lower stent areas. The right side has been virtually pain free now for two weeks. One thing I have noticed is that the twinges of pain seem to be accompanied with what feels like a muscle contraction around the stent area on the left side. I am sure this will pass in time. Now for the best news. My heat intolerance is definitely better, fatigue way less, bladder control somewhat better, headaches a thing of the past, head feels clear, ringing in the ears back to my norm. Just plain feels right this time around! The biggest limiting factor is muscle spasticity and drop foot. With PT I am recovering some mobility. Just going to take some time and honest effort. I have been sleeping well and feel quite refreshed in the mornings. Peace and Health to All, Mark
Last edited by skydog on Wed Dec 16, 2009 11:15 am, edited 6 times in total.
- CNClear
- Family Member
- Posts: 96
- Joined: Fri Aug 28, 2009 2:00 pm
- Location: Near Atlanta, GA
- Contact:
MS HISTORY
Name: Lisa aka, CNClear
Male/Female: (F)
Age: 50
Date(s) & type of neurological diagnosis: RRMS dx 1983
Lesion locations (most affected side, if known), number:
MS treatments: Copaxone - 2 years, Avonex - 2 years
MS symptoms before stenosis intervention:
Number of relapses before intervention (if applicable):
EDSS before CCSVI intervention (self-assessed or physician-assessed?):
[To review EDSS rating, click the following link: http://www.mult-sclerosis.org/expandedd ... scale.html ]
FSS before CCSVI intervention: 6.5
MSIS before CCSVI intervention:
[To calculate MSIS rating , click the following link: http://healingpowernow.com/msis.htm ]
Have you had a procedure for stenosis yet: scheduled for Dec 8th & 9th, 2009 at Stanford with Dake
STENOSIS PROCEDURE HISTORY
Date/location of testing&procedure:
Type of venographic study: (MRV, Doppler)
Diagnosis:
Type of procedure:
Procedure/drug related symptoms:
[Repeat this section if there have been more than one procedure]
Number of relapses since first CCSVI intervention:
Impact on your MS symptoms in words (include date in brackets if there have been multiple updates):
EDSS as of this update (self-assessed or physician-assessed?)
FSS as of this update:
MSIS as of this update:
Name: Lisa aka, CNClear
Male/Female: (F)
Age: 50
Date(s) & type of neurological diagnosis: RRMS dx 1983
Lesion locations (most affected side, if known), number:
MS treatments: Copaxone - 2 years, Avonex - 2 years
MS symptoms before stenosis intervention:
Number of relapses before intervention (if applicable):
EDSS before CCSVI intervention (self-assessed or physician-assessed?):
[To review EDSS rating, click the following link: http://www.mult-sclerosis.org/expandedd ... scale.html ]
FSS before CCSVI intervention: 6.5
MSIS before CCSVI intervention:
[To calculate MSIS rating , click the following link: http://healingpowernow.com/msis.htm ]
Have you had a procedure for stenosis yet: scheduled for Dec 8th & 9th, 2009 at Stanford with Dake
STENOSIS PROCEDURE HISTORY
Date/location of testing&procedure:
Type of venographic study: (MRV, Doppler)
Diagnosis:
Type of procedure:
Procedure/drug related symptoms:
[Repeat this section if there have been more than one procedure]
Number of relapses since first CCSVI intervention:
Impact on your MS symptoms in words (include date in brackets if there have been multiple updates):
EDSS as of this update (self-assessed or physician-assessed?)
FSS as of this update:
MSIS as of this update:
- magoo
- Family Elder
- Posts: 574
- Joined: Thu Sep 10, 2009 2:00 pm
- Location: Charlotte, NC
- Contact:
Patient Name: Rhonda
MS history
Female
42
11/2003 RRMS
8 lesions total, some healed/disappeared from MRI : 6 mm flair abnormality in the right periventricular white matter with T2 white focus, right posterior frontal deep white matter lesion, Enhancing lesion right middle cerebellar peduncle, T2 hyper intensities at the right pontomedullary region and the right frontal region, Suspected spinal cord lesion, physical evidence only.
MS Treatments: Betaseron, Tysabri and Copaxone
MS symptoms before stenosis intervention: Migraines, right sided neck, back and shoulder pain, severe fatigue, numbness, balance issues, dizziness, stiffness, cognitive problems, anxiety, urinary urgency, weakness, MS hug, trembling, heat sensitivity
Relapses: 7-9
EDSS: 5.5
FSS: 5.5
MSIS:100
Stenosis Procedure History
10/19/2009 - Stanford, testing and procedure, Dr. Dake
MRI of the brain /MRV of the head and neck
Diagnosis: High grade narrowing of the upper jugular segments bilaterally at C1 and C2. Pressure gradients of 5 mmHg on left and right.
Procedure: 2 self expanding stents placed on each side, following stent placement pressure gradients were obliterated. The collateral pattern was no longer filling, and both veins were normal in caliber.
Procedure/Drug related symptoms: Extreme head pain during and after procedure. I had muscle twitching in neck and back for 3 days. Morphine and Percocet caused nausea and vomiting. Intense pain and nausea persisted for 4 days. At days 5+ nausea ceased and pain lessened to daily headaches. Headaches relieved by laying flat and not using neck muscles. Normal fatigue as expected from recovery. I have had some left shoulder muscle stiffness.
Number of relapses since CCSVI: 0
Do you use IBT? No
Impact on MS symptoms:One week after procedure:
Fatigue is noticeably better. I have an awake feeling all day. I do not feel the need to rest throughout the day.
Right sided pain is gone.
Stiffness in legs and arms is gone.
No urinary urgency.
No migraines.
Cognitive ability seems improved.
Heat sensitivity seems improved.
1 month after procedure:
MS type fatigue is gone. No need to rest throughout the day and stamina is good. Cognitive function is greatly improved. No more trouble finding words, having conversations or multi-tasking. Right-sided pain is still gone. No dizziness, balance problems, tremors, weakness, or trouble with anxiety since surgery.
I do have some minor stiffness in legs, but this could be the result of more activity. I still have daily headaches above my left eye which are connected to my left shoulder and nerve issues from surgery.
Update: Dec. 2, 2009
Continued improvements in all areas listed above. I certainly do not feel as fragile as I used to. I am doing 1000% more than I was able to do before the surgery. I have no fear planning things or having a day-long list of things to do!!!! The headaches above my left eye continue to be a problem. I did get a soft cervical neckbrace and have had complete relief when wearing it. I assume these will resolve in time as they have for most. I have minor stiffness in calves at night, but nothing that requires medicine. Next week I have my follow-up appt. with Dr. Dake.
Update Dec. 18, 2009:
I wanted to update since I was back at Stanford 12/8 for my follow-up appt. with Dr. Dake. The scans were great. The before and after images were astonishing. The veins were essentially flat, almost 100% closed before surgery. The veins are now wide open and the stents are nicely integrated. I have discontinued Coumadin, but will remain on Plavix for a time. Dr. Dake thinks it is just a good insurance policy. I will continue to take one aspirin daily for the rest of my life.
I feel great. The headaches are mostly gone. I have gone several days without ANY pain medications...I haven't been able to do this in 6 years! I feel pretty much normal. I feel like I did BEFORE MS came into my life. I know this is a huge statement, but it is honestly how I feel. I have no MS symptoms. I do not know if this will be the end of my story, but I am so happy to have my life back for however long
Feb. 18, 2010
I had a few problems this month, none had anything to do with MS/CCSVI. I had the H1N1 vaccine and had a worsening of some symptoms. Dr. Dake didn't know for sure, but had seen one other patient go through the same thing post H1N1. This connection is up for debate, but I believe they are related. Soon after this I found out I was suffering from iron deficient anemia. We are investigating the possible connection to the Plavix and aspirin regimen. I began taking iron supplements and have been on the upswing! I am happy to report my energy, clarity, sleep, and headaches have all improved. I am feeling strong and well, and I'm happy the problems I've had have been explained and are on their way to being remedied. My shoulder is 90% healed and my range of motion is almost back to normal. Dr. Dake said 4 months for healing, looks like he hit the mark!
5 Month Update
My life has taken a normal pace. The Anemia has been resolved. We did not find any evidence that the Plavix or Aspirin were causing it. I had such a feeling of recovery and energy with the iron supplements. I stopped taking them as soon as my numbers were back in the normal range. I now have been living life feeling like a person withOUT MS. I work-out, I've gone hiking, I've been stripping wallpaper and spring cleaning. I have as much energy as all of the other members of my family. I do have some evening stiffness in my neck, but I've had this most of my life. I experience some random aching in my legs at night sometimes, but it is not enough to worry about. I am looking forward to this summer. I have not been able to go to the pool or spend any amount of time in the heat for years. I haven't had any heat intolerance since surgery and I'm so happy not to be wilting in the sun!
7 Month Update
Well... it's 8 days until my 7 month point I am doing really well. I haven't had any of my old MS symptoms at all. Really, not one single bit! My strength and stamina are increasing all the time. I have done things I never thought I'd be able to do like mountain climbing, bike riding, and the most shocking of all...running! Running has always, as far as I can remember, been hard for me. As a kid I hated running because it never felt comfortable or easy. I never knew what people saw in it. (I wonder if it was CCSVI?) Now, I actually feel good and strong when running and I understand!! I just spent three days at the beach in 90 degree weather and had NO heat intolerance. We go every year on Mother's Day weekend and I always ended up back in the condo after a short time in the sun. I would be worn out, numb and in a lot of pain from sitting in the heat. This year I was able to spend the entire time with my kids and family and it was wonderful!!!! I have also been socializing a lot more. Friends I haven't seen in a long time have noticed how well I look and I have been sharing my CCSVI story with a lot of them. It is so amazing to feel like myself again and it's like a miracle to have gotten better. When you have MS you just keep adjusting to the lost stamina and abilities and now I don't have to do that. I wake with energy and tackle each day just like everyone else. I know not everyone has had such good results, and I know how lucky I am to have been treated early, so I will continue to work to move CCSVI forward.
I am doing really well. I haven't had any of my old MS symptoms at all. Really, not one single bit! My strength and stamina are increasing all the time. I have done things I never thought I'd be able to do like mountain climbing, bike riding, and the most shocking of all...running! Running has always, as far as I can remember, been hard for me. As a kid I hated running because it never felt comfortable or easy. I never knew what people saw in it. (I wonder if it was CCSVI?) Now, I actually feel good and strong when running and I understand!! I just spent three days at the beach in 90 degree weather and had NO heat intolerance. We go every year on Mother's Day weekend and I always ended up back in the condo after a short time in the sun. I would be worn out, numb and in a lot of pain from sitting in the heat. This year I was able to spend the entire time with my kids and family and it was wonderful!!!! I have also been socializing a lot more. Friends I haven't seen in a long time have noticed how well I look and I have been sharing my CCSVI story with a lot of them. It is so amazing to feel like myself again and it's like a miracle to have gotten better. When you have MS you just keep adjusting to the lost stamina and abilities and now I don't have to do that. I wake with energy and tackle each day just like everyone else. I know not everyone has had such good results, and I know how lucky I am to have been treated early, so I will continue to work to move CCSVI forward.
18 month update:
Problems with headaches/migraines returning along with right-sided pain. Heat intolerance seems to be returning. I had vertigo after a therapeutic injection in my facet joint. Recently, I had some numbness. Going for evaluation and treatment to check for additional blockages. I initially had only my jugular and azygos veins checked. Now, because so much has been discovered, I will have the renals, iliac, IVC, SVC, and brachiocephalic veins investigated along with the re-check of the jugulars and azygos. CCSVI will require repeated maintenance because restenosis is to be expected. I look forward to discovering what the next venogram will do for my health. I know treating CCSVI changed my disease in a dramatic way. I have had improvement. Nothing else has been able to do that.
3 weeks after 2nd treatment
I had additional problems with both jugular veins at the valves, a 70% blockage in my azygous caused by a tight web and a valve, a 70% blockage in my left renal vein, and an 80% blockage in my left iliac vein (May Thurners). All were treated with angioplasty. My stents are wide open and patent. I have had additional improvements, but I seem to be taking a while to heal. I still have headaches and some pain in my chest and back where my azygous is located. Overall, I am very happy with the improvements I have. I'm not perfect, but SO much better than before this amazing treatment.
2 months after second treatment
Headaches have completely disappeared, heat intolerance is gone and I feel great. I still have the new pain under my left shoulder blade, but all of the improvements I wanted have happened again. Also had an MRI of the brain which showed NO new activity!
MS history
Female
42
11/2003 RRMS
8 lesions total, some healed/disappeared from MRI : 6 mm flair abnormality in the right periventricular white matter with T2 white focus, right posterior frontal deep white matter lesion, Enhancing lesion right middle cerebellar peduncle, T2 hyper intensities at the right pontomedullary region and the right frontal region, Suspected spinal cord lesion, physical evidence only.
MS Treatments: Betaseron, Tysabri and Copaxone
MS symptoms before stenosis intervention: Migraines, right sided neck, back and shoulder pain, severe fatigue, numbness, balance issues, dizziness, stiffness, cognitive problems, anxiety, urinary urgency, weakness, MS hug, trembling, heat sensitivity
Relapses: 7-9
EDSS: 5.5
FSS: 5.5
MSIS:100
Stenosis Procedure History
10/19/2009 - Stanford, testing and procedure, Dr. Dake
MRI of the brain /MRV of the head and neck
Diagnosis: High grade narrowing of the upper jugular segments bilaterally at C1 and C2. Pressure gradients of 5 mmHg on left and right.
Procedure: 2 self expanding stents placed on each side, following stent placement pressure gradients were obliterated. The collateral pattern was no longer filling, and both veins were normal in caliber.
Procedure/Drug related symptoms: Extreme head pain during and after procedure. I had muscle twitching in neck and back for 3 days. Morphine and Percocet caused nausea and vomiting. Intense pain and nausea persisted for 4 days. At days 5+ nausea ceased and pain lessened to daily headaches. Headaches relieved by laying flat and not using neck muscles. Normal fatigue as expected from recovery. I have had some left shoulder muscle stiffness.
Number of relapses since CCSVI: 0
Do you use IBT? No
Impact on MS symptoms:One week after procedure:
Fatigue is noticeably better. I have an awake feeling all day. I do not feel the need to rest throughout the day.
Right sided pain is gone.
Stiffness in legs and arms is gone.
No urinary urgency.
No migraines.
Cognitive ability seems improved.
Heat sensitivity seems improved.
1 month after procedure:
MS type fatigue is gone. No need to rest throughout the day and stamina is good. Cognitive function is greatly improved. No more trouble finding words, having conversations or multi-tasking. Right-sided pain is still gone. No dizziness, balance problems, tremors, weakness, or trouble with anxiety since surgery.
I do have some minor stiffness in legs, but this could be the result of more activity. I still have daily headaches above my left eye which are connected to my left shoulder and nerve issues from surgery.
Update: Dec. 2, 2009
Continued improvements in all areas listed above. I certainly do not feel as fragile as I used to. I am doing 1000% more than I was able to do before the surgery. I have no fear planning things or having a day-long list of things to do!!!! The headaches above my left eye continue to be a problem. I did get a soft cervical neckbrace and have had complete relief when wearing it. I assume these will resolve in time as they have for most. I have minor stiffness in calves at night, but nothing that requires medicine. Next week I have my follow-up appt. with Dr. Dake.
Update Dec. 18, 2009:
I wanted to update since I was back at Stanford 12/8 for my follow-up appt. with Dr. Dake. The scans were great. The before and after images were astonishing. The veins were essentially flat, almost 100% closed before surgery. The veins are now wide open and the stents are nicely integrated. I have discontinued Coumadin, but will remain on Plavix for a time. Dr. Dake thinks it is just a good insurance policy. I will continue to take one aspirin daily for the rest of my life.
I feel great. The headaches are mostly gone. I have gone several days without ANY pain medications...I haven't been able to do this in 6 years! I feel pretty much normal. I feel like I did BEFORE MS came into my life. I know this is a huge statement, but it is honestly how I feel. I have no MS symptoms. I do not know if this will be the end of my story, but I am so happy to have my life back for however long
Feb. 18, 2010
I had a few problems this month, none had anything to do with MS/CCSVI. I had the H1N1 vaccine and had a worsening of some symptoms. Dr. Dake didn't know for sure, but had seen one other patient go through the same thing post H1N1. This connection is up for debate, but I believe they are related. Soon after this I found out I was suffering from iron deficient anemia. We are investigating the possible connection to the Plavix and aspirin regimen. I began taking iron supplements and have been on the upswing! I am happy to report my energy, clarity, sleep, and headaches have all improved. I am feeling strong and well, and I'm happy the problems I've had have been explained and are on their way to being remedied. My shoulder is 90% healed and my range of motion is almost back to normal. Dr. Dake said 4 months for healing, looks like he hit the mark!
5 Month Update
My life has taken a normal pace. The Anemia has been resolved. We did not find any evidence that the Plavix or Aspirin were causing it. I had such a feeling of recovery and energy with the iron supplements. I stopped taking them as soon as my numbers were back in the normal range. I now have been living life feeling like a person withOUT MS. I work-out, I've gone hiking, I've been stripping wallpaper and spring cleaning. I have as much energy as all of the other members of my family. I do have some evening stiffness in my neck, but I've had this most of my life. I experience some random aching in my legs at night sometimes, but it is not enough to worry about. I am looking forward to this summer. I have not been able to go to the pool or spend any amount of time in the heat for years. I haven't had any heat intolerance since surgery and I'm so happy not to be wilting in the sun!
7 Month Update
Well... it's 8 days until my 7 month point
18 month update:
Problems with headaches/migraines returning along with right-sided pain. Heat intolerance seems to be returning. I had vertigo after a therapeutic injection in my facet joint. Recently, I had some numbness. Going for evaluation and treatment to check for additional blockages. I initially had only my jugular and azygos veins checked. Now, because so much has been discovered, I will have the renals, iliac, IVC, SVC, and brachiocephalic veins investigated along with the re-check of the jugulars and azygos. CCSVI will require repeated maintenance because restenosis is to be expected. I look forward to discovering what the next venogram will do for my health. I know treating CCSVI changed my disease in a dramatic way. I have had improvement. Nothing else has been able to do that.
3 weeks after 2nd treatment
I had additional problems with both jugular veins at the valves, a 70% blockage in my azygous caused by a tight web and a valve, a 70% blockage in my left renal vein, and an 80% blockage in my left iliac vein (May Thurners). All were treated with angioplasty. My stents are wide open and patent. I have had additional improvements, but I seem to be taking a while to heal. I still have headaches and some pain in my chest and back where my azygous is located. Overall, I am very happy with the improvements I have. I'm not perfect, but SO much better than before this amazing treatment.
2 months after second treatment
Headaches have completely disappeared, heat intolerance is gone and I feel great. I still have the new pain under my left shoulder blade, but all of the improvements I wanted have happened again. Also had an MRI of the brain which showed NO new activity!
Last edited by magoo on Thu Jul 07, 2011 3:40 pm, edited 15 times in total.
Rhonda~
Treated by Dake 10/19/09, McGuckin 4/25/11 and 3/9/12- blockages in both IJVs, azy, L-iliac, L-renal veins. CCSVI changed my life and disease.
Treated by Dake 10/19/09, McGuckin 4/25/11 and 3/9/12- blockages in both IJVs, azy, L-iliac, L-renal veins. CCSVI changed my life and disease.
-
radeck
- Family Elder
- Posts: 398
- Joined: Mon Feb 16, 2009 3:00 pm
- Contact:
Name: radeck
Male/Female: male
Age: 33
Date(s) & type of neurological diagnosis: Jan 2009, CIS. First symptoms Dec 2008.
Lesion locations, number: 1-3 lesions >3mm (in right splenum of corpus callosum and in periventricular white matter adjacent to anterior horns of pons), several smaller dots (which I suppose don't count as MS lesions).
MS treatments: Lisinopril (<shortened url>) to reduce Th1&Th17 response to CCSVI-induced micro-bleeding. Various endothelial health as well as other supplements. Embry's best bet diet with fish and poultry on and off.
MS symptoms before stenosis intervention: Ups and Downs of mostly mild symptoms: left eyelid twitching and eye pain, subtle vision issues, warm/cold sensation and numbness in left hand, stiffness in left foot and knee, tingling in feet and hands, fatigue, slight dizziness&balance problems, muscle twitches. Most of these gone since August, possibly having to do with adjusting diet and supplements and taking Lisinopril, only rare left eye lid twitching and occasional mild left hand sensory issues.
Number of relapses before intervention: had some ups and downs, but because of general mild nature of the symptoms and lack of lesion burden neuro thinks these were pseudo-relapses, or imaginary, hence still diagnosis of CIS.
EDSS before CCSVI intervention: 0-1
FSS before CCSVI intervention: 1.6
MSIS before CCSVI intervention: 29
Testing: (Y/N) Had MRV in Stanford on Oct 14 which showed both IJV's collapsed above the clavicle/collar bone. Venogram scheduled for Nov 23, to look for reason of collapse (e.g. valve below) and see if problem is "dynamic".
Edit Dec 13: 5 stents were placed to my surprise on Nov 23, including in upper IJV area and azygos. Later noticed irregular heartbeat. EKG on Nov 24 confirmed this and echo revealed that left upper IJV stent had dislodged and migrated into right ventricle. Had emergency open heart surgery with heart-lung bypass, during which stent was retrieved from RV through incision into the right atrium. Many worrisome problems since, some likely due to heart surgery and having been on the heart-lung machine, others may be due to stents.
Male/Female: male
Age: 33
Date(s) & type of neurological diagnosis: Jan 2009, CIS. First symptoms Dec 2008.
Lesion locations, number: 1-3 lesions >3mm (in right splenum of corpus callosum and in periventricular white matter adjacent to anterior horns of pons), several smaller dots (which I suppose don't count as MS lesions).
MS treatments: Lisinopril (<shortened url>) to reduce Th1&Th17 response to CCSVI-induced micro-bleeding. Various endothelial health as well as other supplements. Embry's best bet diet with fish and poultry on and off.
MS symptoms before stenosis intervention: Ups and Downs of mostly mild symptoms: left eyelid twitching and eye pain, subtle vision issues, warm/cold sensation and numbness in left hand, stiffness in left foot and knee, tingling in feet and hands, fatigue, slight dizziness&balance problems, muscle twitches. Most of these gone since August, possibly having to do with adjusting diet and supplements and taking Lisinopril, only rare left eye lid twitching and occasional mild left hand sensory issues.
Number of relapses before intervention: had some ups and downs, but because of general mild nature of the symptoms and lack of lesion burden neuro thinks these were pseudo-relapses, or imaginary, hence still diagnosis of CIS.
EDSS before CCSVI intervention: 0-1
FSS before CCSVI intervention: 1.6
MSIS before CCSVI intervention: 29
Testing: (Y/N) Had MRV in Stanford on Oct 14 which showed both IJV's collapsed above the clavicle/collar bone. Venogram scheduled for Nov 23, to look for reason of collapse (e.g. valve below) and see if problem is "dynamic".
Edit Dec 13: 5 stents were placed to my surprise on Nov 23, including in upper IJV area and azygos. Later noticed irregular heartbeat. EKG on Nov 24 confirmed this and echo revealed that left upper IJV stent had dislodged and migrated into right ventricle. Had emergency open heart surgery with heart-lung bypass, during which stent was retrieved from RV through incision into the right atrium. Many worrisome problems since, some likely due to heart surgery and having been on the heart-lung machine, others may be due to stents.
Last edited by radeck on Sat Jan 16, 2010 7:44 am, edited 22 times in total.
- Rose2
- Family Elder
- Posts: 274
- Joined: Sat Sep 12, 2009 2:00 pm
- Location: SF area
- Contact:
MS History
CCSVI TRACKING 10/30/2009
MS HISTORY
Rose
Female
56 yo
RRMS diagnosed JULY 2001. Large egg sized lesion located in brain stem in 2001. Resulting in FAST, almost complete bilateral paralysis until MS diagnosed in hospital ICU at Stanford. Out of hospital after 8 days in July 2001 and finishing Solumedrol IV.
The lesion that was in my brain stem 2001 that was so large, is no longer visible or cannot be seen on MRI! It was not seen again after 2002. This has surprised all of the medical people that did observe it.
I returned to work for a few years in my healthcare profession but became officially Permanently Disabled from that due to lack of strength, fatigue, inabilty to make it thru a day. I am on Medicare after the 2 year wait.
I do not know all of the anatomical locations of the lesions that are noted on MRIs. There are several and some quite a bit larger than others.
However, they have not changed alot in the last 5 years or so.
3 Relapses that required IV Prednisone since Diagnosis.
AVONEX: weekly from 2002 to 2007. My personal choice to quit it because I was sick ALL week from it. 1 Relapse on Avonex. 2 after quitting Avonex. The last 2 were both in 2009.
EDSS before Intervention:: 5.5 Self Assessed on Dr. Dake's forms 10/19/2009.
FSS before intervention:
MSIS before intervention:
10/19/2009: MRI/MRV
10/20/2009: Dr. Dake at Stanford placed 2 stents on right side: WITH VENOGRAPHY
1. Azygos vein
2. High Jugular had a twist with 4 or 5 fat collaterals as a result.
RELAPSES SINCE FIRST CCSVI Intervention: NONE to date
Impact Noted So Far: It has only been 10 days but all pain is gone, CogFog is gone or not returned yet, the Blanket feeling of MS is gone.
Hard to explain, but I feel lifted and awake!!
Heat sensitivity seems better but too soon to tell I think.
EDSS as of this update:
FSS as of this update:
MSIS as of this update:
MS HISTORY
Rose
Female
56 yo
RRMS diagnosed JULY 2001. Large egg sized lesion located in brain stem in 2001. Resulting in FAST, almost complete bilateral paralysis until MS diagnosed in hospital ICU at Stanford. Out of hospital after 8 days in July 2001 and finishing Solumedrol IV.
The lesion that was in my brain stem 2001 that was so large, is no longer visible or cannot be seen on MRI! It was not seen again after 2002. This has surprised all of the medical people that did observe it.
I returned to work for a few years in my healthcare profession but became officially Permanently Disabled from that due to lack of strength, fatigue, inabilty to make it thru a day. I am on Medicare after the 2 year wait.
I do not know all of the anatomical locations of the lesions that are noted on MRIs. There are several and some quite a bit larger than others.
However, they have not changed alot in the last 5 years or so.
3 Relapses that required IV Prednisone since Diagnosis.
AVONEX: weekly from 2002 to 2007. My personal choice to quit it because I was sick ALL week from it. 1 Relapse on Avonex. 2 after quitting Avonex. The last 2 were both in 2009.
EDSS before Intervention:: 5.5 Self Assessed on Dr. Dake's forms 10/19/2009.
FSS before intervention:
MSIS before intervention:
10/19/2009: MRI/MRV
10/20/2009: Dr. Dake at Stanford placed 2 stents on right side: WITH VENOGRAPHY
1. Azygos vein
2. High Jugular had a twist with 4 or 5 fat collaterals as a result.
RELAPSES SINCE FIRST CCSVI Intervention: NONE to date
Impact Noted So Far: It has only been 10 days but all pain is gone, CogFog is gone or not returned yet, the Blanket feeling of MS is gone.
Hard to explain, but I feel lifted and awake!!
Heat sensitivity seems better but too soon to tell I think.
EDSS as of this update:
FSS as of this update:
MSIS as of this update:



