If you have an MS diagnosis, you are likely to have a constellation of essential nutrient imbalances that have been extensively researched. b12 deficit is the oldest and best known one to watch out for as an ms mimic. more recently, vitamin d3 status been established as a contributing factor. for others the evidence base re ms is still incrementally inching its way up to translation (or not) into mainstream practice.
in the meantime, we can aim for health. Whether MS seems like a possibility or you have been diagnosed already, you might be interested in working to maximize wellness prior to, or in conjunction with, any related MS investigations.
easy first steps (no tests or waiting required):
1. follow the latest evidence based food guides as best you can. unhealthy food is artificially cheap - avoid spending on empty calories.
2. invest in a high quality multivitamin/mineral (the ones for active individuals pack a stronger nutritional punch), high quality fish oil and if needed, vitamin d3 (with careful attention to mineral cofactors, especially magnesium - the RDAs for magnesium are under review at present and may increase in future)
3. maintain a regular exercise regimen (remember to nourish according to the demands you place on your body)
4. note that it's relatively easy, even if it can take a while, to create an imbalance when working with individual essential nutrient supplements or dietary extremes. safety trials don't necessarily last long enough for potential problems to be recorded. sometimes things that should be monitored, aren't. over the long term, diversity and moderation are key.
and now for the more detailed stuff:
the first thing to understand when beginning nutrition inquiries, is the unfortunate language of the lab. Specifically, the statistical term 'normal'.
The 'normal' range (perhaps more familiarly an area under a 'bell curve'), more properly known as the 'reference interval', is often quite a broad band (ie the mean +/- 2 standard deviations), which covers 95% of the population under the curve. the remaining 5% considered non-normal are represented by the 2.5% under the left tail (below normal) and right tail (above normal) respectively. with some exceptions, labs are only going to red flag those particularly low and high results.

*if only* 95% of the population were actually healthy. we're not, therefore in many cases the 'normal' range or 'reference interval' includes both sick and healthy people, much in the way that the curve describes the range of typical results on academic tests. most marks, high or low, are 'normal'. we're not all A students in the health department.
in some cases it is possible to identify a smaller range within the normal range that can be described as 'optimal'. for nutrients where some of this work has made it into lab practice, you see the within-normal ranges and implications on your results. these within-normal levels are termed 'decision limits'. one established nutritional example is serum ferritin as an indicator of iron status. for different level ranges, the lab result will indicate interpretations like 'probably deficient' 'possibly deficient' 'probably not deficient' 'possible iron overload' and so on. vitamin d3 is another essential nutrient with bands indicating deficiency, insufficiency, sufficiency and possible toxicity. the bands and associated ranges can vary depending on the source authority. when a nutrient level is dangerously low a health professional may recommend supplementation. it can be unwise to address single nutrient deficits without considering essential nutritional cofactors, especially in the long term.
essential nutrient levels can travel outside the optimal range for many reasons. One possibility to consider is suboptimal status due as applicable to inadequate nutrient intake (recommended daily intake amounts assume individuals are of 'reference weight' - if you're heavier than reference, you may not be getting enough), absorption, utilization, or stores. medications, smoking, alcohol use, certain food choices/combinations and disease processes can interfere with nutrient status as well.
taking zinc status as an example, normal range for serum zinc might be 10-20 umol/L. ms patients typically average in the low teens. healthy controls often average in the high teens. (see related content re plasma below)
some years ago now, a patient here at TIMS asked for a serum zinc test and was told the level was fine. When the patient asked for specifics the result info was 10.083 umol/L (normal range was 10-20 there). This patient was not told that the level was suboptimal, or even borderline deficient, just that it was 'fine' - ie the computer did not red flag it because the value was within the min and max setpoints. meanwhile by my hospital lab's standards, at which the normal range for serum zinc is (was) 11.5-18.5 umol/L (adhere(d) to the regional standard (at the time)), the same TIMS patient would be considered deficient. but, given a different lab set up, in her case everything was apparently just fine.
another consideration: some labs test zinc in plasma vs serum. locally, this transition from serum zinc to plasma zinc as the standard has taken place. the reference interval for plasma zinc is lower than the earlier one for serum zinc, because serum results can be affected by red blood cell zinc content. this is not the case for plasma. the learning curve is ongoing.
science is still working the zinc nuances out, but you can at least understand whether your status is or is not consistent with findings in ms patients and whether you could take action to be more consistent with results for healthy controls.
intake studies:
- New Insights on the Nutrition Status and Antioxidant Capacity in Multiple Sclerosis Patients
https://www.mdpi.com/2072-6643/11/2/427
"...We found that MS patients consumed a more limited diet compared with the healthy group, indicated by a lower average of 31 nutrients and by consumption levels of zinc and thiamine below the recommended daily intake. Both consumption and measured iron values were significantly lower in MS patients, with the lowest measures in the severe MS group..."
- Total intake of different minerals and the risk of multiple sclerosis
https://n.neurology.org/content/early/2 ... 0.abstract
"Our findings suggest that mineral intake is not an important determinant of MS risk"
status studies:
- Zinc Status and Autoimmunity: A Systematic Review and Meta-Analysis
https://www.mdpi.com/2072-6643/10/1/68/htm
"The data presented in our work, although very heterogeneous in the manner of collecting and investigating samples, have proved to be extremely consistent in witnessing a deficiency of zinc in serum and plasma of patients compared to controls."
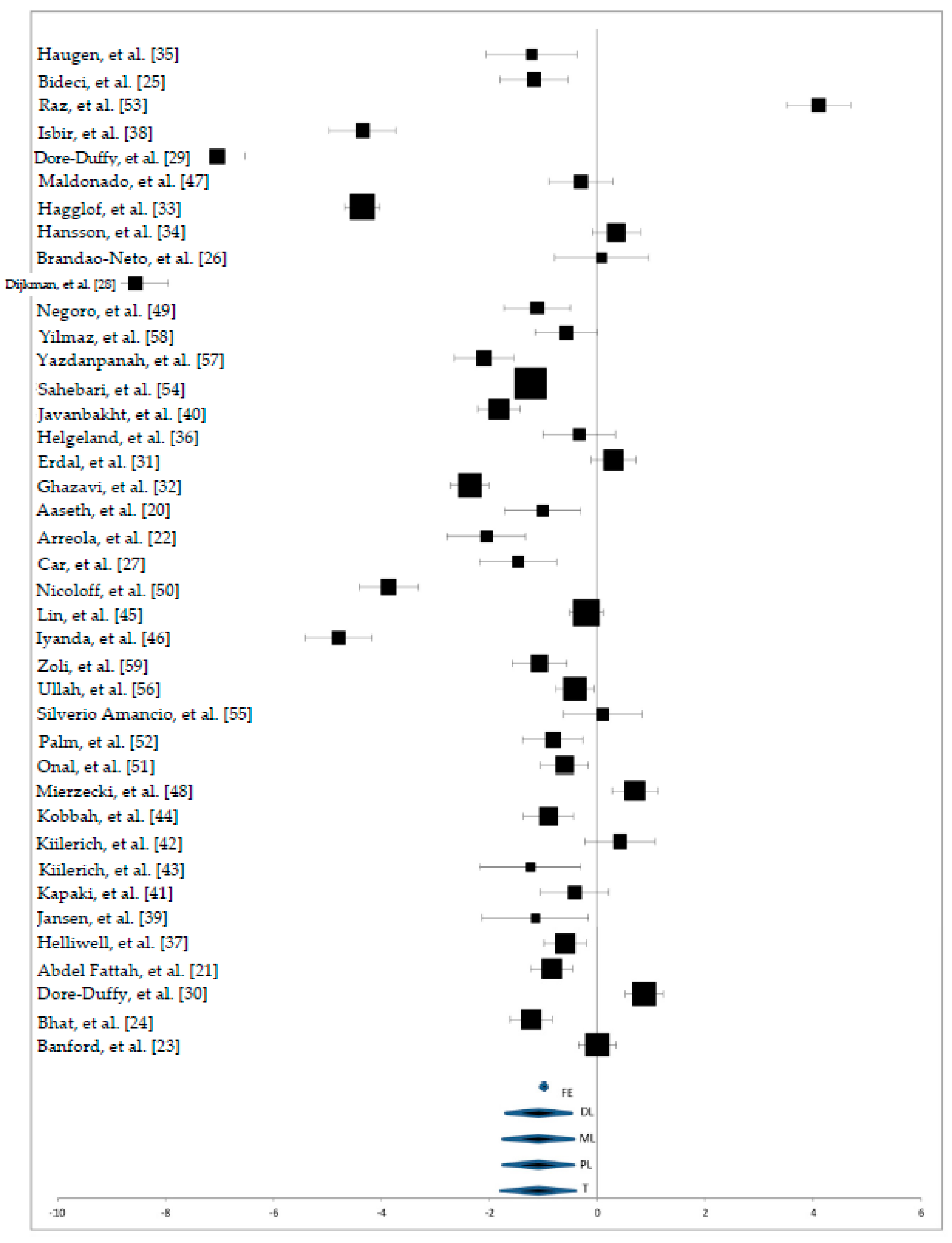
- Lower Serum Zinc Levels in Patients with Multiple Sclerosis Compared to Healthy Controls
https://www.mdpi.com/2072-6643/10/8/967
"MS patients showed significantly lower zinc concentrations (mean (SD)) than HCs (12.5 (2.1) µmol/L vs. 14.6 (2.3) µmol/L, p < 0.001)"
- Zinc in Multiple Sclerosis: A Systematic Review and Meta-Analysis
https://journals.sagepub.com/doi/full/1 ... 1416651511
"The result of the meta-analysis shows a reduction in serum or plasma Zn levels in patients with MS ... The studies measuring whole blood and erythrocyte Zn levels found up to several times higher levels of Zn in patients with MS compared with healthy controls with decreasing levels during attacks in relapsing-remitting MS patients."
- Zinc and Regulation of Inflammatory Cytokines: Implications for Cardiometabolic Disease
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3407988/
"... increased demand for zinc in inflammatory conditions. The acute phase response includes a rapid decline in the plasma zinc concentration as a result of the redistribution of zinc into cellular compartments...."
- Zinc: An antioxidant and anti-inflammatory agent: Role of zinc in degenerative disorders of aging
https://www.sciencedirect.com/science/a ... 2X14001503
"Zinc in human plays an important role in cell mediated immunity and is also an antioxidant and anti-inflammatory agent."
(my 2c, author prasad ^ is pretty much the godfather of zinc and human health research)
...
Another example: the normal range for uric acid can range from as low as 90 umol/l to as high as 480 umol/L (and at my lab, 140-360).
MS patients have been found to average 194 umol/L (lower in relapse, higher in remission). Healthy controls sat in the 290-300 umol/L range:
- Serum uric acid levels in multiple sclerosis patients correlate with activity of disease and blood-brain barrier dysfunction.
https://www.ncbi.nlm.nih.gov/pubmed/11985629
- Low serum uric acid levels in patients with multiple sclerosis and neuromyelitis optica: An updated meta-analysis
https://www.ncbi.nlm.nih.gov/pubmed/27645338
- Is it time to revise the normal range of serum uric acid levels?
https://www.ncbi.nlm.nih.gov/pubmed/24867507
Interestingly, some studies have demonstrated a positive correlation between uric acid levels and zinc levels. So if you are low in essential zinc you may be low in uric acid too. this was certainly the case for me. low normal uric acid for years (188-194 umol/l) until i took my zinc level from deficient 8.6 umol/l to high normal 16.7 umol/l, and uric acid suddenly jumped to 278 umol/l. much better!
- Longitudinal study of serum zinc and copper levels in hemodialysis patients and their relation to biochemical markers
https://link.springer.com/article/10.13 ... :113:3:209
"Uric acid and parathyroid hormone ... were significantly (p<0.05) and linearly related with serum zinc".
- Effect of low zinc intake and oral contraceptive agents on nitrogen utilization and clinical findings in young women
https://www.ncbi.nlm.nih.gov/pubmed/925768
pdf https://bit.ly/2XrVYmg
"Uric acid, the chief end product of purine metabolism, decreased about 20% in both groups. The decrease may be accounted for by the low purine content of the formula diet, the relatively lower N in takes during the study, or a reduction in nucleic acid synthesis and total body pool size due to tissue zinc depletion"
- Oral Zinc Therapy Normalizes Serum Uric Acid Level in Wilson’s Disease Patients
https://www.sciencedirect.com/science/a ... 2915368695
"...These results suggest that oral zinc therapy can normalize UrA metabolism in Wilson’s disease by improving liver dysfunction and increasing UrA synthesis."
vitamin b complex (all of them, particularly b12 and b1)
vitamin d3
vitamin e
magnesium
selenium
zinc
essential polyunsaturated fatty acids
conventional bloodwork does not necessarily capture all or even most of the above. if you haven't already done so, it's worth starting in on the learning curve. at a minimum, you can evaluate the degree to which your status quo diet is providing these nutrients not just at a bare minimum level, but in nourishing amounts per calorie (nutrient density).
research and experiences with these and other nutrients are posted in the dedicated 'sticky' topics found at the top of the natural approach forum. have fun reading up!
