Vitamin D: Scientific Studies & News
Re: Vitamin D: Scientific Studies & News
Efficacy of high-dose vitamin D3 supplementation in vitamin D deficient pregnant women with multiple sclerosis: Preliminary findings of a randomized-controlled trial
Abstract
Background: The aim of this preliminary study was to assess the safety and efficacy of high-dose oral vitamin D3 supplementation during pregnancy in women with multiple sclerosis (MS) in Isfahan, Iran.
Methods: In a single center open-label randomized, controlled clinical Phase I/II pilot study, 15 pregnant women with confirmed MS with low serum 25-hydroxyvitamin D (25(OH)D) levels were randomly allocated to receive either 50,000 IU/week vitamin D3 or routine care from 12 to 16 weeks of gestation till delivery. The main outcome measures were mean change in serum 25(OH)D levels, expanded disability status scale (EDSS) score, and number of relapse events during pregnancy and within 6 months after delivery.
Results: Average serum 25(OH)D level at the end of trial in vitamin D3 supplemented group was higher than routine care group (33.7 ng/mL vs. 14.6 ng/ml, P < 0.050). In vitamin D3 group, the mean EDSS did not changed 6 months after delivery (P > 0.050), whereas in routine care group, the mean EDSS increased from 1.3 (0.4) to 1.7 (0.6) (P < 0.070). Women in vitamin D3 group appeared to have fewer relapse events during pregnancy and within 6 months after delivery. No significant adverse events occurred.
Conclusion: Adding high dose vitamin D3 supplementation during pregnancy to routine care of women with MS had significant effect on the serum 25(OH)D levels, EDSS and number of relapse events during pregnancy and within 6 months after delivery.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4449396/
Re: Vitamin D: Scientific Studies & News
Is vitamin D metabolism altered in dogs with cancer?
A recent study published in the Journal of Veterinary Internal Medicine evaluated the impact of cancer on vitamin D status in dogs.
Like humans, our furry companions are living longer than ever before, and thus experience an increased risk of developing cancer throughout their lifetime. In fact, dogs develop more types of cancer than all other companion animals.
Approximately 1 in 4 dogs are diagnosed with cancer each year. In addition, cancer is responsible for 47% of canine deaths, making this disease the leading cause of canine mortality.
Vitamin D plays a crucial role in cancer prevention and treatment. For example, vitamin D regulates cell differentiation and cell growth, two important components in cancer prevention. In addition, vitamin D can recognize when cells become dysfunctional and initiate cell apoptosis, or programmed cell death.
Research continues to support the role of vitamin D in cancer prevention and treatment among humans. In fact, low vitamin D status has been linked with cancer development, impaired treatment outcome and mortality in people.
Research evaluating the role of vitamin D status in cancer among dogs is in its infancy. One study suggested that dogs with vitamin D levels below 40 ng/ml (100 nmol/l) experienced a 3.9 fold increased risk of developing cancer. Research has also shown that dogs with cancer are more likely to be vitamin D deficient than their healthy counterparts.
Unfortunately, canine vitamin D metabolism differs from humans and is not well understood. Additionally, the reference range for vitamin D status in canines varies significantly, depending on the laboratory used. These factors make it difficult to draw conclusions based off the available data.
Therefore, researchers recently conducted a study to evaluate whether various forms of cancer may affect a dog’s vitamin D status. They also aimed to identify other factors that may impact vitamin D levels among healthy dogs and dogs with cancer.
All dogs included in the study were client owned. Those were considered healthy when they presented a normal medical history, physical exam, complete blood count and biochemical profile. Dogs with newly diagnosed cancer were evaluated at the Mona Campbell Centre for Animal Cancer at the Ontario Veterinary College’s Health Centre to confirm their diagnosis.
Those who received supplements containing calcium or vitamin D, received corticosteroid treatment within two weeks of enrollment, were less than 2 years old or were diagnosed with systemic or infectious diseases (aside from cancer) were excluded from the study. A total of 92 dogs met this criteria, and thus were included in the analysis. Of these dogs, 21 had osteosarcoma, 27 had lymphoma, 21 had mast cell tumors and 23 acted as healthy controls.
The researchers recorded the dog’s dietary vitamin D intake, breed, age, sex, neuter status, body weight, body condition score (BCS) and muscle condition score (MCS). All healthy dogs were followed for one year after enrollment to confirm sustained health. All dogs received a blood draw to measure ionized calcium and parathyroid levels. Ionized calcium is routinely measured to observe blood calcium levels. They also measured the following vitamin D metabolites:
Calcidiol or 25(OH)D: The form of vitamin D that has undergone the first activation step in the liver to become a prohormone. This is the form of vitamin D widely measured to determine vitamin D status.
Calcitriol or 1,25(OH)2D3: The hormonally active form of vitamin D.
24,25(OH)2D: A metabolite associated with CYP24A1, an enzyme that breaks down circulating 25(OH)D and 1,25(OH)2D3 . Research suggests CYP24A1 is upregulated in dogs with cancer, resulting increased 24,25(OH)2D and decreased 25(OH)D levels.
Here is what the researchers found:
The average vitamin D status of healthy dogs was 51.3 ng/ml (128.25 nmol/l); whereas dogs with osteosarcoma had an average of 41.9 ng/ml (104.75 nmol/l), lymphoma had 41.1 ng/ml (102.75 nmol/l) and mast cell tumor had 44.9 ng/ml (112.25 nmol/l).
Dogs with osteosarcoma had significantly higher body weight than dogs with lymphoma (p < 0.05).
Cancer type, serum calcium and 24,25(OH)2 levels were significantly associated with 25(OH)D status (p = 0.004, p = 0.047 and p = 0.001, respectively).
Cancer was independently associated with serum calcium levels (p = 0.005).
As serum calcium levels increased in dogs with cancer, so did their 25(OH)D levels; however, serum 25(OH)D levels decreased as serum calcium levels increased in healthy dogs.
Vitamin D status was not affected by the dog’s age, sex, neuter status, body weight, BCS, MCS or their plasma parathyroid levels (p > 0.05).
The researchers concluded,
“Results support a relationship between cancer and altered vitamin D metabolism in dogs, mediated by plasma ICa concentrations. The CYP24A1 activity and plasma [ionized calcium] should be measured in studies examining plasma 25(OH)D concentrations in dogs.”
Research continues to support the role of vitamin D status in canine health, showcasing the need for more clarity regarding vitamin D requirements for dogs, beyond prevention of rickets.
In order to determine whether vitamin D supplementation may prevent or help treat cancer in dogs, clinical trials are required.
Citation
Sturges, M. Is vitamin D metabolism altered in dogs with cancer? The Vitamin D Council Blog & Newsletter, 2017.
https://www.vitamindcouncil.org/is-vita ... th-cancer/
Re: Vitamin D: Scientific Studies & News
Vitamin D Offers Hope for Multiple Sclerosis Multiple sclerosis (MS) is a disease that attacks the central nervous system and affects millions of people around the world. There is not yet a cure for MS.
As an autoimmune disease, in which the body attacks its own healthy tissues and cells, MS destroys myelin, a substance that surrounds nerve fibers in the brain and spinal cord1 much as insulating material wraps around electrical wire.
By destroying myelin, MS damages the nerves and leaves them unable to send electrical impulses throughout the body. This can make everything from walking to seeing to breathing an arduous if not impossible task for those affected.
While there are a few medications that treat some of the symptoms, none of them can cure or stop the disease, and they can produce side effects.2,3 Annual increases in the prices of these drugs have made many of them unattainable by some patients desperate for any respite from this debilitating illness.3
An array of new data indicates that proper supplementation with low-cost vitamin D can induce a meaningful beneficial effect on multiple sclerosis patients.
According to the latest research, vitamin D offers hope for those suffering from multiple sclerosis. Ample data show that low levels of vitamin D are associated with an increased risk of developing MS,4-7 and the vitamin has been shown to be effective in patients by reducing MS-caused inflammation. Studies show that having adequate levels of vitamin D can not only decrease the risk of developing MS, but can also delay its progression.4,7-10
In addition, vitamin D has been shown to be useful for both preventing and treating a number of other debilitating neurodegenerative diseases, including Parkinson’s and Alzheimer’s.11-16
In this article, you will learn what vitamin D blood levels are required to ensure adequate protection, and how much you need to take in order to achieve these levels.
Because vitamin D is very affordable and safe, no one should suffer the potential adverse consequences of having low levels of this crucial nutrient.
Vitamin D Slows the Progression of MS
Longevity Compounds
A study in JAMA Neurology examined the possible link between vitamin D levels and MS disease progression in 1,482 men and women with relapsing-remitting MS (the most common form of MS) who were being treated with a common MS prescription medication (interferon beta-1b).7
Over an 18-month period, researchers measured vitamin D blood levels, conducted multiple brain MRI (magnetic resonance imaging) scans to assess MS progression, and monitored the relapse rate and progression using the Expanded Disability Status Scale, a method to quantify impairments of ambulation, activity levels, and ability to communicate.
The researchers determined that vitamin D had a significant effect on MS. They reported that those patients with the highest levels of vitamin D (greater than 40 ng/mL) had the lowest rates of new MS lesions.
In addition, a study published in JAMA found that low circulating vitamin D levels are associated with the risk of developing MS.4 Specifically, they found that men and women with low levels of vitamin D (<25 ng/mL) had a much higher risk of developing MS when compared with those who had high levels (>40 ng/mL).
Even more recent studies have shown that optimal vitamin D levels can help slow MS activity, delay disease progression, and delay conversion of MS to secondary-progressive MS, a deadlier and more debilitating form of the disease.9,10
In a 2014 article in JAMA Neurology, researchers measured vitamin D levels in patients who had suspected MS over a 2-year period.9 What they found was nothing short of amazing. The patients who had an average increase in their serum vitamin D of 20 ng/mL in the first 12 months of the study experienced the following improvements over the 5-year length of the study:
57% lower rate of new active brain lesions seen on MRI,
57% lower relapse rate, and a
25% lower yearly increase in brain lesion volume.
Lastly, a 2015 study on patients with relapsing-remitting MS examined whether or not vitamin D levels could predict conversion to secondary-progressive MS.10 In this 3-year study, researchers showed that those patients who had low vitamin D levels (2-14 ng/mL) had a 5.9 times increased risk of shifting into the secondary-progressive form of MS when compared with people who had high levels (23-52 ng/mL).
Together, these studies make it clear that vitamin D can not only decrease the risk of developing MS, but can also delay its progression in those who already have it.
Vitamin D and Neurodegenerative Diseases
In addition to preventing and helping to treat MS, other studies show that vitamin D plays a critical role in preventing other neurodegenerative diseases, such as Parkinson’s and Alzheimer’s.
Parkinson’s disease
Parkinson’s disease is a disorder of the central nervous system that causes progressive and debilitating tremors and difficulty moving. While there is no cure for this disease, recent research has shown that maintaining optimal vitamin D levels may offer a way to prevent it.
In a 2014 paper in the journal Neurological Sciences, researchers did a meta-analysis of studies potentially linking low levels of vitamin D to an increased risk of Parkinson’s.11 After reviewing seven observational studies that included 1,008 patients and 4,536 controls, the authors concluded in no uncertain terms that “low vitamin D levels are associated with an increased risk of PD (Parkinson’s disease).”
A 2015 paper added proof to this powerful statement.12 In this large meta-analysis including 5,690 patients with Parkinson’s and 21,251 controls, the researchers determined that patients with low vitamin D levels (<20 ng/mL) had a two-fold increase in the risk of developing Parkinson’s. Taking it one step further, they also found that vitamin D supplementation was associated with a decreased risk of developing Parkinson’s by a significant 38%.
Alzheimer’s disease
Alzheimer’s disease is the most common form of dementia and has become a 21st century epidemic among America’s aging population. While expensive prescription pharmaceuticals can offer only minimal help in treating the symptoms, evidence shows that maintaining optimal levels of vitamin D can provide a safe and effective way to protect against this disease.
A paper in the journal Neurology followed 1,658 men and women, aged 69-79, over 5.6 years to determine if there was an association between vitamin D levels and Alzheimer’s. The researchers found that people with severe vitamin D deficiency (<10 ng/mL) had a 122% increased risk of developing Alzheimer’s. For individuals that were deficient (greater than or equal to 10 ng/mL to less than 20 ng/mL) there was a 51% increased risk.15 This led the authors to conclude: “our studies confirm that vitamin D deficiency is associated with a substantially increased risk of all-cause dementia and Alzheimer’s disease.”
Another study evaluated the relationship between vitamin D and cognitive function in 2,777 men and women aged 70-79.17 The researchers studied these men and women over a 4-year period, measuring both their vitamin D levels and cognitive performance using multiple tests. The results were unequivocal. Those people with low vitamin D levels (this time, defined as <30 ng/mL) had worse mental functioning and greater decline in their cognition when compared to those with higher levels of vitamin D.
To obtain high enough blood levels of vitamin D to help protect against cognitive decline, it is important to check blood levels of vitamin D and supplement with 5,000 to 8,000 IU of vitamin D daily depending on individual blood levels. Life Extension suggests that optimal blood levels of 25-hydroxyvitamin D using LabCorp’s measuring standard are between 50 to 80 ng/mL.
Summary
Vitamin D is a widely available nutrient essential for optimal health. Receptors for this essential compound have been found in almost every cell in the body.
Vitamin D has been shown to be associated with both preventing and slowing the progression of a number of debilitating neurodegenerative diseases, including MS, Parkinson’s, and Alzheimer’s.
The recommended daily allowance (RDA) set by the government, 600-800 IU a day, is woefully inadequate to achieve the optimal levels of vitamin D in the body that can help ward off these diseases.
With most people deficient in vitamin D—even if they’re taking the RDA—more and more experts recognize that supplementing with at least 5,000 to 8,000 IU is crucial to stem a number of deadly diseases. It should be taken with the heaviest meal of the day to increase absorption.
If you have any questions on the scientific content of this article, please call a Life Extension® Wellness Specialist at 1-866-864-3027.
References
Available at: http://emedicine.medscape.com/article/1 ... ew#showall. Accessed May 31, 2016.
Gohil K. Multiple Sclerosis: Progress, but No Cure. P T. 2015;40(9):604-5.
Hartung DM, Bourdette DN, Ahmed SM, et al. The cost of multiple sclerosis drugs in the US and the pharmaceutical industry: Too big to fail? Neurology. 2015;84(21):2185-92.
Munger KL, Levin LI, Hollis BW, et al. Serum 25-hydroxyvitamin D levels and risk of multiple sclerosis. Jama. 2006;296(23):2832-8.
Duan S, Lv Z, Fan X, et al. Vitamin D status and the risk of multiple sclerosis: a systematic review and meta-analysis. Neurosci Lett. 2014;570:108-13.
Harandi AA, Harandi AA, Pakdaman H, et al. Vitamin D and multiple sclerosis. Iran J Neurol. 2014;13(1):1-6.
Fitzgerald KC, Munger KL, Kochert K, et al. Association of Vitamin D Levels With Multiple Sclerosis Activity and Progression in Patients Receiving Interferon Beta-1b. JAMA Neurol. 2015;72(12):1458-65.
Simpson S, Jr., Taylor B, Blizzard L, et al. Higher 25-hydroxyvitamin D is associated with lower relapse risk in multiple sclerosis. Ann Neurol. 2010;68(2):193-203.
Ascherio A, Munger KL, White R, et al. Vitamin D as an early predictor of multiple sclerosis activity and progression. JAMA Neurol. 2014;71(3):306-14.
Muris AH, Rolf L, Broen K, et al. A low vitamin D status at diagnosis is associated with an early conversion to secondary progressive multiple sclerosis. J Steroid Biochem Mol Biol. 2015.
Lv Z, Qi H, Wang L, et al. Vitamin D status and Parkinson’s disease: a systematic review and meta-analysis. Neurol Sci. 2014;35(11):1723-30.
Shen L, Ji HF. Associations between Vitamin D Status, Supplementation, Outdoor Work and Risk of Parkinson’s Disease: A Meta-Analysis Assessment. Nutrients. 2015;7(6):4817-27.
Balion C, Griffith LE, Strifler L, et al. Vitamin D, cognition, and dementia: a systematic review and meta-analysis. Neurology. 2012;79(13):1397-405.
Schlogl M, Holick MF. Vitamin D and neurocognitive function. Clin Interv Aging. 2014;9:559-68.
Littlejohns TJ, Henley WE, Lang IA, et al. Vitamin D and the risk of dementia and Alzheimer disease. Neurology. 2014;83(10):920-8.
Banerjee A, Khemka VK, Ganguly A, et al. Vitamin D and Alzheimer’s Disease: Neurocognition to Therapeutics. Int J Alzheimers Dis. 2015;2015:192747.
Wilson VK, Houston DK, Kilpatrick L, et al. Relationship between 25-hydroxyvitamin D and cognitive function in older adults: the Health, Aging and Body Composition Study. J Am Geriatr Soc. 2014;62(4):636-41.
http://www.lifeextension.com/Magazine/2 ... is/Page-01
Re: Vitamin D: Scientific Studies & News
Experimental Autoimmune Encephalomyelitis Is Successfully Controlled by Epicutaneous Administration of MOG Plus Vitamin D Analog.
Abstract
Multiple sclerosis (MS) is an inflammatory and demyelinating disorder of the central nervous system (CNS). Experimental autoimmune encephalomyelitis (EAE) has been widely employed to evaluate new strategies to control MS, including procedures to induce immunological tolerance. Considering that skin exposure to protein antigens can induce tolerance and that vitamin D analogs conserve immunomodulatory potential and are less toxic, we investigated the efficacy of epicutaneous application of a myelin oligodendrocyte glycoprotein peptide (MOG35-55) associated with paricalcitol (PARI) on EAE development. Three and 11 days after EAE induction, C57BL/6 mice were treated with an occlusive patch containing MOG plus PARI. Clinical parameters were daily assessed, whereas immunological and histological evaluations were performed during the acute EAE phase. MOG and MOG + PARI significantly controlled disease development reducing weight loss and clinical score. Moreover, MOG and MOG + PARI reduced the inflammatory process and preserved the myelin sheath in the CNS. High percentages of Foxp3+ regulatory T cells (Tregs) and lower MHCII fluorescence intensity in dendritic cells in draining lymph nodes were concomitantly observed. MOG + PARI association was, however, more efficient being able to reduce disease incidence and clinical scores more significantly than MOG or PARI alone. This experimental group also displayed a higher ratio between mRNA expression for Foxp3 and RORc and a higher percentage of Foxp3+ cells in the CNS. Modulation of activation markers observed in microglial cells eluted from EAE treated mice were confirmed by in vitro studies with the BV-2 microglial cell line. The results show that MOG + PARI association applied by an epicutaneous route controlled EAE development. Protective involved mechanisms include mainly a higher proportion of Tregs and also a direct immunomodulatory effect of PARI on microglial cells.
https://www.ncbi.nlm.nih.gov/pubmed/29085356
Re: Vitamin D: Scientific Studies & News
Vitamin D and Immunomodulation: Is It Time to Change the Reference Values? Abstract
The term "vitamin D" refers to two chemical compounds - ergosterol, or vitamin D2, and cholecalciferol, or vitamin D3. Active vitamin D3 is correctly regarded as a neurohormone due to its pleiotropic biological activities. Although the relation between vitamin D and calcium-phosphorus metabolism has never been discussed, the knowledge on many other roles vitamin D plays is growing fast. Briefly, vitamin D immunomodulation includes attenuation and stimulation of Th1 and Th2 cell proliferation, respectively. Similarly, vitamin D can induce or inhibit the synthesis, secretion, and release of anti- inflammatory (IL-4 and IL-10) and pro-inflammatory (IL-1, TNF-α, IFN-γ) cytokines, respectively. Redefining vitamin D reference values seems to be either a critical or urgent issue. There is not so far a univocal consensus on the reference values of vitamin D status, mainly because of such reference value rates on the basis of the parathyroid hormone (PTH) plasma response. The optimal serum concentration of vitamin D has been considered to lead not to a PTH elevation. Such criterion is clearly resulted from a partial knowledge of the biology of vitamin D so that it can be considered at least obsolete.Based on the distribution of vitamin D levels among healthy individuals and inflammatory/autoimmune patients, an appropriate review of vitamin D reference values is required, following adequate standardization and harmonization of the cut-off, as well as taking into account the ethnic/cultural/geographical features influencing vitamin D status.
https://www.ncbi.nlm.nih.gov/pubmed/28801380
Re: Vitamin D: Scientific Studies & News
Lower Serum 25-Hydroxyvitamin D Level is Associated With 3 Types of Autoimmune Thyroid Diseases Abstract
Autoimmune thyroid diseases (AITD) are common autoimmune disorders. A few studies have analyzed the association between serum vitamin D levels and AITD, and available data remain inconclusive.
The aim of this study was to evaluate the association between serum vitamin D levels and 3 types of AITD, that is Graves’ disease (GD), Hashimoto's thyroiditis (HT), and postpartum thyroiditis (PPT).
Two independent case-control studies were designed. The first is a cross-sectional case-control study in which we examined the levels of 25(OH)D in patients with newly diagnosed GD or HT and in controls; the second is a nested case-control study in which we compared 25(OH)D levels in 610 women who developed PPT during the follow-up after delivery and those who did not.
Compared with the controls, GD patients and HT patients had significantly lower 25(OH)D levels. PPT cases also had a lower serum 25(OH)D concentration than controls. Serum 25(OH)D levels were associated with neither antithyroid peroxidase antibody nor antithyroglobulin antibody in GD and HT. There was no significant relationship between thyroid-stimulating hormone and 25(OH)D levels. Every 5 nmol/L increase in serum 25(OH)D concentrations was associated with a 1.55-, 1.62-, and 1.51-fold reduction in GD, HT, and PPT risk, respectively.
We observed a lower serum vitamin D levels in AITD patients compared with controls. The lower the vitamin D level is, not vitamin D deficiency per se, the higher the risk for developing AITD will be. However, vitamin D does not have strong association with the titers of thyroid antibodies or the levels of thyroid hormones.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4616844/
Re: Vitamin D: Scientific Studies & News
Vitamin D status significantly affects risk of multiple sclerosis among Finnish women
Multiple sclerosis (MS) is an immune-mediated disease of the central nervous system (CNS) which disrupts the flow of nervous signals between the brain and spinal cord to the rest of the body. Symptoms of this condition are variable, and it is likely that no two MS patients will have the same symptomatic experience. Symptoms may include fatigue, weakness, numbness or tingling, cognitive impairment, pain, vision loss, depression and more.
Though the cause of MS is still unknown, a combination of environmental, genetic, infectious and immunological factors are thought to contribute to the onset of this condition. Additionally, an abundance of research has observed a relationship between multiple sclerosis and vitamin D status.
However, few studies have assessed factors that may impact future risk of MS in a healthy population. Therefore, researchers chose to evaluate a large cohort of Finnish women in order to determine if vitamin D deficiency is considered a risk factor for MS in this population.
This study included women who had participated in the Finnish Maternity Cohort (FMC). Beginning in 1983, this cohort analysis included over 800,000 pregnant women who had their serum 25(OH)D status tested between 10-14 weeks of gestation. The researchers from this study identified 1,092 women who were clinically diagnosed with MS between 1983 and 2009 and 2,123 age and location matched controls.
Serum vitamin D levels were available in all individuals, prior to diagnosis in the MS group. For those who participated in the FMC over the years and had several vitamin D tests administered, these levels were averaged. Additionally, season of the blood draws were recorded to use in a multivariate analysis. Vitamin D levels below than 12 ng/ml (30 nmol/l) were considered vitamin D deficient, between 12-20 ng/ml (30-50 nmol/l) was considered insufficient, and levels above 20 ng/ml (50 nmol/l) were considered sufficient.
This is what the researchers found:
More than 50% of participants were vitamin D deficient, over 33% of participants had insufficient levels, only 0.04% had 25(OH)D levels above 30 ng/ml (75 nmol/l), and of these, only 0.0009% had levels above 40 ng/ml (100 nmol/l).
A 20 ng/ml (50 nmol/l) increase in vitamin D status was associated with a 39% reduced risk of 95% CI 0.44–0.85, p = 0.003).
Compared to those with levels less than 20 ng/ml (50 nmol/l), women with levels less than 12 ng/ml (30 nmol/l) had a 43% increased risk of MS.
Compared to participants with insufficient levels, deficient women had a 27% increased MS risk (95% CI 1.07–1.50, p = 0.005).
Women with the lowest levels of vitamin D had a 53%– 66% increased risk of MS compared to women with the highest levels of vitamin D (p < 0.001).
The researchers concluded:
“Our results further support and extend those of previous prospective studies of 25(OH)D levels in young adults and risk of MS, and suggests that many individuals are exposed to an increased MS risk that could be reduced by broad population-based programs to prevent vitamin D deficiency.”
There were both some strengths and weaknesses of this study that should be mentioned. A few strengths of this study include the large sample size and the use of a control group. It is important to use a control group in order to be able to compare the effect of vitamin D status in a healthy population against vitamin D status in a population with a specific disease or health condition. Also, the researchers were able to collect vitamin D status an average of 9 years prior to MS diagnosis, which limits the effect of reverse causation.
Despite these strengths, there were some limitations as well. The researchers noted they did not account for confounders such as body mass index in early life, Epstein-Barr virus infection, smoking and human leukocyte antigen status, all of which are risk factors for MS. Additionally, this population was comprised of mainly Caucasian women, which limits the generalizability of these results.
Research seems to support that higher vitamin D status is beneficial for this population. Due to the fact that vitamin D supplementation is an inexpensive and safe way to ensure your vitamin D status is within healthy range, the Vitamin D Council recommends supplementing with between 5,000-10,000 IU per day.
We asked Dr. Cannell to weigh in on this study. He replied,
“As we point out, virtually none of these women had the levels recommended by the Endocrine Society [>40 (not 30) ng/ml]. This almost certainly means this study underestimates the protective effect of vitamin D levels on MS.”
He continued,
“What vitamin D level maximizes the protective effect of vitamin D on MS? My personal experience with another autoimmune illness (autism), is that higher levels of vitamin D has been more beneficial (i.e 40 ng/ml is more beneficial than 30 ng/ml, 50 ng/ml is more beneficial than 40 ng/ml, etc. up to about 70 or 80 ng/ml). While I have not supplemented autistic children above 80 ng/ml, it is possible that the therapeutic effect of vitamin D is not maximized until levels are substantially above 100 ng/ml. Remember, as Michael Holick says, toxicity has never been convincingly demonstrated at levels less than 200 ng/ml.”
As always, we are here to answer any questions you may have about vitamin D supplementation, sun exposure and health. Please email info@vitamindcouncil.org for all questions and concerns.
Citation
Peterson, R. & Cannell, JJ. Vitamin D status significantly affects risk of multiple sclerosis in a cohort of Finnish women. The Vitamin D Council Blog & Newsletter, 10/17.
Source
Munger, K. et al. 25-Hydroxyvitamin D deficiency and risk of MS among women in the Finnish Maternity Cohort. Neurology, 2017.
https://www.vitamindcouncil.org/vitamin ... ish-women/
Re: Vitamin D: Scientific Studies & News
Vitamin D deficiency is associated with disability and disease progression in multiple sclerosis patients independently of oxidative and nitrosative stress.
Abstract
The aim of this study was to assess vitamin D status in patients with multiple sclerosis (MS) and to evaluate whether it was associated with oxidative and nitrosative stress (O&NS) markers and disability. This study included 137 patients with MS and 218 healthy controls. The markers evaluated were serum levels of 25-hydroxyvitamin D, lipid hydroperoxides, advanced oxidation protein products (AOPP), nitric oxide metabolites (NOx), and total radical-trapping antioxidant parameter TRAP/UA. Patients with 25(OH)D<20ng/mL showed higher EDSS (p=0.016), MSSS (p=0.005) and lower AOPP (p=0.046) than those with 25(OH)D≥20ng/mL. After the binary logistic regression analyses, EDSS and MSSS remained significantly associated with vitamin D deficiency. We showed that lower levels of 25(OH)D were associated with higher EDSS and MSSS independently of variables such as O&NS, age, sex, body mass index, ethnicity, MS therapy, use of interferon beta, and clinical forms of MS (odds ratio: 1.380, 95% confidence interval 1.030-1.843, p=0.031). Moreover, the study showed an association between serum levels of 25(OH)D and EDSS (r2=0.115, p=0.002), demonstrating that 25(OH)D may contribute with 11.5% of increase in EDSS. Our results suggest that vitamin D deficiency may be considered one of the predictors of the disability in MS patients, independently of their redox status and influence the progression of disability in MS.
https://www.ncbi.nlm.nih.gov/pubmed/28991684
Re: Vitamin D: Scientific Studies & News
The effect of vitamin D supplement on the score and quality of sleep in 20–50 year-old people with sleep disorders compared with control group.
Abstract
Objectives: Sleep quality may be directly related with vitamin D serum level. Some studies found that people with lower vitamin D serum level experienced a lower sleep quality. Consequently, this study aimed at determining the effect of vitamin D supplements on sleep score and quality in 20–50 year-old people with sleep disorders.
Methods: This double blind, clinical trial was performed in November 2015–February 2016 on 89 people with sleep disorders based on Petersburg's Sleep Index. Patient samples were divided randomly into two groups: intervention and placebo. At the end of the study, the data on 89 subjects (44 in intervention group and 45 people in placebo group) were examined. Intervention group received a 50 000-unit vitamin D supplement, one in a fortnight for 8 weeks. Meanwhile, placebo group received placebo. Before and after intervention, Petersburg's Sleep Quality Questionnaire, International Physical Activity Questionnaire, general information questionnaire, sun exposure, vitamin D serum level and 3-day food record questionnaire were assessed and recorded for all participants. To analyze data, t-test, chi square, ANCOVA, U-Mann–Whitney and Wilcoxon statistical tests were used.
Findings: Based on the results of the present study, at the end of the study sleep score (PSQI) reduced significantly in vitamin recipients as compared with placebo recipients (P < 0.05). This difference was significant even after modifying confounding variables (P < 0.05).
Conclusion: This study shows that the use of vitamin D supplement improves sleep quality, reduces sleep latency, raises sleep duration and improves subjective sleep quality in people of 20–50 year-old with sleep disorder.
http://www.tandfonline.com/doi/abs/10.1 ... de=ynns20&
Re: Vitamin D: Scientific Studies & News
The Big Vitamin D Mistake
Abstract
"Veugelers and Ekwarul, in a correct reanalysis of the data used by the Institute of Medicine, proved that 8895 IU/d are needed for 97.5% of individuals to achieve values ≥50 nmol/L. Heaney et al. confirmed that finding, reporting that 6201 IU/d were needed to achieve the Endocrine Society’s recommendation of 75 nmol/L and 9122 IU/day to reach 100 nmol/L."
Since 2006, type 1 diabetes in Finland has plateaued and then decreased after the authorities’ decision to fortify dietary milk products with cholecalciferol. The role of vitamin D in innate and adaptive immunity is critical. A statistical error in the estimation of the recommended dietary allowance (RDA) for vitamin D was recently discovered; in a correct analysis of the data used by the Institute of Medicine, it was found that 8895 IU/d was needed for 97.5% of individuals to achieve values ≥50 nmol/L. Another study confirmed that 6201 IU/d was needed to achieve 75 nmol/L and 9122 IU/d was needed to reach 100 nmol/L. The largest meta-analysis ever conducted of studies published between 1966 and 2013 showed that 25-hydroxyvitamin D levels <75 nmol/L may be too low for safety and associated with higher all-cause mortality, demolishing the previously presumed U-shape curve of mortality associated with vitamin D levels. Since all-disease mortality is reduced to 1.0 with serum vitamin D levels ≥100 nmol/L, we call public health authorities to consider designating as the RDA at least three-fourths of the levels proposed by the Endocrine Society Expert Committee as safe upper tolerable daily intake doses. This could lead to a recommendation of 1000 IU for children <1 year on enriched formula and 1500 IU for breastfed children older than 6 months, 3000 IU for children >1 year of age, and around 8000 IU for young adults and thereafter. Actions are urgently needed to protect the global population from vitamin D deficiency.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5541280/
Re: Vitamin D: Scientific Studies & News
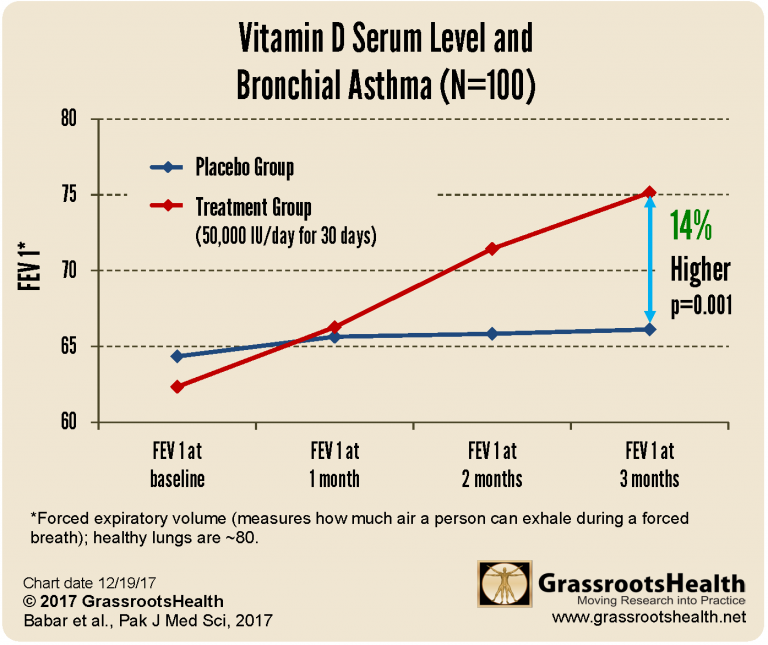
Controlling Asthma with Daily, High-Dose Vitamin D
A case control study using 100 patients in a private clinic in Pakistan found that vitamin D improved FEV1 measurements for asthmatics within two months, and even more by three months.
https://grassrootshealth.net/blog/contr ... vitamin-d/
Re: Vitamin D: Scientific Studies & News
Efficacy and safety outcomes in vitamin D supplement users in the fingolimod phase 3 trials.
Abstract
BACKGROUND:
Low serum levels of 25-hydroxyvitamin D have been associated with worse outcomes in multiple sclerosis (MS) patients treated with interferon-beta. Association of vitamin D nutrition on the outcomes of other MS therapies has been studied less.
OBJECTIVE:
Whether patients in the phase 3 fingolimod trials using vitamin D supplements have better clinical, MRI and safety outcomes than non-users.
MATERIALS AND METHODS:
Pooled data from phase 3 FREEDOMS trials was analyzed post hoc. Vitamin D use was defined as 'non-users' (n = 562), 'casual users' (n = 157) and 'daily users' (usage 100% time in the study, n = 110).
RESULTS:
Expanded Disability Status Scale change from baseline to month 24, and annual relapse rate and proportion of patients with relapses were similar across the vitamin D user groups. Proportion of patients free of new/enlarging T2 lesions significantly favored vitamin D 'daily users' versus 'non-users'. Mean number of lesions were lower and proportion of patients free of gadolinium-enhanced T1-lesions were higher in the 'daily users'. At month 12, percent brain volume change was significantly lower in the 'daily users' versus 'non-users' and remained low at month 24 (non-significant). Incidence of depression was lower for vitamin D 'daily users' (non-significant).
CONCLUSIONS:
We observed improved MRI outcomes on percent brain volume change and proportion of patients free of new/enlarging T2 lesions, and a trend of less depression in the 'daily users' of vitamin D supplement in patients in the FREEDOMS trials.
https://www.ncbi.nlm.nih.gov/pubmed/29243005
Re: Vitamin D: Scientific Studies & News
Association between vitamin D receptor polymorphisms and systemic lupus erythematosus in an Indian cohort.
Abstract
AIM:
Systemic lupus erythematosus (SLE) is an autoimmune disorder with various clinical manifestations. Susceptibility to development of SLE has been linked to several factors, such as genetic, environmental and hormonal. Vitamin D appears to have a regulatory role on disease manifestation and activity. Vitamin D exerts its effect through vitamin D receptors (VDR). Several studies have demonstrated an association between VDR polymorphisms and susceptibility to SLE in different populations, although the results are still inconclusive. In the present study, we investigated the association of VDR polymorphisms with SLE in a cohort of patients from Odisha, India.
METHODS:
Female SLE patients (n = 331) who fulfilled the revised American College of Rheumatology classification criteria were enrolled along with 282 healthy controls from similar geographical areas. VDR polymorphisms (BsmI, ApaI, TaqI and FokI) were typed by polymerase chain reaction followed by restriction fragment length polymorphism. Plasma level of 25-OH vitamin D was quantified by enzyme-linked immunosorbent assay.
RESULTS:
Prevalence of FokI (Ff) and TaqI (Tt) heterozygotes were significantly higher in SLE patients compared to healthy controls (Ff: P < 0.0001, odds ratio [OR] = 2.80, 95%CI = 1.99-3.95; Tt: P < 0.0001, OR = 2.07, 95%CI = 1.49-2.89). Furthermore, the minor alleles of FokI (f) and TaqI (t) polymorphisms were also more frequent in SLE patients than healthy controls (f: P < 0.0001, OR = 1.96, 95%CI = 1.52-2.52; t: P = 0.0002, OR = 1.60, 95%CI = 1.25-2.09).
CONCLUSIONS:
FokI and TaqI variants are significantly associated with SLE in an eastern Indian cohort. The cause-effect relationship can be assessed from the combined analyses of VDR polymorphism, plasma vitamin D levels and clinical manifestations.
https://www.ncbi.nlm.nih.gov/pubmed/29230954
Re: Vitamin D: Scientific Studies & News
1,25-Dihydroxyvitamin-D3 induces brain proteomic changes in cuprizone mice during remyelination involving calcium proteins.
Abstract
Dietary supplementation of vitamin D is commonly recommended to patients with multiple sclerosis. We recently found that high-dose of the hormonally active 1,25-dihydroxyvitamin-D3 (1,25D) promotes myelin repair in the cuprizone model for de- and remyelination. In the present study, we quantified 5062 proteins, of which 125 were differentially regulated in brain tissue from 1,25D treated mice during remyelination, compared to placebo. Proteins upregulated in the early remyelination phase were involved in calcium binding, e.g. calretinin (>1.3 fold, p < 0.005), S10A5 and secretagogin, and involved in mitochondrial function, e.g. NADH-ubiquinone oxidoreductase chain 3, and acyl-coenzyme A synthetase. Calretinin, S10A5 and secretagogin expression levels were characterized using immunohistochemistry. Calretinin immunoreactivity was significantly increased (>3 fold, p = 0.016) in the medial septal nuclei of 1,25D treated mice in the early remyelination phase. Our results indicate that vitamin D may influence remyelination by mechanisms involving an increase in calretinin expression and potentially other calcium binding proteins.
https://www.ncbi.nlm.nih.gov/pubmed/28818673
Re: Vitamin D: Scientific Studies & News
The association between vitamin D receptor polymorphisms and multiple sclerosis in a Turkish population.
Abstract
BACKGROUND:
Multiple sclerosis (MS) is a chronic, demyelinating disease of the central nervous system (CNS). Genetic and environmental factors are important in disease development. Many studies have investigated the relationship between MS and VDR polymorphisms. VDR gene polymorphism has not been previously studied in Turkish MS patients. We aimed to investigate the relationship between MS and VDR genotypes Taq I, Apa I and Fok I polymorphisms in a Turkish population.
METHODS:
167 MS patients and 146 healthy control subjects were included in the present study. MS and the VDR TaqI (rs731236), ApaI (rs7975232), and FokI (rs2228570) polymorphisms were investigated.
RESULTS:
The study enrolled 167 patients (121 females, 46 males) with MS and 146 healthy individuals (88 females, 58 males). The frequency of only the Fok I polymorphism differed significantly between the two groups (p = 0.002). The TaqI (rs731236) and ApaI (rs7975232) genotype distributions were not significantly different between MS patients and healthy controls (p = 0.626 and p = 0.990, respectively). Also there were no significant gender difference between patients and controls for Taq I and Apa I.
CONCLUSION:
In conclusion, we found a significant association between MS and the FokI polymorphism in our region of Turkey. However, the results may be different in other populations. More epidemiological and genetic studies are needed to explain the association between genetic factors and MS.
https://www.ncbi.nlm.nih.gov/pubmed/29331875